Morbidity and cost burden of methicillin-resistant Staphylococcus aureus in early onset ventilator-associated pneumonia
- PMID: 16808853
- PMCID: PMC1550967
- DOI: 10.1186/cc4934
Morbidity and cost burden of methicillin-resistant Staphylococcus aureus in early onset ventilator-associated pneumonia
Abstract
Introduction: To gain a better understanding of the clinical and economic outcomes associated with methicillin-resistant Staphylococcus aureus (MRSA) infection in patients with early onset ventilator-associated pneumonia (VAP), we retrospectively analyzed a multihospital US database to identify patients with VAP over a 24 month period (2002-2003).
Method: Data recorded included physiologic, laboratory, culture, and other clinical variables from 59 institutions. VAP was defined as new positive respiratory culture after at least 24 hours of mechanical ventilation (MV) and the presence of primary or secondary ICD-9-CM diagnosis codes of pneumonia. Outcomes measures included in-hospital morbidity and mortality for the population overall and after onset of VAP (duration of MV, intensive care unit [ICU] stay, in-hospital stay, and case mix and severity-adjusted operating cost). The overall cost was calculated at the hospital level using the Center for Medicare and Medicaid Services Cost/Charge Index for each calendar year.
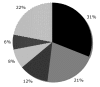
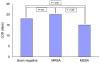
Results: A total of 499 patients were identified as having VAP. S. aureus was the leading organism (31% of isolates). Patients with MRSA were significantly older than patients with methicillin-sensitive Staphylococcus aureus (MSSA; median age 74 versus 67 years, P < 0.05) and more likely to be medical patients. Compared with MSSA patients, MRSA patients on average consumed excess resources of 4.4 (95% confidence interval 0.6-8.2) overall MV days, 3.8 (-0.5 to +8.0) days of inpatient length of stay (LOS), 5.3 (1.0-9.7) ICU days, and US7731 dollars (-US8393 dollars to +US23,856 dollars) total cost after controlling for case mix and other factors. Furthermore, MRSA patients needed excess resources after the onset of VAP (4.5 [95% confidence interval 1.0-8.1] MV days, 3.7 [-0.5 to +8.0] inpatient days, and 4.4 [0.4-8.4] ICU days) after controlling for the same case mix and admission severity covariates.
Conclusion: S. aureus remains a common cause of VAP. VAP due to MRSA was associated with increased overall LOS, ICU LOS, and attributable ICU LOS compared with MSSA-related VAP. Although not statistically significant because of small sample size and large variation, the attributable excess costs of MRSA amounted to approximately US8000 dollars per case after controlling for case mix and severity.
Figures
Comment in
-
Attributable cost of methicillin resistance: an issue that is difficult to evaluate.Crit Care. 2006;10(4):157. doi: 10.1186/cc4994. Crit Care. 2006. PMID: 16934109 Free PMC article. Review.
References
-
- Heyland DK, Cook DJ, Griffith L, Keenan SP, Brun-Buisson C. The attributable morbidity and mortality of ventilator-associated pneumonia in the critically ill patient. The Canadian Critical Trials Group. Am J Respir Crit Care Med. 1999;159:1249–1256. - PubMed
-
- Warren DK, Shukla SJ, Olsen MA, Kollef MH, Hollenbeak CS, Cox MJ, Cohen MM, Fraser VJ. Outcome and attributable cost of ventilator-associated pneumonia among intensive care unit patients in a suburban medical center. Crit Care Med. 2003;31:1312–1317. doi: 10.1097/01.CCM.0000063087.93157.06. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

