Which inotrope for which baby?
- PMID: 16632650
- PMCID: PMC2672709
- DOI: 10.1136/adc.2005.071829
Which inotrope for which baby?
Abstract
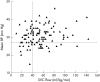
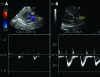
While we know a lot about blood pressure (BP) responses to various inotropes and a bit about systemic and organ blood flow responses, we know almost nothing about how different inotropes affect clinical outcomes. Low systemic blood flow (SBF) is common in the first 24 h after birth in very preterm babies (and more mature babies with severe respiratory problems) and is not always reflected by low BP. The causes of this low SBF are complex but may relate to maladaptation to high extrauterine systemic (and sometimes pulmonary) vascular resistance. After day 1, hypotensive babies are more likely to have normal or high SBF reflecting vasodilatation. Empirically, inotropes that reduce afterload (such as dobutamine) may be more appropriate in the transitional period, while those with more vasoconstrictor actions (such as dopamine) may be more appropriate later on. Defining the haemodynamic in an individual baby needs both BP and echocardiographic measures of SBF. Research in this area needs to move beyond just demonstrating changes in physiological variables to showing improvements in important clinical outcomes.
Conflict of interest statement
Competing interests: none declared
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical