Low CD4 count plus coma predicts cryptococcal meningitis in Tanzania
- PMID: 17493266
- PMCID: PMC1876460
- DOI: 10.1186/1471-2334-7-39
Low CD4 count plus coma predicts cryptococcal meningitis in Tanzania
Abstract
Background: Largely due to the lack of diagnostic reagents, the prevalence and clinical presentation of cryptococcal meningitis in Tanzania is poorly understood. This in turn is limiting the impact of increased fluconazole availability.
Methods: We evaluated a cohort of 149 consecutive HIV-infected adult inpatients presenting with headache or altered mental status for clinical features, CD4 count, cryptococcal infection, and outcome. Cryptococcal meningitis was diagnosed via India ink and latex agglutination assay of CSF (n = 24 and 40 positive, respectively). Associations between cryptococcal meningitis and clinical features were evaluated by t-test. The sensitivity, specificity, and positive likelihood ratio of such features were determined.
Results: Cryptococcal meningitis was associated with confusion, social withdrawal, seizures, fever, tachycardia, meningismus, oral candidiasis, and low Glasgow coma scales and CD4 count. CD4 count < 100/mul provided the highest sensitivity for the diagnosis (93%), coma (Glasgow coma scale < or = 8) provided the highest specificity (84%), and the combination provided the highest positive likelihood ratio (3.8). All cryptococcal meningitis patients were initiated on 800 milligrams of fluconazole daily and 50% survived to discharge, however no clinical or laboratory findings correlated with prognosis.
Conclusion: Cryptococcal meningitis is common among Tanzanian HIV inpatients presenting with headache or altered mental status. Purely clinical features are insensitive for establishing the diagnosis or prognosis. We advocate expanding laboratory capacity for cryptococcal antigen testing to maximize survival.
Figures
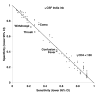
References
-
- Mwaba P, Mwansa J, Chintu C, Pobee J, Scarborough M, Portsmouth S, Zumla A. Clinical presentation, natural history, and cumulative death rates of 230 adults with primary cryptococcal meningitis in Zambian AIDS patients treated under local conditions. Postgrad Med J. 2001;77:769–773. doi: 10.1136/pmj.77.914.769. - DOI - PMC - PubMed
-
- Hakim JG, Gangaidzo IT, Heyderman RS, Mielke J, Mushangi E, Taziwa A, Robertson VJ, Musvaire P, Mason PR. Impact of HIV infection on meningitis in Harare, Zimbabwe: a prospective study of 406 predominantly adult patients. Aids. 2000;14:1401–1407. doi: 10.1097/00002030-200007070-00013. - DOI - PubMed
-
- Corbett EL, Churchyard GJ, Charalambos S, Samb B, Moloi V, Clayton TC, Grant AD, Murray J, Hayes RJ, De Cock KM. Morbidity and mortality in South African gold miners: impact of untreated disease due to human immunodeficiency virus. Clin Infect Dis. 2002;34:1251–1258. doi: 10.1086/339540. - DOI - PubMed
-
- Bekondi C, Bernede C, Passone N, Minssart P, Kamalo C, Mbolidi D, Germani Y. Primary and opportunistic pathogens associated with meningitis in adults in Bangui, Central African Republic, in relation to human immunodeficiency virus serostatus. Int J Infect Dis. 2006;10:387–395. doi: 10.1016/j.ijid.2005.07.004. - DOI - PubMed
-
- Heyderman RS, Gangaidzo IT, Hakim JG, Mielke J, Taziwa A, Musvaire P, Robertson VJ, Mason PR. Cryptococcal meningitis in human immunodeficiency virus-infected patients in Harare, Zimbabwe. Clin Infect Dis. 1998;26:284–289. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

