Osteogenic protein-1 (BMP-7) accelerates healing of scaphoid non-union with proximal pole sclerosis
- PMID: 16506027
- PMCID: PMC2532081
- DOI: 10.1007/s00264-005-0045-z
Osteogenic protein-1 (BMP-7) accelerates healing of scaphoid non-union with proximal pole sclerosis
Abstract
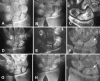
We randomly assigned 17 patients with scaphoid non-union at the proximal pole to three treatment groups: (1) autologous iliac graft (n=6), (2) autologous iliac graft + osteogenic protein-1 (OP-1; n=6), and (3) allogenic iliac graft + OP-1 (n=5). Radiographic, scintigraphic, and clinical assessments were performed throughout the follow-up period of 24 months. OP-1 improved the performance of both autologous and allogenic bone implants and reduced radiographic healing time to 4 weeks compared with 9 weeks in group 1. Helical CT scans and scintigraphy showed that in OP-1-treated patients sclerotic bone was replaced by well-vascularised bone. The addition of OP-1 to allogenic bone implant equalised the clinical outcome with the autologous graft procedure. Consequently the harvesting of autologous graft can be avoided.
Nous avons réparti 17 malades avec une pseudarthrose du pôle proximal du scaphoide en trois groupes aléatoires de traitement: (1) greffe autologue iliaque (n=6), (2) greffe autologue iliaque + protéine osteogenique-1 (OP-1; n=6), et (3) greffe allogène iliaque + OP-1 (n=5). L’estimation radiographique, scintigraphique et clinique a été exécutée pendant une période de suivi de 24 mois. L’OP-1 a amélioré la performance des autogreffes et des allogreffes osseuses et a réduit le temps curatif radiographique à 4 semaines, comparé à 9 semaines dans le groupe traité uniquement avec de l’os autologues. Chez les malades traités avec l’OP-1, la tomodensitométrie hélicoïdale et la scintigraphie ont montré que l’os scléreux était remplacé par de l’os bien vascularisé. L’addition d’OP-1 à la greffe allogène a égalisé le résultat clinique avec la procédure de greffe autologue et a permis de supprimer le temps de prise de greffe.
Figures

References
-
- Bilic R, Korzinek K (1987) Results of scaphoid non-union treatment by Matti-Russe procedure using compressed cancellous bone. Unfallchirurg 90:134–138 - PubMed
-
- Burkus JK, Gornet MF, Dickman CA, Zdeblick TA (2002) Anterior lumbar interbody fusion using rhBMP-2 with tapered interbody cages. J Spinal Disord Tech 15:337–349 - PubMed
-
- Cook SD, Rueger DC (2002) Preclinical models of recombinant BMP induced healing of orthopedic defects. In: Vukicevic S, Sampath K (eds) Bone morphogenetic proteins: from laboratory to clinical practice. Birkhäuser, Basel, pp 121–144
-
- Fisk GR (1984) The wrist. J Bone Joint Surg Br 66:396–407 - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

