An evaluation of prognostic factors and tumor staging of resected carcinoma of the esophagus
- PMID: 17457164
- PMCID: PMC1877056
- DOI: 10.1097/01.sla.0000251703.35919.02
An evaluation of prognostic factors and tumor staging of resected carcinoma of the esophagus
Abstract
Objective: To evaluate prognostic factors and tumor staging in patients after esophagectomy for cancer.
Summary background data: Several reports have questioned the appropriateness of the sixth edition of the International Union Against Cancer (UICC) TNM guidelines for staging esophageal cancer. Additional pathologic characteristics, besides the 3 basic facets of anatomic spread (tumor, node, metastases), might also have prognostic value.
Methods: All patients who underwent resection of the esophagus for carcinoma between January 1995 and March 2003 were extracted from a prospective database. Univariate and multivariate analysis was performed to identify prognostic factors for survival. The goodness of fit and accuracy of 3 staging models (UICC-TNM, Korst classification, Rice classification) predicting survival were assessed.
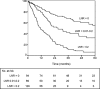
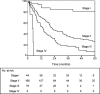
Results: A total of 292 patients (mean age, 63 years) underwent esophagectomy. The 5-year overall survival rate was 29% (median, 21 months). pT-, pN-, pm-stage, and radicality of the resection were independent prognostic factors. Subdivision of T1 tumors into mucosal and submucosal showed significant differences in 5-year survival between both groups: 90% versus 47%, respectively (P = 0.01). Subdivision of pN-stage into 3 groups based on the number of positive nodes (0, 1-2, and >3 nodes positive) or the lymph node ratio (0, 0.01-0.2, and >0.2) also refined staging (P = 0.001 and P < 0.001, respectively). The current subclassification of M1 (M1a and M1b) is not warranted (P = 0.41). The staging model of Rice was more accurate than the UICC-TNM classification in predicting survival.
Conclusion: This study supports the view that the current (6th edition) UICC-TNM staging model for esophageal cancer needs to be revised.
Figures





Similar articles
-
Improving the accuracy of TNM staging in esophageal cancer: a pathological review of resected specimens.Ann Surg Oncol. 2008 Dec;15(12):3447-58. doi: 10.1245/s10434-008-0155-0. Epub 2008 Oct 1. Ann Surg Oncol. 2008. PMID: 18830669
-
[Analysis of the survival in patients after surgical resection of thoracic esophageal cancer].Zhonghua Zhong Liu Za Zhi. 2009 Jul;31(7):541-5. Zhonghua Zhong Liu Za Zhi. 2009. PMID: 19950705 Chinese.
-
[Influence of number of removed lymph nodes on the TNM staging and survival in advanced esophageal carcinoma].Zhonghua Zhong Liu Za Zhi. 2007 Aug;29(8):604-8. Zhonghua Zhong Liu Za Zhi. 2007. PMID: 18210881 Chinese.
-
New TNM staging system for esophageal cancer: what chest radiologists need to know.Radiographics. 2014 Oct;34(6):1722-40. doi: 10.1148/rg.346130079. Radiographics. 2014. PMID: 25310426 Review.
-
Comparison of two major staging systems of esophageal cancer-toward more practical common scale for tumor staging.Ann Transl Med. 2018 Feb;6(4):76. doi: 10.21037/atm.2018.01.27. Ann Transl Med. 2018. PMID: 29666799 Free PMC article. Review.
Cited by
-
Prognostic analysis of esophageal cancer in elderly patients: metastatic lymph node ratio versus 2010 AJCC classification by lymph nodes.World J Surg Oncol. 2013 Jul 18;11:162. doi: 10.1186/1477-7819-11-162. World J Surg Oncol. 2013. PMID: 23866060 Free PMC article.
-
Preoperative platelet lymphocyte ratio (PLR) is superior to neutrophil lymphocyte ratio (NLR) as a predictive factor in patients with esophageal squamous cell carcinoma.World J Surg Oncol. 2014 Mar 19;12:58. doi: 10.1186/1477-7819-12-58. World J Surg Oncol. 2014. PMID: 24641770 Free PMC article.
-
Turning left or right? A comparative analysis in adenocarcinomas of the esophagogastric junction according to the seventh AJCC TNM classification for cancers of the esophagus and stomach: experience in a Chinese single institution.Int J Clin Exp Med. 2015 Jul 15;8(7):10668-77. eCollection 2015. Int J Clin Exp Med. 2015. PMID: 26379858 Free PMC article.
-
Lymphopenia predicts poor prognosis in patients with esophageal squamous cell carcinoma.Medicine (Baltimore). 2014 Dec;93(27):e257. doi: 10.1097/MD.0000000000000257. Medicine (Baltimore). 2014. PMID: 25501097 Free PMC article.
-
Extended lymphadenectomy in esophageal cancer is crucial.World J Surg. 2013 Aug;37(8):1751-6. doi: 10.1007/s00268-013-2068-8. World J Surg. 2013. PMID: 23625012
References
-
- Sobin LH. TNM: evolution and relation to other prognostic factors. Semin Surg Oncol. 2003;21:3–7. - PubMed
-
- Statistics UcoCSCaA. Clinical Stage Classification and Presentation of Results, Malignant Tumours of the Breast and Larynx. Paris: International Union Against Cancer, 1958.
-
- LH. Sobin CWE. TNM Classification of Malignant Tumours, 6th ed. Hoboken, NJ: John Wiley & Sons, 2002.
-
- Sobin LH. TNM. principles, history, and relation to other prognostic factors. Cancer. 2001;91(suppl 8):1589–1592. - PubMed
-
- Demeester SR. Lymph node involvement in esophageal adenocarcinoma: if you see one, have you seen them all? J Thorac Cardiovasc Surg. 2003;126:947–949. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

