Prior authorization of newer insomnia medications in managed care: is it cost saving?
- PMID: 17694729
- PMCID: PMC1978307
Prior authorization of newer insomnia medications in managed care: is it cost saving?
Abstract
Study objectives: New pharmacotherapeutic treatment options are available to treat patients with 1 or more insomnia symptoms. However, these new pharmaceuticals are subject to a variety of managed-care tools, such as prior authorizations, that may restrict access to these medications. The objective of this study was to evaluate the economic consequences to a health plan that requires prior authorization for nonbenzodiazepine medications approved for the treatment of insomnia characterized by difficulties both falling and staying asleep.
Methods: An economic model was constructed to determine the effects of a typical prior-authorization program across a hypothetical managed-care population. Model parameters were derived from national estimates and a literature review.
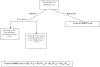
Results: Economic consequences of a prior-authorization program were based on a hypothetical managed-care plan with 500,000 insured patients. An estimated acquisition cost of $300 per 100 tablets of medication requiring prior authorization, $40 to process each priorauthorization request, and prior-authorization rejection rates of 2% to 5% were considered. Using the default-model inputs of the hypothetical plan characteristics and costs, the economic model estimated a loss of $600,000 to $700,000 per year to the health plan. In a 3-way threshold sensitivity analysis when prior-authorization rejection rate was increased to 5%, the cost of each request in the prior-authorization program was decreased to $20, and the cost of a first-generation nonbenzodiazepine was decreased to a generic price (i.e. $100 per prescription), the model continued to show a net loss to managed care in each case.
Conclusions: This model showed that requiring prior authorization for newer sleep treatments might not be a cost-saving strategy for managed-care organizations.
Figures
Similar articles
-
Will insomnia treatments produce overall cost savings to commercial managed-care plans? A predictive analysis in the United States.Curr Med Res Opin. 2007 Jun;23(6):1431-43. doi: 10.1185/030079907X199619. Epub 2007 May 17. Curr Med Res Opin. 2007. PMID: 17559740
-
Prior authorization for topical psoriasis treatments: is it cost-beneficial for managed care?J Dermatolog Treat. 2010 May;21(3):178-84. doi: 10.3109/09546630903268247. J Dermatolog Treat. 2010. PMID: 19821787
-
Chronic insomnia treatment and Medicare Part D: implications for managed care organizations.Am J Manag Care. 2007 Nov;13(5 Suppl):S121-4. Am J Manag Care. 2007. PMID: 18041872 Review.
-
The role of eszopiclone in the treatment of insomnia.Adv Ther. 2009 May;26(5):500-18. doi: 10.1007/s12325-009-0026-5. Epub 2009 Jun 2. Adv Ther. 2009. PMID: 19513631 Review.
-
Cost-effectiveness of eszopiclone for the treatment of adults with primary chronic insomnia.Sleep. 2009 Jun;32(6):817-24. doi: 10.1093/sleep/32.6.817. Sleep. 2009. PMID: 19544759 Free PMC article.
Cited by
-
Prevalence and factors associated with off-label antidepressant prescriptions for insomnia.Drug Healthc Patient Saf. 2011;3:27-36. doi: 10.2147/DHPS.S21079. Epub 2011 Jul 8. Drug Healthc Patient Saf. 2011. PMID: 21904465 Free PMC article.
References
-
- Smith C, Cowan C, Heffler S, Catlin A. National health spending in 2004: recent slowdown led by prescription drug spending. Health Aff. 2006;25:186–96. - PubMed
-
- Cunningham PJ. Medicaid cost containment and access to prescription drugs. Health Aff. 2005;24:780–9. - PubMed
-
- Olson BM. Approaches to pharmacy benefit management and the impact of consumer cost sharing. Clin Ther. 2003;25:250–72. - PubMed
-
- Ranjan JN. Medicaid and the unconstitutional dimensions of prior authorization. Mich Law Rev. 2002;101:602–47. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
