Time-dependent changes in pulmonary surfactant function and composition in acute respiratory distress syndrome due to pneumonia or aspiration
- PMID: 17662121
- PMCID: PMC1950506
- DOI: 10.1186/1465-9921-8-55
Time-dependent changes in pulmonary surfactant function and composition in acute respiratory distress syndrome due to pneumonia or aspiration
Abstract
Background: Alterations to pulmonary surfactant composition have been encountered in the Acute Respiratory Distress Syndrome (ARDS). However, only few data are available regarding the time-course and duration of surfactant changes in ARDS patients, although this information may largely influence the optimum design of clinical trials addressing surfactant replacement therapy. We therefore examined the time-course of surfactant changes in 15 patients with direct ARDS (pneumonia, aspiration) over the first 8 days after onset of mechanical ventilation.
Methods: Three consecutive bronchoalveolar lavages (BAL) were performed shortly after intubation (T0), and four days (T1) and eight days (T2) after intubation. Fifteen healthy volunteers served as controls. Phospholipid-to-protein ratio in BAL fluids, phospholipid class profiles, phosphatidylcholine (PC) molecular species, surfactant proteins (SP)-A, -B, -C, -D, and relative content and surface tension properties of large surfactant aggregates (LA) were assessed.
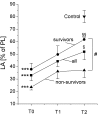
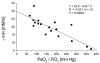
Results: At T0, a severe and highly significant reduction in SP-A, SP-B and SP-C, the LA fraction, PC and phosphatidylglycerol (PG) percentages, and dipalmitoylation of PC (DPPC) was encountered. Surface activity of the LA fraction was greatly impaired. Over time, significant improvements were encountered especially in view of LA content, DPPC, PG and SP-A, but minimum surface tension of LA was not fully restored (15 mN/m at T2). A highly significant correlation was observed between PaO2/FiO2 and minimum surface tension (r = -0.83; p < 0.001), SP-C (r = 0.64; p < 0.001), and DPPC (r = 0.59; p = 0.003). Outcome analysis revealed that non-survivors had even more unfavourable surfactant properties as compared to survivors.
Conclusion: We concluded that a profound impairment of pulmonary surfactant composition and function occurs in the very early stage of the disease and only gradually resolves over time. These observations may explain why former surfactant replacement studies with a short treatment duration failed to improve outcome and may help to establish optimal composition and duration of surfactant administration in future surfactant replacement studies in acute lung injury.
Figures

References
-
- Veldhuizen R, Nag K, Orgeig S, Possmayer F. The role of lipids in pulmonary surfactant. Biochim Biophys Acta. 1998;1408:90–108. - PubMed
-
- Pison U, Seeger W, Buchhorn R, Joka T, Brand M, Obertacke U, Neuhof H, Schmit-Neuerburg KP. Surfactant abnormalities in patients with respiratory failure after multiple trauma. Am Rev Respir Dis. 1989;140:1033–1039. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

