Acute psychiatric admissions from an out-of-hours Casualty Clinic; how do referring doctors and admitting specialists agree?
- PMID: 16571113
- PMCID: PMC1552062
- DOI: 10.1186/1472-6963-6-41
Acute psychiatric admissions from an out-of-hours Casualty Clinic; how do referring doctors and admitting specialists agree?
Abstract
Background: Over the last decades there has been an increasing pressure on the acute psychiatric wards in Norway. The major contributor to psychiatric acute admissions at the University Hospital of North Norway in the city of Tromsø in 2001 was the GP-based Tromsø Casualty Clinic, only open out-of-hours. We explored all acute psychiatric referrals from Tromsø Casualty Clinic in 2001. The purpose of the study was to characterize the admissions and assess the agreement between the referring doctors and the hospital specialists according to the need for hospitalization, agreement on application of the law and the diagnostic evaluation to assess whether the admissions were appropriate.
Methods: Retrospective, record based, descriptive study comprising 101 psychiatric acute referrals from the Tromsø Casualty Clinic to the psychiatric acute wards at the University Hospital of North Norway.
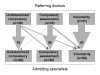
Results: The specialists accepted all referrals except one, they mostly agreed upon the diagnoses suggested by the referring doctors and they mostly confirmed the application of the law.Seventy-five percent of the admissions took place during weekends, public holidays or nighttimes. Diagnoses of psychoses or suicidal attempts accounted for 76 % of the total referrals. Substance abuse was noted for 43 %, and in 22 % of all admissions the patients had stopped taking their psychopharmacological medication. The police assisted the referring doctors in one third of all admissions, and was the legal representative in 52 out of 59 involuntary admissions. Thirty percent of the admissions were first- time admissions. Thirty-two percent of the hospital stays lasted for three days or less. Median length of stay was 6.5 days.
Conclusion: The casualty clinic physicians and the hospital specialists mostly agreed in their evaluation of patients indicating that most of the admissions were appropriate. The police was more often involved in the involuntary admissions than intended in the law. The proportion of patients with substance abuse was significant. Alternative treatment strategies should be developed for non-psychotic patients in need of short-term stays.
Figures
Similar articles
-
Differential use of admission status in a psychiatric emergency room.Bull Am Acad Psychiatry Law. 1995;23(4):595-606. Bull Am Acad Psychiatry Law. 1995. PMID: 8639987
-
Possible criteria for inpatient psychiatric admissions: which patients are transferred from emergency services to inpatient psychiatric treatment?BMC Health Serv Res. 2006 Nov 22;6:150. doi: 10.1186/1472-6963-6-150. BMC Health Serv Res. 2006. PMID: 17121672 Free PMC article.
-
Predictors of involuntary hospitalizations to acute psychiatry.Int J Law Psychiatry. 2013 Mar-Apr;36(2):136-43. doi: 10.1016/j.ijlp.2013.01.006. Epub 2013 Feb 8. Int J Law Psychiatry. 2013. PMID: 23395506
-
[Dichotomy of psychiatric and somatic emergency care; fundamental flaw should be addressed].Ned Tijdschr Geneeskd. 2015;159:A9151. Ned Tijdschr Geneeskd. 2015. PMID: 26230348 Review. Dutch.
-
[Emergency psychiatry in Belgium; a challenge for the mental health services].Tijdschr Psychiatr. 2008;50 Spec no.:35-9. Tijdschr Psychiatr. 2008. PMID: 19067298 Review. Dutch.
Cited by
-
Local psychiatric beds appear to decrease the use of involuntary admission: a case-registry study.BMC Health Serv Res. 2014 Feb 10;14:64. doi: 10.1186/1472-6963-14-64. BMC Health Serv Res. 2014. PMID: 24506810 Free PMC article.
-
Involuntary admission and treatment of patients with mental disorder.Neurosci Bull. 2015 Feb;31(1):99-112. doi: 10.1007/s12264-014-1493-5. Epub 2015 Jan 16. Neurosci Bull. 2015. PMID: 25595369 Free PMC article. Review.
-
Involuntary psychiatric admission: how the patients are detected and the general practitioners' expectations for hospitalization. An interview-based study.Int J Ment Health Syst. 2016 Mar 8;10:20. doi: 10.1186/s13033-016-0048-8. eCollection 2016. Int J Ment Health Syst. 2016. PMID: 26958076 Free PMC article.
-
Contacts related to mental illness and substance abuse in primary health care: a cross-sectional study comparing patients' use of daytime versus out-of-hours primary care in Norway.Scand J Prim Health Care. 2010 Sep;28(3):160-5. doi: 10.3109/02813432.2010.493310. Scand J Prim Health Care. 2010. PMID: 20575649 Free PMC article.
-
Involuntary admission in Norwegian adult psychiatric hospitals: a systematic review.Int J Ment Health Syst. 2018 Mar 22;12:10. doi: 10.1186/s13033-018-0189-z. eCollection 2018. Int J Ment Health Syst. 2018. PMID: 29588656 Free PMC article. Review.
References
-
- Hansen V. Psychiatric service within primary care. Mode of organization and influence on admission-rates to a mental hospital. Acta Psychiatr Scand. 1987;76(2):121–128. - PubMed
-
- Hansen V, Oiesvold T. Community psychiatry in the sub-arctic. Experiences with the shift from hospital-based to community-based psychiatric services in Northern Norway. Epidemiol Psichiatr Soc. 2004;13:73–77. - PubMed
-
- Norway S. [Beds in psychiatric institutions and departments] 2005. http://www.ssb.no/emner/03/02/speshelsepsyk/arkiv/tab-2002-09-18-01.html
-
- Munizza C, Furlan PM, d'Elia A, D'Onofrio MR, Leggero P, Punzo F, Vidini N, Villari V. Emergency psychiatry: a review of the literature. Acta Psychiatr Scand Suppl. 1993;374:1–51. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical