Intestinal strongyloidiasis and hyperinfection syndrome
- PMID: 16734908
- PMCID: PMC1538622
- DOI: 10.1186/1476-7961-4-8
Intestinal strongyloidiasis and hyperinfection syndrome
Abstract
In spite of recent advances with experiments on animal models, strongyloidiasis, an infection caused by the nematode parasite Strongyloides stercoralis, has still been an elusive disease. Though endemic in some developing countries, strongyloidiasis still poses a threat to the developed world. Due to the peculiar but characteristic features of autoinfection, hyperinfection syndrome involving only pulmonary and gastrointestinal systems, and disseminated infection with involvement of other organs, strongyloidiasis needs special attention by the physician, especially one serving patients in areas endemic for strongyloidiasis. Strongyloidiasis can occur without any symptoms, or as a potentially fatal hyperinfection or disseminated infection. Th2 cell-mediated immunity, humoral immunity and mucosal immunity have been shown to have protective effects against this parasitic infection especially in animal models. Any factors that suppress these mechanisms (such as intercurrent immune suppression or glucocorticoid therapy) could potentially trigger hyperinfection or disseminated infection which could be fatal. Even with the recent advances in laboratory tests, strongyloidiasis is still difficult to diagnose. But once diagnosed, the disease can be treated effectively with antihelminthic drugs like Ivermectin. This review article summarizes a case of strongyloidiasis and various aspects of strongyloidiasis, with emphasis on epidemiology, life cycle of Strongyloides stercoralis, clinical manifestations of the disease, corticosteroids and strongyloidiasis, diagnostic aspects of the disease, various host defense pathways against strongyloidiasis, and available treatment options.
Figures
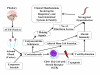
Similar articles
-
Is Strongyloides stercoralis hyperinfection induced by glucocorticoids a result of both suppressed host immunity and altered parasite genetics?Mol Biochem Parasitol. 2022 Sep;251:111511. doi: 10.1016/j.molbiopara.2022.111511. Epub 2022 Aug 22. Mol Biochem Parasitol. 2022. PMID: 36007683
-
Manifestations, diagnosis, and treatment of Strongyloides stercoralis infection.Ann Pharmacother. 2007 Dec;41(12):1992-2001. doi: 10.1345/aph.1K302. Epub 2007 Oct 16. Ann Pharmacother. 2007. PMID: 17940124 Review.
-
Strongyloides hyperinfection in a patient with solid malignant tumor a case report.Indian J Public Health. 2020 Jan-Mar;64(1):90-92. doi: 10.4103/ijph.IJPH_111_19. Indian J Public Health. 2020. PMID: 32189692
-
Strongyloides Hyperinfection Syndrome: A Curious Case of Asthma Worsened by Systemic Corticosteroids.Am J Case Rep. 2020 Dec 21;21:e925221. doi: 10.12659/AJCR.925221. Am J Case Rep. 2020. PMID: 33347427 Free PMC article.
-
Strongyloides stercoralis infection complicating the central nervous system.Handb Clin Neurol. 2013;114:229-34. doi: 10.1016/B978-0-444-53490-3.00017-0. Handb Clin Neurol. 2013. PMID: 23829913 Review.
Cited by
-
Strongyloides hyperinfection syndrome following resection of meningioma.BMJ Case Rep. 2012 Jun 15;2012:bcr2012006174. doi: 10.1136/bcr-2012-006174. BMJ Case Rep. 2012. PMID: 22717933 Free PMC article.
-
Ivermectin Treatment and Sanitation Effectively Reduce Strongyloides stercoralis Infection Risk in Rural Communities in Cambodia.PLoS Negl Trop Dis. 2016 Aug 22;10(8):e0004909. doi: 10.1371/journal.pntd.0004909. eCollection 2016 Aug. PLoS Negl Trop Dis. 2016. PMID: 27548286 Free PMC article.
-
Strongyloidiasis.Nat Rev Dis Primers. 2024 Jan 25;10(1):6. doi: 10.1038/s41572-023-00490-x. Nat Rev Dis Primers. 2024. PMID: 38272922 Review.
-
Disseminated Strongyloides stercoralis Infection Associated with Endogenous Hypercortisolism - A Case Report.Eur J Case Rep Intern Med. 2020 Apr 14;7(7):001509. doi: 10.12890/2020_001509. eCollection 2020. Eur J Case Rep Intern Med. 2020. PMID: 32665921 Free PMC article.
-
Rare Case of Strongyloides stercoralis Hyperinfection in a Greek Patient with Chronic Eosinophilia.Int J Prev Med. 2012 May;3(5):370-2. Int J Prev Med. 2012. PMID: 22708034 Free PMC article.
References
-
- Roman-Sanchez P, Pastor-Guzman A, Moreno-Guillen S, Igual-Adell R, Suner-Generoso S, Tornero-Estebanez C. High prevalence of Strongyloides stercoralis among farm workers on the Mediterranean coast of Spain: analysis of the predictive factors of infection in developed countries. Am J Trop Med Hyg. 2003;69:336–340. - PubMed
-
- Liu LX, Weller PF. Strongyloidiasis and other intestinal nematode infections. Infect Dis Clin North Am. 1993;7:655–682. - PubMed
-
- Schwartz RA, Tarlow MM. Strongyloidiasis. 2005.
LinkOut - more resources
Full Text Sources

