Cytokine, sickness behavior, and depression
- PMID: 16877117
- PMCID: PMC2909644
- DOI: 10.1016/j.ncl.2006.03.003
Cytokine, sickness behavior, and depression
Abstract
Sufficient evidence is now available to accept the concept that the brain recognizes cytokines as molecular signals of sickness. Clarifying the way the brain processes information generated by the innate immune system is accompanied by a progressive elucidation of the cellular and molecular components of the intricate system that mediates cytokine-induced sickness behavior. We are still far, however, from understanding the whole. Among the hundreds of genes that proinflammatory cytokines can induce in their cellular targets, only a handful has been examined functionally. In addition, a dynamic view of the cellular interactions that occur at the brain sites of cytokine production and action is missing, together with a clarification of the mechanisms that favor the transition toward pathology.
Figures


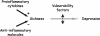

Republished in
-
Cytokine, sickness behavior, and depression.Immunol Allergy Clin North Am. 2009 May;29(2):247-64. doi: 10.1016/j.iac.2009.02.002. Immunol Allergy Clin North Am. 2009. PMID: 19389580 Free PMC article.
Similar articles
-
Cytokine-induced sickness behavior: where do we stand?Brain Behav Immun. 2001 Mar;15(1):7-24. doi: 10.1006/brbi.2000.0613. Brain Behav Immun. 2001. PMID: 11259077 Review.
-
Unkind cytokines: current evidence for the potential role of cytokines in immune-mediated depression.Int Rev Psychiatry. 2005 Dec;17(6):477-83. doi: 10.1080/02646830500381757. Int Rev Psychiatry. 2005. PMID: 16401546 Review.
-
Immune-to-Brain Communication Pathways in Inflammation-Associated Sickness and Depression.Curr Top Behav Neurosci. 2017;31:73-94. doi: 10.1007/7854_2016_37. Curr Top Behav Neurosci. 2017. PMID: 27677781 Review.
-
Age and neuroinflammation: a lifetime of psychoneuroimmune consequences.Neurol Clin. 2006 Aug;24(3):521-38. doi: 10.1016/j.ncl.2006.03.010. Neurol Clin. 2006. PMID: 16877122 Review.
-
Psychoneuroimmunology and the cytokine action in the CNS: implications for psychiatric disorders.Prog Neuropsychopharmacol Biol Psychiatry. 1998 Jan;22(1):1-33. doi: 10.1016/s0278-5846(97)00179-6. Prog Neuropsychopharmacol Biol Psychiatry. 1998. PMID: 9533165 Review.
Cited by
-
'Chronomics' in ICU: circadian aspects of immune response and therapeutic perspectives in the critically ill.Intensive Care Med Exp. 2014 Dec;2(1):18. doi: 10.1186/2197-425X-2-18. Epub 2014 May 14. Intensive Care Med Exp. 2014. PMID: 26266918 Free PMC article.
-
C-Reactive Protein as a Biomarker for Major Depressive Disorder?Int J Mol Sci. 2022 Jan 30;23(3):1616. doi: 10.3390/ijms23031616. Int J Mol Sci. 2022. PMID: 35163538 Free PMC article. Review.
-
Inflammatory markers as predictors of depression and anxiety in adolescents: Statistical model building with component-wise gradient boosting.J Affect Disord. 2018 Jul;234:276-281. doi: 10.1016/j.jad.2018.03.006. Epub 2018 Mar 12. J Affect Disord. 2018. PMID: 29554616 Free PMC article.
-
Peripheral injection of SB203580 inhibits the inflammatory-dependent synthesis of proinflammatory cytokines in the hypothalamus.Biomed Res Int. 2014;2014:475152. doi: 10.1155/2014/475152. Epub 2014 Jun 4. Biomed Res Int. 2014. PMID: 24995301 Free PMC article.
-
Immune Homeostasis: A Novel Example of Teamwork.Methods Mol Biol. 2024;2782:1-24. doi: 10.1007/978-1-0716-3754-8_1. Methods Mol Biol. 2024. PMID: 38622389
References
-
- Dantzer R. Cytokine-induced sickness behavior: where do we stand? Brain Behav Immun. 2001;15:7–24. - PubMed
-
- Konsman JP, Parnet P, Dantzer R. Cytokine-induced sickness behaviour: mechanisms and implications. Trends Neurosci. 2002;25:154–9. - PubMed
-
- Barton GM, Medzhitov R. Toll-like receptor signaling pathways. Science. 2003;300:1524–5. - PubMed
-
- Romanovsky A, Almeida MC, Aronoff DM, et al. Fever and hypothermia in systemic inflammation: recent discoveries and revisions. Front Biosci. 2005;10:2193–216. - PubMed
-
- Berkenbosch F, van Oers J, del Rey A, et al. Corticotropin-releasing factor-producing neurons in the rat activated by interleukin-1. Science. 1987;238:524–6. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

