Comparison of effects in randomized controlled trials with observational studies in digestive surgery
- PMID: 17060757
- PMCID: PMC1856609
- DOI: 10.1097/01.sla.0000225356.04304.bc
Comparison of effects in randomized controlled trials with observational studies in digestive surgery
Abstract
Objectives: To compare the results of randomized controlled trials versus observational studies in meta-analyses of digestive surgical topics.
Summary background data: While randomized controlled trials have been recognized as providing the highest standard of evidence, claims have been made that observational studies may overestimate treatment benefits. This debate has recently been renewed, particularly with regard to pharmacotherapies.
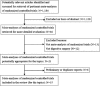
Methods: The PubMed (1966 to April 2004), EMBASE (1986 to April 2004) and Cochrane databases (Issue 2, 2004) were searched to identify meta-analyses of randomized controlled trials in digestive surgery. Fifty-two outcomes of 18 topics were identified from 276 original articles (96 randomized trials, 180 observational studies) and included in meta-analyses. All available binary data and study characteristics were extracted and combined separately for randomized and observational studies. In each selected digestive surgical topic, summary odds ratios or relative risks from randomized controlled trials were compared with observational studies using an equivalent calculation method.
Results: Significant between-study heterogeneity was seen more often among observational studies (5 of 12 topics) than among randomized trials (1 of 9 topics). In 4 of the 16 primary outcomes compared (10 of 52 total outcomes), summary estimates of treatment effects showed significant discrepancies between the two designs.
Conclusions: One fourth of observational studies gave different results than randomized trials, and between-study heterogeneity was more common in observational studies in the field of digestive surgery.
Figures


Comment in
-
Randomized, controlled trials: is there a role for them in surgery?Ann Surg. 2006 Nov;244(5):684-5. doi: 10.1097/01.sla.0000243593.93571.98. Ann Surg. 2006. PMID: 17060759 Free PMC article. No abstract available.
References
-
- Preventive Services Task Force. Guide to Clinical Preventive Services: Report of the U.S. Preventive Services Task Force, 2nd ed. Baltimore: Williams & Wilkins, 1996.
-
- Chalmers TC, Matta RJ, Smith H Jr, et al. Evidence favoring the use of anticoagulants in the hospital phase of acute myocardial infarction. N Engl J Med. 1977;297:1091–1096. - PubMed
-
- Sacks HS, Chalmers TC, Smith H Jr. Randomized versus historical controls for clinical trials. Am J Med. 1982;72:233–240. - PubMed
-
- Colditz GA, Miller JN, Mosteller F. How study design affects outcomes in comparisons of therapy. I. Med Stat Med. 1989;8:441–454. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

