Evaluation of the GenoType MTBDRplus assay for rifampin and isoniazid susceptibility testing of Mycobacterium tuberculosis strains and clinical specimens
- PMID: 17537937
- PMCID: PMC1951233
- DOI: 10.1128/JCM.00521-07
Evaluation of the GenoType MTBDRplus assay for rifampin and isoniazid susceptibility testing of Mycobacterium tuberculosis strains and clinical specimens
Abstract
The new GenoType MTBDRplus assay (Hain Lifescience GmbH, Nehren, Germany) was tested with 125 clinical isolates and directly with 72 smear-positive sputum specimens for its ability to detect rifampin (RMP) and isoniazid (INH) resistance in Mycobacterium tuberculosis complex (MTBC) strains. In total, 106 RMP(r)/INH(r), 10 RMP(s)/INH(r), and 80 RMP(s)/INH(s) MTBC strains were comparatively analyzed with the new and the old MTBDR assays. Besides the detection of mutations within the 81-bp hot spot region of rpoB and katG codon 315, the GenoType MTBDRplus assay is designed to detect mutations in the regulatory region of inhA. The applicability of the new assay directly to specimens was shown, since 71 of 72 results for smear-positive sputa and all 125 results for clinical isolates were interpretable and no discrepancies compared with the results of real-time PCR or DNA sequencing were obtained. In comparison to conventional drug susceptibility testing, both assays were able to identify RMP resistance correctly in 74 of 75 strains (98.7%) and 30 of 31 specimens (96.8%). The misidentification of RMP resistance was obtained for two strains containing rpoB P533L mutations. Compared to the old MTBDR assay, the new GenoType MTBDRplus assay enhanced the rate of detection of INH resistance from 66 (88.0%) to 69 (92.0%) among the 75 INH-resistant strains and 36 (87.8%) to 37 (90.2%) among the 41 specimens containing INH-resistant strains. Thus, the new GenoType MTBDRplus assay represents a reliable and upgraded tool for the detection of INH and RMP resistance in strains or directly from smear-positive specimens.
Figures
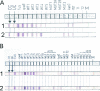
References
-
- Bártfai, Z., Á. Somoskövi, C. Ködmön, N. Szabó, E. Puskás, L. Kosztolányi, E. Faragó, J. Mester, L. M. Parsons, and M. Salfinger. 2001. Molecular characterization of rifampin-resistant isolates of Mycobacterium tuberculosis from Hungary by DNA sequencing and the line probe assay. J. Clin. Microbiol. 39:3736-3739. - PMC - PubMed
-
- Deutsches Institut für Normung. 1986. Medical microbiology. Diagnosis of tuberculosis. Parts 3 and 32. Beuth Verlag, Berlin, Germany.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

