Dependence of acetylcholine and ADP dilation of pial arterioles on heme oxygenase after transfusion of cell-free polymeric hemoglobin
- PMID: 16214847
- PMCID: PMC1827797
- DOI: 10.1152/ajpheart.00500.2005
Dependence of acetylcholine and ADP dilation of pial arterioles on heme oxygenase after transfusion of cell-free polymeric hemoglobin
Abstract
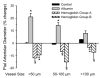
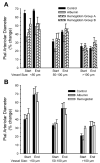
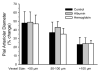
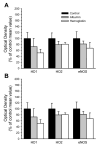
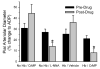
Polymers of cell-free hemoglobin have been designed for clinical use as oxygen carriers, but limited information is available regarding their effects on vascular regulation. We tested the hypothesis that the contribution of heme oxygenase (HO) to acetylcholine-evoked dilation of pial arterioles is upregulated 2 days after polymeric hemoglobin transfusion. Dilator responses to acetylcholine measured by intravital microscopy in anesthetized cats were blocked by superfusion of the HO inhibitor tin protoporphyrin-IX (SnPPIX) in a group that had undergone exchange transfusion with hemoglobin 2 days earlier but not in surgical sham and albumin-transfused groups. However, immunoblots from cortical brain homogenates did not reveal changes in expression of the inducible isoform HO1 or the constitutive isoform HO2 in the hemoglobin-transfused group. To test whether the inhibitory effect of SnPPIX was present acutely after hemoglobin transfusion, responses were measured within an hour of completion of the exchange transfusion. In control and albumin-transfused groups, acetylcholine responses were unaffected by SnPPIX but were blocked by addition of the nitric oxide synthase inhibitor N(omega)-nitro-l-arginine (l-NNA) to the superfusate. In hemoglobin-transfused groups, the acetylcholine response was blocked by either SnPPIX or l-NNA alone. The effect of another HO inhibitor, chromium mesoporphyrin (CrMP), was tested on ADP, another endothelial-dependent dilator, in anesthetized rats. Pial arteriolar dilation to ADP was unaffected by CrMP in controls but was attenuated 62% by CrMP in rats transfused with hemoglobin. It is concluded that 1) polymeric hemoglobin transfusion acutely upregulates the contribution of HO to acetylcholine-induced dilation of pial arterioles in cats, 2) this upregulation persists 2 days after transfusion when 95% of the hemoglobin is cleared from the circulation, and 3) this acute upregulation of HO signaling is ubiquitous in that similar effects were observed with a different endothelial-dependent agonist (i.e., ADP) in a another species (rat).
Figures


Similar articles
-
Endothelin rather than 20-HETE contributes to loss of pial arteriolar dilation during focal cerebral ischemia with and without polymeric hemoglobin transfusion.Am J Physiol Regul Integr Comp Physiol. 2009 May;296(5):R1412-8. doi: 10.1152/ajpregu.00003.2009. Epub 2009 Mar 4. Am J Physiol Regul Integr Comp Physiol. 2009. PMID: 19261918 Free PMC article.
-
Role of heme oxygenase-2 in pial arteriolar response to acetylcholine in mice with and without transfusion of cell-free hemoglobin polymers.Am J Physiol Regul Integr Comp Physiol. 2008 Aug;295(2):R498-504. doi: 10.1152/ajpregu.00188.2008. Epub 2008 May 21. Am J Physiol Regul Integr Comp Physiol. 2008. PMID: 18495834 Free PMC article.
-
Sustained endothelial dependent dilation in pial arterioles after crosslinked hemoglobin transfusion.Artif Cells Blood Substit Immobil Biotechnol. 1997 Jan-Mar;25(1-2):115-20. doi: 10.3109/10731199709118903. Artif Cells Blood Substit Immobil Biotechnol. 1997. PMID: 9083632
-
Effect of cross-linked hemoglobin transfusion on endothelial-dependent dilation in cat pial arterioles.Am J Physiol. 1998 Oct;275(4):H1313-21. doi: 10.1152/ajpheart.1998.275.4.H1313. Am J Physiol. 1998. PMID: 9746481
-
Carbon monoxide as an endogenous vascular modulator.Am J Physiol Heart Circ Physiol. 2011 Jul;301(1):H1-H11. doi: 10.1152/ajpheart.00230.2011. Epub 2011 Apr 15. Am J Physiol Heart Circ Physiol. 2011. PMID: 21498777 Free PMC article. Review.
Cited by
-
Exposure to Blast Overpressure Impairs Cerebral Microvascular Responses and Alters Vascular and Astrocytic Structure.J Neurotrauma. 2019 Nov 15;36(22):3138-3157. doi: 10.1089/neu.2019.6423. Epub 2019 Jul 31. J Neurotrauma. 2019. PMID: 31210096 Free PMC article.
-
Effects of the Oxygen-Carrying Solution OxyVita C on the Cerebral Microcirculation and Systemic Blood Pressures in Healthy Rats.J Funct Biomater. 2014 Nov 18;5(4):246-58. doi: 10.3390/jfb5040246. J Funct Biomater. 2014. PMID: 25411852 Free PMC article.
-
Endothelin rather than 20-HETE contributes to loss of pial arteriolar dilation during focal cerebral ischemia with and without polymeric hemoglobin transfusion.Am J Physiol Regul Integr Comp Physiol. 2009 May;296(5):R1412-8. doi: 10.1152/ajpregu.00003.2009. Epub 2009 Mar 4. Am J Physiol Regul Integr Comp Physiol. 2009. PMID: 19261918 Free PMC article.
-
Cerebral Microvascular and Systemic Effects Following Intravenous Administration of the Perfluorocarbon Emulsion Perftoran.J Funct Biomater. 2016 Nov 18;7(4):29. doi: 10.3390/jfb7040029. J Funct Biomater. 2016. PMID: 27869709 Free PMC article.
-
Regulation of the Cerebral Circulation During Development.Compr Physiol. 2021 Sep 23;11(4):2371-2432. doi: 10.1002/cphy.c200028. Compr Physiol. 2021. PMID: 34558670 Free PMC article.
References
-
- Appleton SD, Chretien ML, McLaughlin BE, Vreman HJ, Stevenson DK, Brien JF, Nakatsu K, Maurice DH, Marks GS. Selective inhibition of heme oxygenase, without inhibition of nitric oxide synthase or soluble guanylyl cyclase, by metalloporphyrins at low concentrations. Drug Metab Dispos. 1999;27:1214–1219. - PubMed
-
- Appleton SD, Marks GS, Nakatsu K, Brien JF, Smith GN, Graham CH. Heme oxygenase activity in placenta: direct dependence on oxygen availability. Am J Physiol Heart Circ Physiol. 2002;282:H2055–H2059. - PubMed
-
- Asano Y, Koehler RC, Ulatowski JA, Traystman RJ, Bucci E. Effect of crosslinked hemoglobin transfusion on endothelial dependent dilation in feline pial arterioles. Am J Physiol Heart Circ Physiol. 1998;275:H1313–H1321. - PubMed
-
- Balla J, Nath KA, Balla G, Juckett MB, Jacob HS, Vercellotti GM. Endothelial cell heme oxygenase and ferritin induction in rat lung by hemoglobin in vivo. Am J Physiol Lung Cell Mol Physiol. 1995;268:L321–L327. - PubMed
-
- Barkoudah E, Jaggar JH, Leffler CW. The permissive role of endothelial NO in CO-induced cerebrovascular dilation. Am J Physiol Heart Circ Physiol. 2004;287:H1459–H1465. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

