Oxygen uptake-to-delivery relationship: a way to assess adequate flow
- PMID: 17164016
- PMCID: PMC3226126
- DOI: 10.1186/cc4831
Oxygen uptake-to-delivery relationship: a way to assess adequate flow
Abstract
Invasive and noninvasive monitoring facilitates clinical evaluation when resuscitating patients with complex haemodynamic disorders. If the macrocirculation is to be stable, then it must adapt to blood flow or blood flow must be optimized. The objective of flow monitoring is to assist with matching observed oxygen consumption (VO2) to pathophysiological needs. If an adequate balance cannot be maintained then dysoxia occurs. In this review we propose a simple schema for global reasoning; we discuss the limitations of VO2 and arterial oxygen delivery (DaO2) assessment; and we address concerns about increasing DaO2 to supranormal values or targeting pre-established levels of DaO2, cardiac output, or mixed venous oxygen saturation. All of these haemodynamic variables are interrelated and limited by physiological and/or pathological processes. A unique global challenge, and one that is of great prognostic interest, is to achieve rapid matching between observed and needed VO2--no more and no less. However, measuring or calculating these two variables at the bedside remains difficult. In practice, we propose a distinction between three situations. Clinical and blood lactate clearance improvements can limit investigations in simple cases. Intermediate cases may be managed by continuous monitoring of VO2-related variables such as DaO2, cardiac output, or mixed venous oxygen saturation. In more complex cases, three methods can help to estimate the needed VO2 level: comparison with expected values from past physiological studies; analysis of the relationship between VO2 and oxygen delivery; and use of computer software to integrate the preceding two methods.
Figures

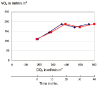

References
-
- Russell JA, Phang PT. The oxygen delivery/consumption controversy. Approaches to management of the critically ill. Am J Respir Crit Care Med. 1994;149:533–537. - PubMed
-
- Granton JT, Walley KR, Phang PT, Russell JA, Lichtenstein S. Assessment of three methods to reduce the influence of mathematical coupling on oxygen consumption and delivery relationships. Chest. 1998;113:1347–1355. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

