Quinolone efflux pumps play a central role in emergence of fluoroquinolone resistance in Streptococcus pneumoniae
- PMID: 16377702
- PMCID: PMC1346791
- DOI: 10.1128/AAC.50.1.310-317.2006
Quinolone efflux pumps play a central role in emergence of fluoroquinolone resistance in Streptococcus pneumoniae
Abstract
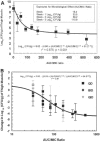
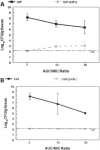
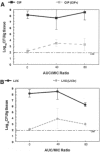
The preferential use of older antimicrobial agents is, in general, sound public health policy and is meant to maintain susceptibility to newer agents. In the case of fluoroquinolones, however, this strategy is flawed and may actually hasten the spread of Streptococcus pneumoniae strains resistant to newer members of the class. In a mouse thigh infection model, we were unable to isolate clones of pneumococci resistant to the newer fluoroquinolone levofloxacin at 2 x or 4 x the baseline MIC. An initial exposure in vivo to the older agent, ciprofloxacin, allowed straightforward selection of clones resistant to levofloxacin in a subsequent experiment. The original ciprofloxacin exposure generated clones without changes in the parC/E and gyrA/B quinolone target sites almost exclusively but did allow overexpression of a reserpine-responsive pump. While this caused only minimal change in the levofloxacin MIC (0.6 mg/liter to 0.8 mg/liter), it allowed a major change in the mutational frequency to resistance for levofloxacin (<1/10(8.5) to approximately 1/10(4.5)), which allowed levofloxacin-resistant clones to be isolated in a subsequent in vivo experiment. The reason underlying ciprofloxacin's propensity to select for pump-overexpressed clones is likely related to its hydrophilicity. To preserve the susceptibility of Streptococcus pneumoniae to newer members of the class of quinolones, use of ciprofloxacin for community-acquired respiratory infections should be minimized.
Figures

References
-
- Bartlett, J. G., R. F. Breiman, L. A., Mandell, and T. M. File, Jr. 1998. Community-acquired pneumonia in adults: guidelines for management. Clin. Infect. Dis. 26:811-838. - PubMed
-
- Chen, D. K., A. McGeer, J. C. de Azavedo, and D. E Low. 1999. Decreased susceptibility of Streptococcus pneumoniae to fluoroquinolones in Canada. N. Engl. J. Med. 341:233-239. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

