Cortical abnormalities in epilepsy revealed by local EEG synchrony
- PMID: 17224281
- PMCID: PMC1994936
- DOI: 10.1016/j.neuroimage.2006.11.009
Cortical abnormalities in epilepsy revealed by local EEG synchrony
Abstract
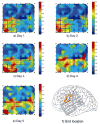
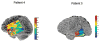
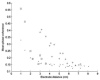
Abnormally strong functional linkage between cortical areas has been postulated to play a role in the pathogenesis of partial epilepsy. We explore the possibility that such linkages may be manifest in the interictal EEG apart from epileptiform disturbances or visually evident focal abnormalities. We analyzed samples of interictal intracranial EEG (ICEEG) recorded from subdural grids in nine patients with medically intractable partial epilepsy, measuring interelectrode synchrony using the mean phase coherence algorithm. This analysis revealed areas of elevated local synchrony, or "hypersynchrony" which had persistent spatiotemporal characteristics that were unique to each patient. Measuring local synchrony in a subdural grid results in a map of the cortical surface that provides information not visually apparent on either EEG or structural imaging. We explore the relationship of hypersynchronous areas to the clinical evidence of seizure localization in each case, and speculate that local hypersynchrony may be a marker of epileptogenic cortex, and may prove to be a valuable aid to clinical ICEEG interpretation.
Figures


Similar articles
-
Results of surgery in patients with refractory extratemporal epilepsy with normal or nonlocalizing magnetic resonance findings investigated with subdural grids.Epilepsia. 2001 Jul;42(7):889-94. doi: 10.1046/j.1528-1157.2001.00201.x. Epilepsia. 2001. PMID: 11488889
-
Subdural electrode analysis in focal cortical dysplasia: predictors of surgical outcome.Neurology. 2007 Aug 14;69(7):660-7. doi: 10.1212/01.wnl.0000267427.91987.21. Neurology. 2007. PMID: 17698787
-
The impact of cerebral source area and synchrony on recording scalp electroencephalography ictal patterns.Epilepsia. 2007 Nov;48(11):2167-76. doi: 10.1111/j.1528-1167.2007.01224.x. Epub 2007 Jul 28. Epilepsia. 2007. PMID: 17662060
-
Use of magnetoencephalography in the presurgical evaluation of epilepsy patients.Clin Neurophysiol. 2007 Jul;118(7):1438-48. doi: 10.1016/j.clinph.2007.03.002. Epub 2007 Apr 23. Clin Neurophysiol. 2007. PMID: 17452007 Review.
-
Cortical substrates of scalp EEG epileptiform discharges.J Clin Neurophysiol. 2007 Apr;24(2):96-100. doi: 10.1097/WNP.0b013e31803ecdaf. J Clin Neurophysiol. 2007. PMID: 17414965 Review.
Cited by
-
Recording and analysis techniques for high-frequency oscillations.Prog Neurobiol. 2012 Sep;98(3):265-78. doi: 10.1016/j.pneurobio.2012.02.006. Epub 2012 Mar 7. Prog Neurobiol. 2012. PMID: 22420981 Free PMC article. Review.
-
Understanding Language Reorganization With Neuroimaging: How Language Adapts to Different Focal Lesions and Insights Into Clinical Applications.Front Hum Neurosci. 2022 Feb 18;16:747215. doi: 10.3389/fnhum.2022.747215. eCollection 2022. Front Hum Neurosci. 2022. PMID: 35250510 Free PMC article. Review.
-
Disrupted functional brain connectivity in partial epilepsy: a resting-state fMRI study.PLoS One. 2011;7(1):e28196. doi: 10.1371/journal.pone.0028196. Epub 2012 Jan 5. PLoS One. 2011. PMID: 22242146 Free PMC article.
-
Toward new paradigms of seizure detection.Epilepsy Behav. 2013 Mar;26(3):247-52. doi: 10.1016/j.yebeh.2012.10.027. Epub 2012 Dec 12. Epilepsy Behav. 2013. PMID: 23246145 Free PMC article. Review.
-
Magnetoencephalographic signatures of insular epileptic spikes based on functional connectivity.Hum Brain Mapp. 2016 Sep;37(9):3250-61. doi: 10.1002/hbm.23238. Epub 2016 May 24. Hum Brain Mapp. 2016. PMID: 27220112 Free PMC article.
References
-
- Alarcon G, Binnie CD, et al. Power spectrum and intracranial EEG patterns at seizure onset in partial epilepsy. Electroencephalogr Clin Neurophysiol. 1995;94:326–337. - PubMed
-
- Allen PJ, Fish DR, et al. Very high-frequency rhythmic activity during SEEG suppression in frontal lobe epilepsy. Electroencephalography and Clinical Neurophysiology. 1992;82(2):155–59. - PubMed
-
- Blumenfeld H. Positive and negative network correlations in temporal lobe epilepsy - PubMed
-
- Bragin A, Wilson CL, et al. Chronic epileptogenesis requires development of a network of pathologically interconnected neuron clusters: a hypothesis. Epilepsia. 2000;41(Suppl 6):S144–52. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

