Proximal gastric response to small intestinal nutrients is abnormal in mechanically ventilated critically ill patients
- PMID: 16865782
- PMCID: PMC4087751
- DOI: 10.3748/wjg.v12.i27.4383
Proximal gastric response to small intestinal nutrients is abnormal in mechanically ventilated critically ill patients
Abstract
Aim: To determine the response of the proximal stomach to small intestinal nutrients in critically ill patients.
Methods: Proximal gastric motility was measured in 13 critically ill patients (49.3 +/- 4.7 years) and 12 healthy volunteers (27.7 +/- 2.9 years) using a barostat technique. Recordings were performed at baseline, during a 60-min intra-duodenal infusion of Ensure (2 kcal/min), and for 2 h following the infusion. Minimum distending pressure (MDP), intra-bag volume and fundic wave activity were determined.
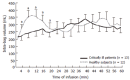
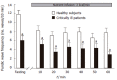
Results: The MDP was higher in patients (11.7 +/- 1.1 vs 7.8 +/- 0.7 mmHg; P < 0.01). Baseline intra-bag volumes were similar in the 2 groups. In healthy subjects, a 'bimodal' proximal gastric volume response was observed. In patients, the initial increase in proximal gastric volume was small and delayed, but eventually reached a maximal volume similar to that of healthy subjects. In healthy subjects, the proximal gastric volume rapidly returned to baseline level after nutrient infusion (median 18 min). In contrast, the recovery of volume to baseline was delayed in critically ill patients (median 106 min). In 6 patients, the volume had not returned to baseline level 2 hours after nutrient infusion. In patients, fundic volume waves were less frequent (P < 0.05) and had lower amplitude (P < 0.001), compared to healthy subjects.
Conclusion: In critical illness, proximal gastric motor responses to small intestinal nutrient stimulation are abnormal.
Figures


References
-
- De Beaux M, Fraser R, Finnis M, De Keulenaer B, Liberalli D, Satanek M. Enteral nutrition in the critically ill: a prospective survey in an Australian intensive care unit. Anaesth Intensive Care. 2001;29:619–622. - PubMed
-
- Dive A, Moulart M, Jonard P, Jamart J, Mahieu P. Gastroduodenal motility in mechanically ventilated critically ill patients: a manometric study. Crit Care Med. 1994;22:441–447. - PubMed
-
- Dempsey DT, Mullen JL, Buzby GP. The link between nutritional status and clinical outcome: can nutritional intervention modify it. Am J Clin Nutr. 1988;47:352–356. - PubMed
-
- Ricci DA, McCallum RW. Diagnosis and treatment of delayed gastric emptying. Adv Intern Med. 1988;33:357–384. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

