Central core disease
- PMID: 17504518
- PMCID: PMC1887524
- DOI: 10.1186/1750-1172-2-25
Central core disease
Abstract
Central core disease (CCD) is an inherited neuromuscular disorder characterised by central cores on muscle biopsy and clinical features of a congenital myopathy. Prevalence is unknown but the condition is probably more common than other congenital myopathies. CCD typically presents in infancy with hypotonia and motor developmental delay and is characterized by predominantly proximal weakness pronounced in the hip girdle; orthopaedic complications are common and malignant hyperthermia susceptibility (MHS) is a frequent complication. CCD and MHS are allelic conditions both due to (predominantly dominant) mutations in the skeletal muscle ryanodine receptor (RYR1) gene, encoding the principal skeletal muscle sarcoplasmic reticulum calcium release channel (RyR1). Altered excitability and/or changes in calcium homeostasis within muscle cells due to mutation-induced conformational changes of the RyR protein are considered the main pathogenetic mechanism(s). The diagnosis of CCD is based on the presence of suggestive clinical features and central cores on muscle biopsy; muscle MRI may show a characteristic pattern of selective muscle involvement and aid the diagnosis in cases with equivocal histopathological findings. Mutational analysis of the RYR1 gene may provide genetic confirmation of the diagnosis. Management is mainly supportive and has to anticipate susceptibility to potentially life-threatening reactions to general anaesthesia. Further evaluation of the underlying molecular mechanisms may provide the basis for future rational pharmacological treatment. In the majority of patients, weakness is static or only slowly progressive, with a favourable long-term outcome.
Figures

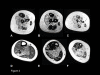
Similar articles
-
Ryanodine receptor mutations in malignant hyperthermia and central core disease.Hum Mutat. 2000;15(5):410-7. doi: 10.1002/(SICI)1098-1004(200005)15:5<410::AID-HUMU2>3.0.CO;2-D. Hum Mutat. 2000. PMID: 10790202 Review.
-
Mutations in RYR1 in malignant hyperthermia and central core disease.Hum Mutat. 2006 Oct;27(10):977-89. doi: 10.1002/humu.20356. Hum Mutat. 2006. PMID: 16917943 Review.
-
Central core disease is due to RYR1 mutations in more than 90% of patients.Brain. 2006 Jun;129(Pt 6):1470-80. doi: 10.1093/brain/awl077. Epub 2006 Apr 18. Brain. 2006. PMID: 16621918
-
Magnetic resonance imaging of muscle in congenital myopathies associated with RYR1 mutations.Neuromuscul Disord. 2004 Dec;14(12):785-90. doi: 10.1016/j.nmd.2004.08.006. Neuromuscul Disord. 2004. PMID: 15564033
-
Functional properties of RYR1 mutations identified in Swedish patients with malignant hyperthermia and central core disease.Anesth Analg. 2010 Jul;111(1):185-90. doi: 10.1213/ANE.0b013e3181cbd815. Epub 2010 Feb 8. Anesth Analg. 2010. PMID: 20142353
Cited by
-
Mild Clinical Features and Histopathologically Atypical Cores in Two Korean Families with Central Core Disease Harboring RYR1 Mutations at the C-Terminal Region.J Clin Neurol. 2015 Jan;11(1):97-101. doi: 10.3988/jcn.2015.11.1.97. Epub 2014 Nov 11. J Clin Neurol. 2015. PMID: 25628744 Free PMC article.
-
Adolescent idiopathic scoliosis without limb weakness: a differential diagnosis of core myopathy?BMC Musculoskelet Disord. 2015 Aug 5;16:179. doi: 10.1186/s12891-015-0629-8. BMC Musculoskelet Disord. 2015. PMID: 26242231 Free PMC article.
-
Oxidative stress and successful antioxidant treatment in models of RYR1-related myopathy.Brain. 2012 Apr;135(Pt 4):1115-27. doi: 10.1093/brain/aws036. Epub 2012 Mar 14. Brain. 2012. PMID: 22418739 Free PMC article.
-
Joint hypermobility as a distinctive feature in the differential diagnosis of myopathies.J Neurol. 2009 Jan;256(1):13-27. doi: 10.1007/s00415-009-0105-1. Epub 2009 Feb 9. J Neurol. 2009. PMID: 19221853 Review.
-
Ion Channel Gene Mutations Causing Skeletal Muscle Disorders: Pathomechanisms and Opportunities for Therapy.Cells. 2021 Jun 16;10(6):1521. doi: 10.3390/cells10061521. Cells. 2021. PMID: 34208776 Free PMC article. Review.
References
-
- McKusick VA. In: Mendelian Inheritance in Man. 12th edition. Press TJHU, editor. Baltimore , Johns Hopkins University Press; 1998.
-
- Wallgren-Pettersson C. Commentationes Physico Mathematicae. University of Helsinki; 1990. Congenital nemaline myopathy: a longitudinal study.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

