Hyperoxia causes angiopoietin 2-mediated acute lung injury and necrotic cell death
- PMID: 17086189
- PMCID: PMC2768268
- DOI: 10.1038/nm1494
Hyperoxia causes angiopoietin 2-mediated acute lung injury and necrotic cell death
Abstract
The angiogenic growth factor angiopoietin 2 (Ang2) destabilizes blood vessels, enhances vascular leak and induces vascular regression and endothelial cell apoptosis. We considered that Ang2 might be important in hyperoxic acute lung injury (ALI). Here we have characterized the responses in lungs induced by hyperoxia in wild-type and Ang2-/- mice or those given either recombinant Ang2 or short interfering RNA (siRNA) targeted to Ang2. During hyperoxia Ang2 expression is induced in lung epithelial cells, while hyperoxia-induced oxidant injury, cell death, inflammation, permeability alterations and mortality are ameliorated in Ang2-/- and siRNA-treated mice. Hyperoxia induces and activates the extrinsic and mitochondrial cell death pathways and activates initiator and effector caspases through Ang2-dependent pathways in vivo. Ang2 increases inflammation and cell death during hyperoxia in vivo and stimulates epithelial necrosis in hyperoxia in vitro. Ang2 in plasma and alveolar edema fluid is increased in adults with ALI and pulmonary edema. Tracheal Ang2 is also increased in neonates that develop bronchopulmonary dysplasia. Ang2 is thus a mediator of epithelial necrosis with an important role in hyperoxic ALI and pulmonary edema.
Figures





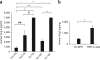
References
-
- Barazzone C, Horowitz S, Donati YR, Rodriguez I, Piguet PF. Oxygen toxicity in mouse lung: pathways to cell death. Am. J. Respir. Cell Mol. Biol. 1998;19:573–581. - PubMed
-
- Barazzone C, White CW. Mechanisms of cell injury and death in hyperoxia: role of cytokines and Bcl-2 family proteins. Am. J. Respir. Cell Mol. Biol. 2000;22:517–519. - PubMed
-
- Crapo JD. Morphologic changes in pulmonary oxygen toxicity. Annu. Rev. Physiol. 1986;48:721–731. - PubMed
-
- O'Reilly MA, et al. Bcl-2 family gene expression during severe hyperoxia induced lung injury. Lab. Invest. 2000;80:1845–1854. - PubMed
-
- Ward NS, et al. Interleukin-6-induced protection in hyperoxic acute lung injury. Am. J. Respir. Cell Mol. Biol. 2000;22:535–542. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

