Are regional variations in end-of-life care intensity explained by patient preferences?: A Study of the US Medicare Population
- PMID: 17446824
- PMCID: PMC2147061
- DOI: 10.1097/01.mlr.0000255248.79308.41
Are regional variations in end-of-life care intensity explained by patient preferences?: A Study of the US Medicare Population
Abstract
Objective: We sought to test whether variations across regions in end-of-life (EOL) treatment intensity are associated with regional differences in patient preferences for EOL care.
Research design: Dual-language (English/Spanish) survey conducted March to October 2005, either by mail or computer-assisted telephone questionnaire, among a probability sample of 3480 Medicare part A and/or B eligible beneficiaries in the 20% denominator file, age 65 or older on July 1, 2003. Data collected included demographics, health status, and general preferences for medical care in the event the respondent had a serious illness and less than 1 year to live. EOL concerns and preferences were regressed on hospital referral region EOL spending, a validated measure of treatment intensity.
Results: A total of 2515 Medicare beneficiaries completed the survey (65% response rate). In analyses adjusted for age, sex, race/ethnicity, education, financial strain, and health status, there were no differences by spending in concern about getting too little treatment (39.6% in lowest spending quintile, Q1; 41.2% in highest, Q5; P value for trend, 0.637) or too much treatment (44.2% Q1, 45.1% Q5; P = 0.797) at the end of life, preference for spending their last days in a hospital (8.4% Q1, 8.5% Q5; P = 0.965), for potentially life-prolonging drugs that made them feel worse all the time (14.4% Q1, 16.5% Q5; P = 0.326), for palliative drugs, even if they might be life-shortening (77.7% Q1, 73.4% Q5; P = 0.138), for mechanical ventilation if it would extend their life by 1 month (21% Q1, 21.4% Q5; P = 0.870) or by 1 week (12.1% Q1, 11.7%; P = 0.875).
Conclusions: Medicare beneficiaries generally prefer treatment focused on palliation rather than life-extension. Differences in preferences are unlikely to explain regional variations in EOL spending.
Figures
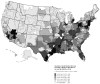
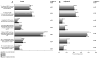
Comment in
-
Toward a better understanding of the role of geography in intensity of end-of-life care: must we first come to an understanding of end-of-life care?Med Care. 2007 May;45(5):374-6. doi: 10.1097/01.mlr.0000263474.23170.c2. Med Care. 2007. PMID: 17446822 No abstract available.
References
-
- Wennberg JE, Cooper M. The Dartmouth Atlas of Health Care. [Accessed January 2, 2007]. Available at: www.dartmouthatlas.org.
-
- Fisher ES, Wennberg DE, Stukel TA, et al. The implications of regional variations in Medicare spending. Part 1: the content, quality, and accessibility of care. Ann Intern Med. 2003;138:273–287. - PubMed
-
- Fisher ES, Wennberg DE, Stukel TA, et al. The implications of regional variations in Medicare spending. Part 2: health outcomes and satisfaction with care. Ann Intern Med. 2003;138:288–298. - PubMed
-
- Teno JM, Mor V, Ward N, et al. Bereaved family member perceptions of quality of end-of-life care in U.S. regions with high and low usage of intensive care unit care. J Am Geriatr Soc. 2005;53:1905–1911. - PubMed
-
- Welch WP, Miller ME, Welch HG, et al. Geographic variation in expenditures for physicians’ services in the United States [see comments] N Engl J Med. 1993;328:621–627. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

