Pseudoachalasia in a patient after truncal vagotomy surgery successfully treated by subsequent pneumatic dilations
- PMID: 16937515
- PMCID: PMC4087422
- DOI: 10.3748/wjg.v12.i31.5087
Pseudoachalasia in a patient after truncal vagotomy surgery successfully treated by subsequent pneumatic dilations
Abstract
Pseudoachalasia is a difficult condition for the clinician to differentiate from idiopathic achalasia even by manometry, radiological studies or endoscopy. Its etiology is usually associated with tumors. In most cases, the diagnosis is made after surgical explorations. The proposed pathogenesis of the disease is considered as mechanical obstruction of the distal esophagus or infiltration of the malignancy that affects the inhibitory neurons of the meyenteric plexus in the majority of cases. Surgery has been reported as a cause of pseudoachalasia. We report a 70-year-old man who suffered from deglutination disorder caused by pseudo-achalasia after truncal vagotomy. The patient was symptom-free after a nine-year follow-up and complete recovery of esophageal motility status from pseudoachalasia after pneumatic dilations. We also reviewed the literature of pseudoachalasia.
Figures
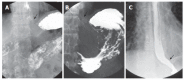
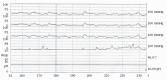
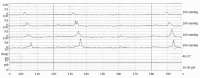
References
-
- Gockel I, Eckardt VF, Schmitt T, Junginger T. Pseudoachalasia: a case series and analysis of the literature. Scand J Gastroenterol. 2005;40:378–385. - PubMed
-
- Champion JK, Delise N, Hunt T. Myenteric plexus in spastic motility disorders. J Gastrointest Surg. 2001;5:514–516. - PubMed
-
- Park W, Vaezi MF. Etiology and pathogenesis of achalasia: the current understanding. Am J Gastroenterol. 2005;100:1404–1414. - PubMed
-
- Paterson WG. Etiology and pathogenesis of achalasia. Gastrointest Endosc Clin N Am. 2001;11:249–266, vi. - PubMed
-
- Hashemi N, Banwait KS, DiMarino AJ, Cohen S. Manometric evaluation of achalasia in the elderly. Aliment Pharmacol Ther. 2005;21:431–434. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

