Treatment of malaria restricted to laboratory-confirmed cases: a prospective cohort study in Ugandan children
- PMID: 17239256
- PMCID: PMC1797179
- DOI: 10.1186/1475-2875-6-7
Treatment of malaria restricted to laboratory-confirmed cases: a prospective cohort study in Ugandan children
Abstract
Background: Presumptive treatment of malaria in febrile children is widely advocated in Africa. This may occur in the absence of diagnostic testing or even when diagnostic testing is performed but fails to detect malaria parasites. Such over-treatment of malaria has been tolerated in the era of inexpensive and safe monotherapy. However, with the introduction of new artemisinin-based combination therapy (ACT), presumptive treatment becomes economically and clinically less acceptable.
Methods: The risks and benefits of only treating children with microscopy confirmed malaria using a prospective cohort design were investigated. A representative sample of 601 children between one and 10 years of age were recruited from a census population in Kampala, Uganda and were followed for all of their health care needs in a study clinic. Standard microscopy was performed each time a child presented with a new episode of fever and antimalarial therapy given only if the blood smear was positive.
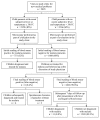
Results: Of 5,895 visits for new medical problems 40% were for febrile illnesses. Of the 2,359 episodes of new febrile illnesses, blood smears were initially reported as negative in 1,608 (68%) and no antimalarial therapy was given. Six of these initially negative smears were reported to be positive following quality control reading of all blood smears: four of these patients were subsequently diagnosed with uncomplicated malaria and two cleared their parasites without antimalarial treatment. Of the 1,602 new febrile illnesses in which the final blood smear reading was classified as negative, only 13 episodes (0.8%) were diagnosed with malaria in the subsequent 7 days. All 13 of these episodes of malaria were uncomplicated and were successfully treated.
Conclusion: In this urban setting, malaria was responsible for only 32% of febrile episodes. Withholding antimalarial therapy in febrile children with negative blood smears was safe and saved over 1,600 antimalarial treatments in 601 children over an 18-month period. In the era of expensive ACT, directing resources towards improving diagnostic and treatment practices may provide a cost-effective measure for promoting rational use of antimalarial therapy.
Figures
References
-
- WHO . WHO guidelines for treatment of malaria. Geneva: WHO; 2006. WHO/HTM/MAL/2006.1108.
-
- Agnamey P, Brasseur P, Cisse M, Gaye O, Dumoulin J, Rigal J, Taylor WR, Olliaro P. Economic evaluation of a policy change from single-agent treatment for suspected malaria to artesunate-amodiaquine for microscopically confirmed uncomplicated falciparum malaria in the Oussouye District of south-western Senegal. Trop Med Int Health. 2005;10:926–933. doi: 10.1111/j.1365-3156.2005.01482.x. - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

