Disinhibition of the cardiac limb of the arterial baroreflex in rat: a role for metabotropic glutamate receptors in the nucleus tractus solitarii
- PMID: 16809369
- PMCID: PMC1995684
- DOI: 10.1113/jphysiol.2006.112672
Disinhibition of the cardiac limb of the arterial baroreflex in rat: a role for metabotropic glutamate receptors in the nucleus tractus solitarii
Abstract
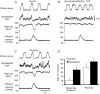
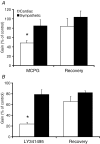
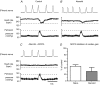
The nucleus tractus solitarii (NTS) is the first site of integration for primary baroreceptor afferents, which release glutamate to excite second-order neurones through ionotropic receptors. In vitro studies indicate that glutamate may also activate metabotropic receptors (mGluRs) to modulate the excitability of NTS neurones at pre- and postsynaptic loci. We examined the functional role of metabotropic glutamate receptors (mGluRs) in modulating the baroreceptor reflex in the rat NTS. Using the working heart-brainstem preparation, the baroreflex was activated using brief pressor stimuli and the consequent cardiac (heart rate change) and non-cardiac sympathetic (T8-10 chain) baroreflex gains were obtained. Microinjections of glutamate antagonists were made bilaterally into the NTS at the site of termination of baroreceptor afferents. NTS microinjection of kynurenate (ionotropic antagonist) inhibited both the cardiac and sympathetic baroreflex gains (16 +/- 5% and 59 +/- 11% of control, respectively). The non-selective mGluR antagonist MCPG produced a dose-dependent inhibition of the cardiac gain (30 +/- 3% of control) but not the sympathetic gain. Selective inhibitions of the cardiac gain were also seen with LY341495 and EGLU suggesting the response was mediated by group II mGluRs. This effect on cardiac gain involves attenuation of the parasympathetic baroreflex as it persists in the presence of atenolol. Prior NTS microinjection of bicuculline (GABA(A) antagonist) prevented the mGluR-mediated attenuation of the cardiac gain. These results are consistent with the reported presynaptic inhibition of GABAergic transmission by group II mGluRs in the NTS and constitute a plausible mechanism allowing selective feed-forward disinhibition to increase the gain of the cardiac limb of the baroreflex without changing the sympathoinhibitory component.
Figures



Similar articles
-
Antagonism of glutamatergic metabotropic receptors in the NTS of awake rats does not affect the gain of the baroreflex.Auton Neurosci. 2003 Jan 31;103(1-2):65-71. doi: 10.1016/s1566-0702(02)00234-5. Auton Neurosci. 2003. PMID: 12531399
-
Glutamate suppresses GABA release via presynaptic metabotropic glutamate receptors at baroreceptor neurones in rats.J Physiol. 2005 Jan 15;562(Pt 2):535-51. doi: 10.1113/jphysiol.2004.076885. Epub 2004 Nov 11. J Physiol. 2005. PMID: 15539399 Free PMC article.
-
Cardiovascular response to group I metabotropic glutamate receptor activation in NTS.Am J Physiol. 1999 May;276(5):R1469-78. doi: 10.1152/ajpregu.1999.276.5.R1469. Am J Physiol. 1999. PMID: 10233041
-
Serotonin2 receptors in the nucleus tractus solitarius: characterization and role in the baroreceptor reflex arc.Cell Mol Neurobiol. 2003 Oct;23(4-5):709-26. doi: 10.1023/a:1025096718559. Cell Mol Neurobiol. 2003. PMID: 14514026 Free PMC article. Review.
-
Neurotransmission of the cardiovascular reflexes in the nucleus tractus solitarii of awake rats.Ann N Y Acad Sci. 2001 Jun;940:179-96. doi: 10.1111/j.1749-6632.2001.tb03676.x. Ann N Y Acad Sci. 2001. PMID: 11458676 Review.
Cited by
-
Vanilloid, purinergic, and CCK receptors activate glutamate release on single neurons of the nucleus tractus solitarius centralis.Am J Physiol Regul Integr Comp Physiol. 2011 Aug;301(2):R394-401. doi: 10.1152/ajpregu.00054.2011. Epub 2011 May 4. Am J Physiol Regul Integr Comp Physiol. 2011. PMID: 21543639 Free PMC article.
-
A novel postsynaptic group II metabotropic glutamate receptor role in modulating baroreceptor signal transmission.J Neurosci. 2009 Sep 23;29(38):11807-16. doi: 10.1523/JNEUROSCI.2617-09.2009. J Neurosci. 2009. PMID: 19776267 Free PMC article.
-
Vagal afferent fibres determine the oxytocin-induced modulation of gastric tone.J Physiol. 2013 Jun 15;591(12):3081-100. doi: 10.1113/jphysiol.2013.253732. Epub 2013 Apr 15. J Physiol. 2013. PMID: 23587885 Free PMC article.
-
An exploration of the control of micturition using a novel in situ arterially perfused rat preparation.Front Neurosci. 2011 May 13;5:62. doi: 10.3389/fnins.2011.00062. eCollection 2011. Front Neurosci. 2011. PMID: 21625609 Free PMC article.
-
Chronic stimulation of group II metabotropic glutamate receptors in the medulla oblongata attenuates hypertension development in spontaneously hypertensive rats.PLoS One. 2021 May 19;16(5):e0251495. doi: 10.1371/journal.pone.0251495. eCollection 2021. PLoS One. 2021. PMID: 34010316 Free PMC article.
References
-
- Antunes VR, Machado BH. Antagonism of glutamatergic metabotropic receptors in the NTS of awake rats does not affect the gain of the baroreflex. Auton Neurosci. 2003;103:65–71. - PubMed
-
- Blessing W. The Lower Brainstem and Bodily Homeostasis. New York: Oxford University Press; 1997.
-
- Boscan P, Kasparov S, Paton JF. Somatic nociception activates NK1 receptors in the nucleus tractus solitarii to attenuate the baroreceptor cardiac reflex. Eur J Neurosci. 2002;16:907–920. - PubMed
-
- Boscan P, Paton JF. Role of the solitary tract nucleus in mediating nociceptive evoked cardiorespiratory responses. Auton Neurosci. 2001;86:170–182. - PubMed
-
- Chan R, Peto C, Sawchenko P. Fine structure and plasticity of barosensitive neurons in the nucleus of solitary tract. J Comp Neurol. 2000;422:338–351. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

