Sleep disorders in chronic traumatic brain injury
- PMID: 17694723
- PMCID: PMC1978305
Sleep disorders in chronic traumatic brain injury
Abstract
Study objective: To examine the spectrum of sleep disorders in patients with chronic traumatic brain injury (TBI) and determine if the severity of sleep disorder is related to severity of chronic TBI.
Methods: Patients who underwent evaluation for sleep disorder/s following a TBI were included in this retrospective analysis. Sixty adult patients with TBI (age 20-69 yr; 38 M and 22 F), who presented with sleep-related complaints 3 months to 2 years following TBI, were studied. None had sleep complaints prior to the TBI. Orophrayngeal, chin, and TMJ examinations were considered benign. The severity of injury was assessed by the Global Assessment of Functioning (GAF) scale. Polysomnograms (PSGs) were performed on 54 patients (90%), 28 of whom underwent multiple sleep latency tests (MSLTs) because they scored >11 on the Epworth Sleepiness Scale (ESS). The Beck Depression Inventory (BDI) scale was administered if there was sleep maintenance insomnia, and the Hamilton Anxiety Scale (HAS) was administered if there was sleep onset insomnia.
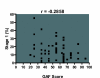
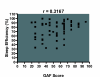
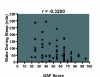
Results: The TBI severity was mild in 40%, moderate in 20%, and severe in 40%. The Epworth Sleepiness Scale (ESS) score was elevated (>11) in 52%. Hypersomnia was the presenting complaint in 50%, mostly due to sleep apnea, narcolepsy, and periodic limb movement disorder (PLMD). Insomnia was the presenting complaint in 25%, half with sleep maintenance insomnia and high BDI scores, and the remainder with sleep onset insomnia and high HAS scores. Parasomnia was the presenting complaint in 25%; the most frequent parasomnia was REM behavior disorder (RBD). GAF scores were significantly correlated (p < 0.05) with some of the measures of sleep disruption (stage 1, sleep efficiency, and wake during sleep), but not with others (wake before sleep, stage-shifts, PLMI, PLMA and AHI) on the PSG. Fifty-three percent (15/28) had a mean sleep onset latency <5 minutes, and 32% (9/28), also had two or more sleep onset rapid eye movement periods (SOREMPs) on the MSLT.
Conclusion: The results of this study demonstrate that a full spectrum of common sleep disorders occurs in patients with chronic TBI. The severity of chronic TBI as measured by GAF scores is correlated with some of the measures of sleep disruption but not others, indicating a complex and multifactorial pathogenesis.
Figures
Comment in
-
Is the silent epidemic keeping patients awake?J Clin Sleep Med. 2007 Jun 15;3(4):347-8. J Clin Sleep Med. 2007. PMID: 17694721 Free PMC article. No abstract available.
References
-
- Parker F, Andrews PJD, Azouvi P, Aghakhani N, Perrouin-Verbe B. Acute Traumatic brain injury. Continuum. 2001;7:7–31.
-
- Gill AW. Idiopathic and traumatic narcolepsy. Lancet. 1941;1:474–6.
-
- Amico G, Pasquali F, Pittaluga E. Pickwickian-narcoleptic disorders after brain concussion. Riv Sper Freniatr Med Leg Alien Ment. 1972;29:74–85. - PubMed
-
- Guilleminault C, Faull K, Miles L, Van den Hoed J. Post-traumatic excessive daytime sleepiness: a review of 20 patients. Neurology. 1982;33:1584–9. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
