Mild episodes of tourniquet-induced forearm ischaemia-reperfusion injury results in leukocyte activation and changes in inflammatory and coagulation markers
- PMID: 17537260
- PMCID: PMC1890284
- DOI: 10.1186/1476-9255-4-12
Mild episodes of tourniquet-induced forearm ischaemia-reperfusion injury results in leukocyte activation and changes in inflammatory and coagulation markers
Abstract
Background: Monocytes and neutrophils are examples of phagocytic leukocytes, with neutrophils being considered as the 'chief' phagocytic leukocyte. Both monocytes and neutrophils have been implicated to play a key role in the development of ischaemia-reperfusion injury, where they are intrinsically involved in leukocyte-endothelial cell interactions. In this pilot study we hypothesised that mild episodes of tourniquet induced forearm ischaemia-reperfusion injury results in leukocyte activation and changes in inflammatory and coagulation markers.
Methods: Ten healthy human volunteers were recruited after informed consent. None had any history of cardiovascular disease with each subject volunteer participating in the study for a 24 hour period. Six venous blood samples were collected from each subject volunteer at baseline, 10 minutes ischaemia, 5, 15, 30, 60 minutes and 24 hours reperfusion, by means of a cannula from the ante-cubital fossa. Monocyte and neutrophil leukocyte sub-populations were isolated by density gradient centrifugation techniques. Leukocyte trapping was investigated by measuring the concentration of leukocytes in venous blood leaving the arm. The cell surface expression of CD62L (L-selectin), CD11b and the intracellular production of hydrogen peroxide (H2O2) were measured via flow cytometry. C-reactive protein (CRP) was measured using a clinical chemistry analyser. Plasma concentrations of D-dimer and von Willebrand factor (vWF) were measured using enzyme-linked fluorescent assays (ELFA).
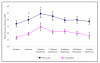
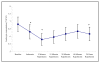
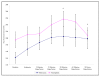
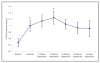
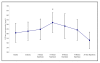
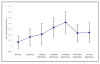
Results: During ischaemia-reperfusion injury, there was a decrease in CD62L and an increase in CD11b cell surface expression for both monocytes and neutrophils, with changes in the measured parameters reaching statistical significance (p =< 0.05). A significant decrease in peripheral blood leukocyte concentration was observed during this process, which was measured to assess the degree of leukocyte trapping in the micro-circulation (p =< 0.001). There was an increase in the intracellular production of H2O2 production by leukocyte sub-populations, which was measured as a marker of leukocyte activation. Intracellular production of H2O2 in monocytes during ischaemia-reperfusion injury reached statistical significance (p = 0.014), although similar trends were observed with neutrophils these did not reach statistical significance. CRP was measured to assess the inflammatory response following mild episodes of ischaemia-reperfusion injury and resulted in a significant increase in the CRP concentration (p =< 0.001). There were also increased plasma concentrations of D-dimer and a trend towards elevated vWF levels, which were measured as markers of coagulation activation and endothelial damage respectively. Although significant changes in D-dimer concentrations were observed during ischaemia-reperfusion injury (p = 0.007), measurement of the vWF did not reach statistical significance.
Conclusion: Tourniquet induced forearm ischaemia-reperfusion injury results in increased adhesiveness, trapping and activation of leukocytes. We report that, even following a mild ischaemic insult, this leukocyte response is immediately followed by evidence of increased inflammatory response, coagulation activity and endothelial damage. These results may have important implications and this pilot study may lead to a series of trials that shed light on the mechanisms of ischaemia-reperfusion injury, including potential points of therapeutic intervention for pathophysiological conditions.
Figures


References
-
- Babior BM. Neutrophil function as related to neutrophil-endothelial cell interactions. Nonv Rev Fr Hematol. 1992;34:S29–S35. - PubMed
-
- Hughes SF, Cotter MJ, Evans S-A, Jones KP, Adams RA. The role of leukocytes in damage to the vascular endothelium during ischaemia-reperfusion injury. Br J Biomed Sci. 2006;63:166–170. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

