Pancreatic signals controlling food intake; insulin, glucagon and amylin
- PMID: 16815800
- PMCID: PMC1642707
- DOI: 10.1098/rstb.2006.1858
Pancreatic signals controlling food intake; insulin, glucagon and amylin
Abstract
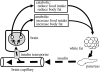
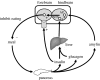
The control of food intake and body weight by the brain relies upon the detection and integration of signals reflecting energy stores and fluxes, and their interaction with many different inputs related to food palatability and gastrointestinal handling as well as social, emotional, circadian, habitual and other situational factors. This review focuses upon the role of hormones secreted by the endocrine pancreas: hormones, which individually and collectively influence food intake, with an emphasis upon insulin, glucagon and amylin. Insulin and amylin are co-secreted by B-cells and provide a signal that reflects both circulating energy in the form of glucose and stored energy in the form of visceral adipose tissue. Insulin acts directly at the liver to suppress the synthesis and secretion of glucose, and some plasma insulin is transported into the brain and especially the mediobasal hypothalamus where it elicits a net catabolic response, particularly reduced food intake and loss of body weight. Amylin reduces meal size by stimulating neurons in the hindbrain, and there is evidence that amylin additionally functions as an adiposity signal controlling body weight as well as meal size. Glucagon is secreted from A-cells and increases glucose secretion from the liver. Glucagon acts in the liver to reduce meal size, the signal being relayed to the brain via the vagus nerves. To summarize, hormones of the endocrine pancreas are collectively at the crossroads of many aspects of energy homeostasis. Glucagon and amylin act in the short term to reduce meal size, and insulin sensitizes the brain to short-term meal-generated satiety signals; and insulin and perhaps amylin as well act over longer intervals to modulate the amount of fat maintained and defended by the brain. Hormones of the endocrine pancreas interact with receptors at many points along the gut-brain axis, from the liver to the sensory vagus nerve to the hindbrain to the hypothalamus; and their signals are conveyed both neurally and humorally. Finally, their actions include gastrointestinal and metabolic as well as behavioural effects.
Figures
Similar articles
-
Inhibition of glucagon secretion.Adv Pharmacol. 2005;52:151-71. doi: 10.1016/S1054-3589(05)52008-8. Adv Pharmacol. 2005. PMID: 16492545 Review.
-
Central amylin signaling and the regulation of energy homeostasis.Curr Pharm Des. 2003;9(10):819-25. doi: 10.2174/1381612033455387. Curr Pharm Des. 2003. PMID: 12678881 Review.
-
Amylin receptor blockade stimulates food intake in rats.Am J Physiol Regul Integr Comp Physiol. 2004 Sep;287(3):R568-74. doi: 10.1152/ajpregu.00213.2004. Epub 2004 May 6. Am J Physiol Regul Integr Comp Physiol. 2004. PMID: 15130879
-
Afferent signals regulating food intake.Proc Nutr Soc. 2000 Aug;59(3):373-84. doi: 10.1017/s0029665100000422. Proc Nutr Soc. 2000. PMID: 10997653 Review.
-
[Amylin--a partner hormone to insulin].Med Arh. 2003;57(3):177-8. Med Arh. 2003. PMID: 12858660 Review. Croatian.
Cited by
-
Phosphatidylethanolamine enhances amyloid fiber-dependent membrane fragmentation.Biochemistry. 2012 Oct 2;51(39):7676-84. doi: 10.1021/bi3009888. Epub 2012 Sep 21. Biochemistry. 2012. PMID: 22970795 Free PMC article.
-
Membrane Curvature-sensing and Curvature-inducing Activity of Islet Amyloid Polypeptide and Its Implications for Membrane Disruption.J Biol Chem. 2015 Oct 23;290(43):25782-93. doi: 10.1074/jbc.M115.659797. Epub 2015 Aug 17. J Biol Chem. 2015. PMID: 26283787 Free PMC article.
-
Sex differences in the physiology of eating.Am J Physiol Regul Integr Comp Physiol. 2013 Dec;305(11):R1215-67. doi: 10.1152/ajpregu.00446.2012. Epub 2013 Jul 31. Am J Physiol Regul Integr Comp Physiol. 2013. PMID: 23904103 Free PMC article. Review.
-
Slc12a2 loss in insulin-secreting β-cells links development of overweight and metabolic dysregulation to impaired satiation control of feeding.Am J Physiol Endocrinol Metab. 2023 Nov 1;325(5):E581-E594. doi: 10.1152/ajpendo.00197.2023. Epub 2023 Oct 11. Am J Physiol Endocrinol Metab. 2023. PMID: 37819196 Free PMC article.
-
Autoantibodies against appetite-regulating peptide hormones and neuropeptides: putative modulation by gut microflora.Nutrition. 2008 Apr;24(4):348-59. doi: 10.1016/j.nut.2007.12.006. Epub 2008 Feb 8. Nutrition. 2008. PMID: 18262391 Free PMC article.
References
-
- Ahima R.S, Saper C.B, Flier J.S, Elmquist J.K. Leptin regulation of neuroendocrine systems. Front. Neuroendocrinol. 2000;21:263–307. doi:10.1006/frne.2000.0197 - DOI - PubMed
-
- Air E.L, Strowski M.Z, Benoit S.C, Conarello S.L, Salituro G.M, Guan X.M, Liu K, Woods S.C, Zhang B.B. Small molecule insulin mimetics reduce food intake and body weight and prevent development of obesity. Nat. Med. 2002;8:179–183. doi:10.1038/nm0202-179 - DOI - PubMed
-
- Anika S.M, Houpt T.L, Houpt K.A. Insulin as a satiety hormone. Physiol. Behav. 1980;25:21–23. doi:10.1016/0031-9384(80)90175-4 - DOI - PubMed
-
- Arase K, Fisler J.S, Shargill N.S, York D.A, Bray G.A. Intracerebroventricular infusions of 3-OHB and insulin in a rat model of dietary obesity. Am. J. Physiol. 1988;255:R974–R981. - PubMed
-
- Arnelo U, Blevins J.E, Larsson J, Permert J, Westermark P, Reidelberger R.D, Adrian T.E. Effects of acute and chronic infusion of islet amyloid polypeptide on food intake in rats. Scand. J. Gastroenterol. 1996a;31:83–89. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

