Extent and distribution of white matter hyperintensities in normal aging, MCI, and AD
- PMID: 17190943
- PMCID: PMC3776588
- DOI: 10.1212/01.wnl.0000249119.95747.1f
Extent and distribution of white matter hyperintensities in normal aging, MCI, and AD
Abstract
Objective: To analyze the extent and spatial distribution of white matter hyperintensities (WMH) in brain regions from cognitively normal older individuals (CN) and patients with mild cognitive impairment (MCI) and Alzheimer disease (AD).
Methods: We studied 26 mild AD, 28 MCI, and 33 CN. MRI analysis included quantification of WMH volume, nonlinear mapping onto a common anatomic image, and spatial localization of each WMH voxel to create an anatomically precise frequency distribution map. Areas of greatest frequency of WMH from the WMH composite map were used to identify 10 anatomic regions involving periventricular areas and the corpus callosum (CC) for group comparisons.
Results: Total WMH volumes were associated with age, extent of concurrent vascular risk factors, and diagnosis. After correcting for age, total WMH volumes remained significantly associated with diagnosis and extent of vascular risk. Regional WMH analyses revealed significant differences in WMH across regions that also differed significantly according to diagnosis. In post-hoc analyses, significant differences were seen between CN and AD in posterior periventricular regions and the splenium of the CC. MCI subjects had intermediate values at all regions. Repeated measures analysis including vascular risk factors in the model found a significant relationship between periventricular WMH and vascular risk that differed by region, but regional differences according to diagnosis remained significant and there was no interaction between diagnosis and vascular risk.
Conclusions: Differences in white matter hyperintensities (WMH) associated with increasing cognitive impairment appear related to both extent and spatial location. Multiple regression analysis of regional WMH, vascular risk factors, and diagnosis suggest that these spatial differences may result from the additive effects of vascular and degenerative injury. Posterior periventricular and corpus callosum extension of WMH associated with mild cognitive impairment and Alzheimer disease indicate involvement of strategic white matter bundles that may contribute to the cognitive deficits seen with these syndromes.
Conflict of interest statement
Disclosure: The authors report no conflicts of interest.
Figures



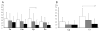


Similar articles
-
Regional white matter hyperintensities in normal aging, single domain amnestic mild cognitive impairment, and mild Alzheimer's disease.J Clin Neurosci. 2011 Aug;18(8):1101-6. doi: 10.1016/j.jocn.2011.01.008. Epub 2011 Jul 2. J Clin Neurosci. 2011. PMID: 21723730
-
Regional pattern of white matter microstructural changes in normal aging, MCI, and AD.Neurology. 2009 Nov 24;73(21):1722-8. doi: 10.1212/WNL.0b013e3181c33afb. Epub 2009 Oct 21. Neurology. 2009. PMID: 19846830 Free PMC article.
-
Vascular and degenerative processes differentially affect regional interhemispheric connections in normal aging, mild cognitive impairment, and Alzheimer disease.Stroke. 2010 Aug;41(8):1791-7. doi: 10.1161/STROKEAHA.110.582163. Epub 2010 Jul 1. Stroke. 2010. PMID: 20595668 Free PMC article.
-
White matter hyperintensities and neuropsychological outcome following carbon monoxide poisoning.Neurology. 2002 May 28;58(10):1525-32. doi: 10.1212/wnl.58.10.1525. Neurology. 2002. PMID: 12034791 Review.
-
White Matter Hyperintensities and Cognition in Mild Cognitive Impairment and Alzheimer's Disease: A Domain-Specific Meta-Analysis.J Alzheimers Dis. 2018;63(2):515-527. doi: 10.3233/JAD-170573. J Alzheimers Dis. 2018. PMID: 29630548 Review.
Cited by
-
Tractography at 3T MRI of Corpus Callosum Tracts Crossing White Matter Hyperintensities.AJNR Am J Neuroradiol. 2016 Sep;37(9):1617-22. doi: 10.3174/ajnr.A4788. Epub 2016 Apr 28. AJNR Am J Neuroradiol. 2016. PMID: 27127001 Free PMC article.
-
In vivo microstructural heterogeneity of white matter and cognitive correlates in aging using tissue compositional analysis of diffusion magnetic resonance imaging.Hum Brain Mapp. 2024 Mar;45(4):e26618. doi: 10.1002/hbm.26618. Hum Brain Mapp. 2024. PMID: 38414286 Free PMC article.
-
Coevolution of white matter hyperintensities and cognition in the elderly.Neurology. 2012 Jul 31;79(5):442-8. doi: 10.1212/WNL.0b013e3182617136. Epub 2012 Jul 18. Neurology. 2012. PMID: 22815562 Free PMC article.
-
White matter hyperintensities in diverse populations: A systematic review of literature in the United States.Cereb Circ Cogn Behav. 2024 Jan 14;6:100204. doi: 10.1016/j.cccb.2024.100204. eCollection 2024. Cereb Circ Cogn Behav. 2024. PMID: 38298455 Free PMC article. Review.
-
Regional White Matter Hyperintensities and Alzheimer's Disease Biomarkers Among Older Adults with Normal Cognition and Mild Cognitive Impairment.J Alzheimers Dis. 2023;92(1):323-339. doi: 10.3233/JAD-220846. J Alzheimers Dis. 2023. PMID: 36744337 Free PMC article.
References
-
- Chirtiansen P, Larsson HB, Thomsen C, et al. Age dependent white matter lesions and brain volume changes in healthy volunteers. Acta Radiol. 1994;35:117–122. - PubMed
-
- DeCarli C, Massaro J, Harvey D, et al. Measures of brain morphology and infarction in the Framingham Heart Study: establishing what is normal. Neurobiol Aging. 2005;26:491–510. - PubMed
-
- Bretler MMV, van Swieten JC, Bots ML, et al. Cerebral white matter lesions, vascular risk factors, and cognitive function in a population-based study: the Rotterdam Study. Neurology. 1994;44:1246–1252. - PubMed
-
- Jeerakathil T, Wolf PA, Beiser A, et al. Stroke risk profile predicts white matter hyperintensity volume: the Framingham Study. Stroke. 2004;35:1857–1861. - PubMed
-
- DeCarli C, Miller BL, Swan GE, et al. Cerebrovascular and brain morphologic correlates of mild cognitive impairment in the National Heart, Lung, and Blood Institute Twin Study. Arch Neurol. 2001;58:643–647. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
