Quality of life and salivary output in patients with head-and-neck cancer five years after radiotherapy
- PMID: 17207274
- PMCID: PMC1779273
- DOI: 10.1186/1748-717X-2-3
Quality of life and salivary output in patients with head-and-neck cancer five years after radiotherapy
Abstract
Background: To describe long-term changes in time of quality of life (QOL) and the relation with parotid salivary output in patients with head-and-neck cancer treated with radiotherapy.
Methods: Forty-four patients completed the EORTC-QLQ-C30(+3) and the EORTC-QLQ-H&N35 questionnaires before treatment, 6 weeks, 6 months, 12 months, and at least 3.5 years after treatment. At the same time points, stimulated bilateral parotid flow rates were measured.
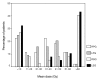
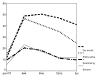
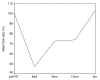
Results: There was a deterioration of most QOL items after radiotherapy compared with baseline, with gradual improvement during 5 years follow-up. The specific xerostomia-related items showed improvement in time, but did not return to baseline. Global QOL did not alter significantly in time, although 41% of patients complained of moderate or severe xerostomia at 5 years follow-up. Five years after radiotherapy the mean cumulated parotid flow ratio returned to baseline but 20% of patients had a flow ratio <25%. The change in time of xerostomia was significantly related with the change in flow ratio (p = 0.01).
Conclusion: Most of the xerostomia-related QOL scores improved in time after radiotherapy without altering the global QOL, which remained high. The recovery of the dry mouth feeling was significantly correlated with the recovery in parotid flow ratio.
Figures

Similar articles
-
Preservation of oral health-related quality of life and salivary flow rates after inverse-planned intensity- modulated radiotherapy (IMRT) for head-and-neck cancer.Int J Radiat Oncol Biol Phys. 2004 Mar 1;58(3):663-73. doi: 10.1016/S0360-3016(03)01571-2. Int J Radiat Oncol Biol Phys. 2004. PMID: 14967418 Clinical Trial.
-
Does radiation dose to the salivary glands and oral cavity predict patient-rated xerostomia and sticky saliva in head and neck cancer patients treated with curative radiotherapy?Radiother Oncol. 2005 Nov;77(2):164-71. doi: 10.1016/j.radonc.2005.10.002. Epub 2005 Oct 26. Radiother Oncol. 2005. PMID: 16256229
-
Xerostomia and quality of life after intensity-modulated radiotherapy vs. conventional radiotherapy for early-stage nasopharyngeal carcinoma: initial report on a randomized controlled clinical trial.Int J Radiat Oncol Biol Phys. 2006 Nov 15;66(4):981-91. doi: 10.1016/j.ijrobp.2006.06.013. Int J Radiat Oncol Biol Phys. 2006. PMID: 17145528 Clinical Trial.
-
Radiation-induced xerostomia in patients with head and neck cancer: pathogenesis, impact on quality of life, and management.Head Neck. 2004 Sep;26(9):796-807. doi: 10.1002/hed.20045. Head Neck. 2004. PMID: 15350026 Review.
-
Outcomes of xerostomia-related quality of life for nasopharyngeal carcinoma treated by IMRT: based on the EORTC QLQ-C30 and H&N35 questionnaires.Expert Rev Anticancer Ther. 2015 Jan;15(1):109-19. doi: 10.1586/14737140.2015.961427. Epub 2014 Sep 18. Expert Rev Anticancer Ther. 2015. PMID: 25231774 Review.
Cited by
-
Radiotherapy dose-volume effects on salivary gland function.Int J Radiat Oncol Biol Phys. 2010 Mar 1;76(3 Suppl):S58-63. doi: 10.1016/j.ijrobp.2009.06.090. Int J Radiat Oncol Biol Phys. 2010. PMID: 20171519 Free PMC article. Review.
-
Mathematical evaluation of post-radiotherapy salivary gland function using salivary gland scintigraphy.Br J Radiol. 2022 Feb 1;95(1130):20210718. doi: 10.1259/bjr.20210718. Epub 2021 Dec 20. Br J Radiol. 2022. PMID: 34928174 Free PMC article.
-
A Prospective Cohort Study Analyzing Radiation-Induced Xerostomia and Quality of Life of Head and Neck Cancer Patients Treated With Intensity-Modulated Radiotherapy and 3D Conformal Radiotherapy Techniques at a Tertiary Cancer Center in Eastern India.Cureus. 2023 Mar 20;15(3):e36442. doi: 10.7759/cureus.36442. eCollection 2023 Mar. Cureus. 2023. PMID: 37090370 Free PMC article.
-
Translation and Validation of University of Washington Quality of Life Questionnaire in Malayalam, an Indian Language.J Maxillofac Oral Surg. 2024 Dec;23(6):1594-1600. doi: 10.1007/s12663-021-01573-6. Epub 2021 Apr 19. J Maxillofac Oral Surg. 2024. PMID: 39618435
-
Toxicity and biodistribution of the serotype 2 recombinant adeno-associated viral vector, encoding Aquaporin-1, after retroductal delivery to a single mouse parotid gland.PLoS One. 2014 Mar 25;9(3):e92832. doi: 10.1371/journal.pone.0092832. eCollection 2014. PLoS One. 2014. PMID: 24667436 Free PMC article.
References
-
- Valdez IH. Radiation-induced salivary dysfunction: clinical course and significance. Spec Care Dentist. 1991;11:252–255. - PubMed
-
- Bjordal K, Kaasa S, Mastekaasa A. Quality of life in patients treated for head and neck cancer: a follow-up study 7 to 11 years after radiotherapy. Int J Radiat Oncol Biol Phys. 1994;28:847–856. - PubMed
-
- Jensen AB, Hansen O, Jorgensen K, Bastholt L. Influence of late side-effects upon daily life after radiotherapy for laryngeal and pharyngeal cancer. Acta Oncol. 1994;33:487–491. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

