Clinical experience with gene therapy for the treatment of prostate cancer
- PMID: 17387369
- PMCID: PMC1831538
Clinical experience with gene therapy for the treatment of prostate cancer
Abstract
Localized prostate cancer can be treated effectively with radical prostatectomy or radiation therapy. The treatment options for metastatic prostate cancer are limited to hormonal therapy; hormone-refractory cancer is treated with taxane-based chemotherapy, which provides only a modest survival benefit. New treatments are needed. The gene for the initiation of prostate cancer has not been identified; however, gene therapy can involve tumor injection of a gene to kill cells, systemic gene delivery to target and kill metastases, or local gene expression intended to generate a systemic response. This review will provide an overview of the various strategies of cancer gene therapy, focusing on those that have gone to clinical trial, detailing clinical experience in prostate cancer patients.
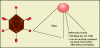
Figures



Similar articles
-
Management of localised prostate cancer: watchful waiting, surgery or radiation therapy, depending on the natural course, which is often relatively slow.Prescrire Int. 2012 Oct;21(131):242-8. Prescrire Int. 2012. PMID: 23185849 Review.
-
Overview of resistance to systemic therapy in patients with breast cancer.Adv Exp Med Biol. 2007;608:1-22. doi: 10.1007/978-0-387-74039-3_1. Adv Exp Med Biol. 2007. PMID: 17993229 Review.
-
Prostate specific antigen only progression of prostate cancer.J Urol. 2000 Jun;163(6):1632-42. J Urol. 2000. PMID: 10799151 Review.
-
Early versus late hormonal therapy: debating the issues.Urology. 2003 Feb;61(2 Suppl 1):8-13. doi: 10.1016/s0090-4295(02)02394-4. Urology. 2003. PMID: 12667882
-
The evolving role of systemic therapy in high risk prostate cancer: strategies for cure in the 21st century.Crit Rev Oncol Hematol. 2002 May;42(2):179-88. doi: 10.1016/s1040-8428(01)00187-1. Crit Rev Oncol Hematol. 2002. PMID: 12007976 Review.
Cited by
-
Functional characterization of the GDEP promoter and three enhancer elements in retinoblastoma and prostate cell lines.Med Oncol. 2008;25(1):40-9. doi: 10.1007/s12032-007-0038-4. Epub 2007 Jun 27. Med Oncol. 2008. PMID: 18188713
References
-
- Jemal A, Siegel R, Ward E, et al. Cancer Statistics, 2006. CA Cancer J Clin. 2006;56:106–130. - PubMed
-
- Petrylak DP, Tangen CM, Hussain MH, et al. Docetaxel and estramustine compared with mitoxantrone and prednisone for advanced refractory prostate cancer. N Engl J Med. 2004;351:1513–1520. - PubMed
-
- Tannock IF, de Wit R, Berry WR, et al. for the TAX 327 Investigators, authors. Docetaxel plus prednisone or mitoxantrone plus prednisone for advanced prostate cancer. N Engl J Med. 2004;351:1502–1512. - PubMed
-
- Office of Biotechnology Web site, authors. [November 2006]. Available at: http://www4.od.nih.gov/oba.
-
- Simons JW, Mikhak B, Chang JF, et al. Induction of immunity to prostate cancer antigens: results of a clinical trial of vaccination with irradiated autologous prostate tumor cells engineered to secrete granulocyte-macrophage colony-stimulating factor using ex vivo gene transfer. Cancer Res. 1999;59:5160–5168. - PubMed
LinkOut - more resources
Full Text Sources
