Meta-analysis of short-term outcomes after laparoscopy-assisted distal gastrectomy
- PMID: 17171799
- PMCID: PMC4088052
- DOI: 10.3748/wjg.v12.i47.7676
Meta-analysis of short-term outcomes after laparoscopy-assisted distal gastrectomy
Abstract
Aim: To elucidate the current status of laparoscopy-assisted distal gastrectomy (LADG) with regard to its short-term outcomes by comparing it with conventional open distal gastrectomy (CODG).
Methods: Original articles published from January 1991 to August 2006 were searched in the MEDLINE, EMBASE, and Cochrane Controlled Trials Register. Clinical appraisal and data extraction were conducted independently by 2 reviewers. A meta-analysis was performed using a random effects model.
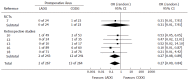
Results: Outcomes of 1611 procedures from 4 randomized controlled trials and 12 retrospective studies were analyzed. Compared to CODG, LADG was a longer procedure (weighted mean difference [WMD] 54.3; 95% confidence interval [CI] 38.8 to 69.8; P < 0.001), but was associated with a lower associated morbidity (odds ratio [OR] 0.54; 95% CI 0.37 to 0.77; P < 0.001); this was most significant for postoperative ileus (OR 0.27; 95% CI 0.09 to 0.84; P = 0.02). There was no significant difference between the two groups in anastomotic, pulmonary, and wound complications and mortality. Duration from surgery to first passage of flatus was faster (WMD -0.68; 95% CI -0.85 to -0.50; P < 0.001) and the frequency of additional analgesic requirement (WMD -1.36; 95% CI -2.44 to -0.28; P = 0.01), and duration of hospital stay (WMD -5.51; 95% CI -7.61 to -3.42; P < 0.001) were significantly lower after LADG. However, a significantly higher number of lymph nodes were dissected by CODG (WMD -4.35; 95% CI -5.73 to -2.98; P < 0.001).
Conclusion: LADG for early gastric cancer is associated with a lower morbidity, less pain, faster bowel function recovery, and shorter hospital stay.
Figures



References
-
- Reza MM, Blasco JA, Andradas E, Cantero R, Mayol J. Systematic review of laparoscopic versus open surgery for colorectal cancer. Br J Surg. 2006;93:921–928. - PubMed
-
- Chung RS, Rowland DY, Li P, Diaz J. A meta-analysis of randomized controlled trials of laparoscopic versus conventional appendectomy. Am J Surg. 1999;177:250–256. - PubMed
-
- Glavic Z, Begic L, Simlesa D, Rukavina A. Treatment of acute cholecystitis. A comparison of open vs laparoscopic cholecystectomy. Surg Endosc. 2001;15:398–401. - PubMed
-
- Kitano S, Iso Y, Moriyama M, Sugimachi K. Laparoscopy-assisted Billroth I gastrectomy. Surg Laparosc Endosc. 1994;4:146–148. - PubMed
-
- Goh PM, Alponat A, Mak K, Kum CK. Early international results of laparoscopic gastrectomies. Surg Endosc. 1997;11:650–652. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

