Cerebral hemodynamics in Moyamoya disease: correlation between perfusion-weighted MR imaging and cerebral angiography
- PMID: 16484417
- PMCID: PMC8148755
Cerebral hemodynamics in Moyamoya disease: correlation between perfusion-weighted MR imaging and cerebral angiography
Abstract
Background and purpose: In Moyamoya disease, the relationship between cerebral hemodynamics and angiographic findings has not been fully evaluated. The purpose of this study is to evaluate hemodynamics in Moyamoya disease with perfusion-weighted MR imaging (PWI) and cerebral angiography.
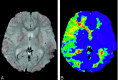
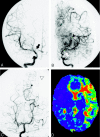
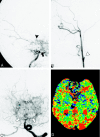
Methods: Twenty patients with Moyamoya disease were the subjects. Mean transit time (MTT) derived from PWI was calculated in the medial frontal lobes, the posterior frontal lobes, the occipital lobes, and the basal ganglia. From the angiographies, we classified the degrees of internal carotid artery (ICA) and posterior cerebral artery (PCA) stenoses as well as the degrees of Moyamoya vessels and leptomeningeal anastomosis (LMA). MTT in each region was compared with the angiographic findings.
Results: MTT positively correlated with the degree of ICA stenosis in the medial frontal (P < .01), posterior frontal (P < .001), and occipital (P < .001) lobes, as well as in the basal ganglia (P < .001). MTT correlated with the degree of PCA stenosis in the medial frontal (P < .001), posterior frontal (P < .001), and occipital (P < .001) lobes, as well as in the basal ganglia (P < .001). MTT correlated with the degree of Moyamoya vessels in the medial frontal (P < .05) and posterior frontal (P < .01) lobes. A multivariate analysis revealed that ICA and PCA stenoses and Moyamoya vessels were independent factors that prolonged MTT.
Conclusion: Both ICA and PCA stenoses may influence overall cerebral perfusion in Moyamoya disease. The development of Moyamoya vessels may indicate hemodynamic impairment.
Figures
Similar articles
-
Perfusion-weighted magnetic resonance imaging used in assessing hemodynamics following superficial temporal artery-middle cerebral artery bypass in patients with Moyamoya disease.Cerebrovasc Dis. 2013;35(5):455-60. doi: 10.1159/000350197. Epub 2013 May 31. Cerebrovasc Dis. 2013. PMID: 23735877 Clinical Trial.
-
Cerebral hemodynamics and oxygen metabolism in patients with moyamoya syndrome associated with atherosclerotic steno-occlusive arterial lesions.Cerebrovasc Dis. 2008;26(1):9-15. doi: 10.1159/000135647. Epub 2008 May 30. Cerebrovasc Dis. 2008. PMID: 18511866
-
Changing Ischemic Lesion Patterns and Hemodynamics of the Posterior Cerebral Artery in Moyamoya Disease.J Ultrasound Med. 2019 Oct;38(10):2621-2630. doi: 10.1002/jum.14959. Epub 2019 Jan 31. J Ultrasound Med. 2019. PMID: 30702756
-
[A case of adult moyamoya disease showing fulminant clinical course associated with progression from unilateral to bilateral involvement].No Shinkei Geka. 1997 Jan;25(1):79-84. No Shinkei Geka. 1997. PMID: 8990473 Review. Japanese.
-
Quantitative hemodynamic studies in moyamoya disease: a review.Neurosurg Focus. 2009 Apr;26(4):E5. doi: 10.3171/2009.1.FOCUS08300. Neurosurg Focus. 2009. PMID: 19335131 Free PMC article. Review.
Cited by
-
Cerebral Ischemic Complications of Surgical Treatment in Patients with Moyamoya Disease.Acta Neurochir Suppl. 2025;136:85-91. doi: 10.1007/978-3-031-89844-0_10. Acta Neurochir Suppl. 2025. PMID: 40632257
-
Correlation between collateral compensation of the posterior cerebral artery on 5 T magnetic resonance imaging and clinical classifications in patients with Moyamoya angiopathy.Jpn J Radiol. 2025 Aug;43(8):1286-1294. doi: 10.1007/s11604-025-01784-8. Epub 2025 Apr 16. Jpn J Radiol. 2025. PMID: 40238043
-
Quantitative Digital Subtraction Angiography in Pediatric Moyamoya Disease.J Korean Neurosurg Soc. 2015 Jun;57(6):432-5. doi: 10.3340/jkns.2015.57.6.432. Epub 2015 Jun 30. J Korean Neurosurg Soc. 2015. PMID: 26180611 Free PMC article. Review.
-
Application of CT perfusion to assess hemodynamics in symptomatic Moyamoya syndrome: focus on affected side and parameter characteristic.Childs Nerv Syst. 2018 Jun;34(6):1189-1197. doi: 10.1007/s00381-018-3727-8. Epub 2018 Jan 27. Childs Nerv Syst. 2018. PMID: 29374799
-
Research Progress of Moyamoya Disease in Children.Int J Med Sci. 2015 Jul 3;12(7):566-75. doi: 10.7150/ijms.11719. eCollection 2015. Int J Med Sci. 2015. PMID: 26180513 Free PMC article. Review.
References
-
- Suzuki J, Takaku A. Cerebrovascular “moyamoya” disease: disease showing abnormal net-like vessels in base of brain. Arch Neurol 1969;20:288–99 - PubMed
-
- Suzuki J, Kodama N. Moyamoya disease: a review. Stroke 1983;14:104–10 - PubMed
-
- Nishimoto A, Takeuchi S. Abnormal cerebrovascular network related to the internal carotid arteries. J Neurosurg 1968;29:255–60 - PubMed
-
- Miyamoto S, Kikuchi H, Karasawa J, et al. Study of the posterior circulation in moyamoya disease: clinical and neuroradiological evaluation. J Neurosurg 1984;61:1032–37 - PubMed
-
- Yamada I, Himeno Y, Suzuki S, et al. Posterior circulation in moyamoya disease: angiographic study. Radiology 1995;197:239–46 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous
