Use of gabapentin for perioperative pain control -- a meta-analysis
- PMID: 17505569
- PMCID: PMC2670715
- DOI: 10.1155/2007/840572
Use of gabapentin for perioperative pain control -- a meta-analysis
Abstract
Background: Gabapentin, an anticonvulsant, has recently been suggested as an effective postoperative 'analgesic' agent. The objective of the present study was to examine the analgesic effectiveness, opioid-sparing effects and side effects associated with the use of gabapentin in a perioperative setting.
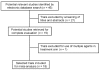
Methods: Following the Quality of Reporting of Meta-analyses recommendations, nine electronic databases until February 2006 were searched, without language restriction, for randomized controlled trials comparing gabapentin with control for postoperative pain control. Outcome measures, namely, 24 h cumulative opioid consumption, visual analogue scale pain scores and adverse effects, were expressed as odds ratios, ratio of means or weighted mean differences (as appropriate), which were aggregated under the fixed or random effects models.
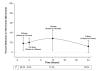
Results: Gabapentin caused a 35% reduction in total opioid consumption over the first 24 h following surgery (ratio of means 0.65, 95% CI 0.59 to 0.72), a significant reduction in postoperative pain at rest (in the first 24 h) and with movement (at 2 h, 4 h and 12 h), regardless of whether treatment effects were expressed as ratios of means or weighted mean differences, and a reduction of vomiting (relative risk [RR] 0.73, 95% CI 0.56 to 0.95) and pruritus (RR 0.30, 95% CI 0.13 to 0.70). It was associated with a significant increase in dizziness (RR 1.40, 95% CI 1.06 to 1.84) and an increase in sedation of borderline significance (RR 1.65, 95% CI 1.00 to 2.74).
Conclusion: Gabapentin improves the analgesic efficacy of opioids both at rest and with movement, reduces analgesic consumption and opioid-related adverse effects, but is associated with an increased incidence of sedation and dizziness.
CONTEXTE :: La gabapentine, un anticonvulsivant, se montrerait également un analgésique postopératoire efficace, d’après des observations récentes. La présente étude avait pour but d’examiner l’efficacité analgésique du médicament, son effet d’épargne d’opioïdes et ses effets indésirables en phase périopératoire.
MÉTHODE :: À la suite des recommandations sur la qualité des rapports de méta-analyses, une recherche a été entreprise dans neuf bases de données électroniques et poursuivie jusqu’en février 2006, sans restriction de langue, sur des essais réalisés avec hasardisation, comparant la gabapentine à des traitements témoins pour le soulagement de la douleur périopératoire. Les mesures de résultats, soit la consommation cumulée d’opioïdes sur 24 h, les cotations de la douleur sur une échelle visuelle analogue et les effets indésirables, ont été exprimées sous forme de risque relatif approché, de rapports de moyennes ou d’écarts de moyennes pondérées, selon le cas, puis intégrées globalement dans les modèles à effets fixes ou à effets aléatoires.
RÉSULTATS :: La gabapentine a permis une réduction de 35 % de la consommation totale d’opioïdes au cours des 24 premières heures postopératoires (rapport des moyennes : 0,65; intervalle de confiance [IC] à 95 % : 0,59 – 0,72), une diminution significative de la douleur postopératoire au repos, au cours des 24 premières heures, et au moment de l’exécution des mouvements, au bout de 2 h, de 4 h et de 12 h, peu importe que les effets du traitement aient été exprimés sous forme de rapports de moyennes ou d’écarts de moyennes pondérées, ainsi qu’une diminution des vomissements (risque relatif [RR] : 0,73; IC à 95 % : 0,56–0,95) et du prurit (RR : 0,30; IC à 95 % : 0,13 – 0,70). Par contre, le médicament a été associé à une augmentation significative des étourdissements (RR : 1,40; IC à 95 % : 1,06 – 1,84) et à une augmentation significativement limite de la sédation (RR : 1,65; IC à 95 % : 1,00 – 2,74).
CONCLUSION :: La gabapentine augmente l’efficacité analgésique des opioïdes, tant au repos qu’à l’exécution des mouvements, diminue la consommation d’analgésiques et les effets indésirables liés aux opioïdes, mais elle est associée à une augmentation de l’incidence de la sédation et des étourdissements.
Figures

Similar articles
-
Analgesic effects of gabapentin after scoliosis surgery in children: a randomized controlled trial.Paediatr Anaesth. 2014 Dec;24(12):1239-44. doi: 10.1111/pan.12524. Epub 2014 Sep 17. Paediatr Anaesth. 2014. PMID: 25230144 Clinical Trial.
-
Is gabapentin effective and safe in open hysterectomy? A PRISMA compliant meta-analysis of randomized controlled trials.J Clin Anesth. 2017 Sep;41:76-83. doi: 10.1016/j.jclinane.2017.07.002. Epub 2017 Jul 18. J Clin Anesth. 2017. PMID: 28802618 Review.
-
The Efficacy of Preoperative Gabapentin in Spinal Surgery: A Meta-Analysis of Randomized Controlled Trials.Pain Physician. 2017 Nov;20(7):649-661. Pain Physician. 2017. PMID: 29149144 Review.
-
The analgesic effects of perioperative gabapentin on postoperative pain: a meta-analysis.Reg Anesth Pain Med. 2006 May-Jun;31(3):237-47. doi: 10.1016/j.rapm.2006.01.005. Reg Anesth Pain Med. 2006. PMID: 16701190
-
Gabapentin use in pediatric spinal fusion patients: a randomized, double-blind, controlled trial.Anesth Analg. 2010 May 1;110(5):1393-8. doi: 10.1213/ANE.0b013e3181d41dc2. Anesth Analg. 2010. PMID: 20418301 Clinical Trial.
Cited by
-
Adding pregabalin to a multimodal analgesic regimen does not reduce pain scores following cosmetic surgery: a randomized trial.J Anesth. 2012 Dec;26(6):829-35. doi: 10.1007/s00540-012-1447-x. Epub 2012 Jul 14. J Anesth. 2012. PMID: 22797880 Clinical Trial.
-
The use of gabapentin in the management of postoperative pain after total hip arthroplasty: a meta-analysis of randomised controlled trials.J Orthop Surg Res. 2016 Jul 12;11(1):79. doi: 10.1186/s13018-016-0412-z. J Orthop Surg Res. 2016. PMID: 27405805 Free PMC article. Review.
-
A Narrative Review on Perioperative Pain Management Strategies in Enhanced Recovery Pathways-The Past, Present and Future.J Clin Med. 2021 Jun 10;10(12):2568. doi: 10.3390/jcm10122568. J Clin Med. 2021. PMID: 34200695 Free PMC article. Review.
-
Efficacy of Pregabalin in Acute Postoperative Pain Under Different Surgical Categories: A Meta-Analysis.Medicine (Baltimore). 2015 Nov;94(46):e1944. doi: 10.1097/MD.0000000000001944. Medicine (Baltimore). 2015. PMID: 26579802 Free PMC article.
-
The efficacy of perioperative gabapentin for the treatment of postoperative pain following total knee and hip arthroplasty: a meta-analysis.J Orthop Surg Res. 2020 Aug 15;15(1):332. doi: 10.1186/s13018-020-01849-6. J Orthop Surg Res. 2020. PMID: 32799902 Free PMC article. Review.
References
-
- Apfelbaum JL, Chen C, Mehta S, Gan TJ. Postoperative pain experience: Results from a national survey suggest postoperative pain continues to be undermanaged. Anesth Analg. 2003;97:534–40. - PubMed
-
- Warfield CA, Kahn CH. Acute pain management: Programs in U.S. hospitals and experiences and attitudes among U.S. adults. Anesthesiology. 1995;83:1090–4. - PubMed
-
- Austrup ML, Korean G. Analgesic agents for the postoperative period. Opioids. Surg Clin North Am. 1999;79:253–73. - PubMed
-
- Wheeler M, Oderda GM, Ashburn MA, Lipman AG. Adverse events associated with postoperative opioid analgesia: A systemic review. J Pain. 2002;3:159–80. - PubMed
-
- Oderda GM, Evans S, Lloyd J, et al. Cost of opioid-related adverse drug events in surgical patients. J Pain Symptom Manage. 2003;25:276–83. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

