Persistent depression affects adherence to secondary prevention behaviors after acute coronary syndromes
- PMID: 16899061
- PMCID: PMC1831650
- DOI: 10.1111/j.1525-1497.2006.00586.x
Persistent depression affects adherence to secondary prevention behaviors after acute coronary syndromes
Abstract
Background: The persistence of depressive symptoms after hospitalization is a strong risk factor for mortality after acute coronary syndromes (ACS). Poor adherence to secondary prevention behaviors may be a mediator of the relationship between depression and increased mortality.
Objective: To determine whether rates of adherence to risk reducing behaviors were affected by depressive status during hospitalization and 3 months later.
Design: Prospective observational cohort study.
Setting: Three university hospitals.
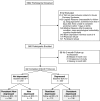
Participants: Five hundred and sixty patients were enrolled within 7 days after ACS. Of these, 492 (88%) patients completed 3-month follow-up.
Measurements: We used the Beck Depression Inventory (BDI) to assess depressive symptoms in the hospital and 3 months after discharge. We assessed adherence to 5 risk-reducing behaviors by patient self-report at 3 months. We used chi2 analysis to compare differences in adherence among 3 groups: persistently nondepressed (BDI < 10 at hospitalization and 3 months); remittent depressed (BDI > or = 10 at hospitalization; < 10 at 3 months); and persistently depressed patients (BDI > or = 10 at hospitalization and 3 months).
Results: Compared with persistently nondepressed, persistently depressed patients reported lower rates of adherence to quitting smoking (adjusted odds ratio [OR] 0.23, 95% confidence interval [95% CI] 0.05 to 0.97), taking medications (adjusted OR 0.50, 95% CI 0.27 to 0.95), exercising (adjusted OR 0.57, 95% CI 0.34 to 0.95), and attending cardiac rehabilitation (adjusted OR 0.5, 95% CI 0.27 to 0.91). There were no significant differences between remittent depressed and persistently nondepressed patients.
Conclusions: Persistently depressed patients were less likely to adhere to behaviors that reduce the risk of recurrent ACS. Differences in adherence to these behaviors may explain in part why depression predicts mortality after ACS.
Figures
References
-
- Lane D, Carroll D, Ring C, Beevers DG, Lip GY. The prevalence and persistence of depression and anxiety following myocardial infarction. Br J Health Psychol. 2002;7:11–21. - PubMed
-
- Lesperance F, Frasure-Smith N, Juneau M, Theroux P. Depression and 1-year prognosis in unstable angina. Arch Intern Med. 2000;160:1354–60. - PubMed
-
- Barefoot JC, Schroll M. Symptoms of depression, acute myocardial infarction, and total mortality in a community sample. Circulation. 1996;93:1976–80. - PubMed
-
- Frasure-Smith N, Lesperance F, Talajic M. Depression and 18-month prognosis after myocardial infarction. Circulation. 1995;91:999–1005. - PubMed
-
- Bush DE, Ziegelstein RC, Tayback M, et al. Even minimal symptoms of depression increase mortality risk after acute myocardial infarction. Am J Cardiol. 2001;88:337–41. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources