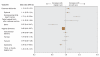
Comparison of obstetric outcomes between on-call and patients' own obstetricians
- PMID: 17698823
- PMCID: PMC1942095
- DOI: 10.1503/cmaj.060920
Comparison of obstetric outcomes between on-call and patients' own obstetricians
Abstract
Background: The question "will you be delivering my baby?" is one that pregnant women frequently ask their physicians. We sought to determine whether obstetric outcomes differed between women whose babies were delivered by their own obstetrician (regular-care obstetrician) and those attended by an on-call obstetrician who did not provide antenatal care.
Methods: We performed a cohort study of all live singleton term births between 1991 and 2001 at the Royal Victoria Hospital in Montréal. We excluded breech deliveries, elective cesarean sections and deliveries with placenta previa or prolapse of the umbilical cord. Logistic regression analysis was used to compare obstetric outcomes (e.g., cesarean delivery, instrumental vaginal delivery and episiotomy) between the regular-care and on-call obstetricians after adjustment for potential confounders.
Results: A total of 28,332 eligible deliveries were attended by 26 obstetricians: 21,779 (76.9%) by the patient's own obstetrician and 6553 (23.1%) by the on-call obstetrician. Compared with women attended by their regular-care obstetrician, those attended by an on-call obstetrician had higher rates of cesarean delivery (11.9% v. 11.4%, adjusted odds ratio [OR] 1.13, 95% confidence interval [CI] 1.03-1.24, p < 0.01) and of third-or fourth-degree tears (7.9% v. 6.4%, adjusted OR 1.21, 95% CI 1.07-1.36, p < 0.01) but lower rates of episiotomy (38.5% v. 42.9%, OR 0.77, 95% CI 0.72-0.82, p < 0.001). No differences were observed between the groups in the rate of instrumental vaginal delivery. The increase in the overall rate of cesarean delivery among women attended by an on-call obstetrician was due mainly to an increase in cesarean deliveries during the first stage of labour because of nonreassuring fetal heart tracing (2.9% v. 1.7%, adjusted OR 1.79, 95% CI 1.49-2.15, p < 0.001). The time of day of delivery did not modify the observed effects.
Interpretation: The type of attending obstetrician (regular care v. on call) had a minor effect on obstetric outcomes.
Figures
Comment in
-
"You're not my obstetrician" (and it may not matter).CMAJ. 2007 Aug 14;177(4):372-3. doi: 10.1503/cmaj.070904. CMAJ. 2007. PMID: 17698827 Free PMC article. No abstract available.
Similar articles
-
Obstetrician call schedule and obstetric outcomes among women eligible for a trial of labor after cesarean.Am J Obstet Gynecol. 2017 Jan;216(1):75.e1-75.e6. doi: 10.1016/j.ajog.2016.08.032. Epub 2016 Aug 30. Am J Obstet Gynecol. 2017. PMID: 27589899 Free PMC article.
-
Practice variations between family physicians and obstetricians in the management of low-risk pregnancies.J Fam Pract. 1995 Apr;40(4):345-51. J Fam Pract. 1995. PMID: 7699347
-
Cohort study of operative delivery in the second stage of labour and standard of obstetric care.BJOG. 2003 Jun;110(6):610-5. BJOG. 2003. PMID: 12798481
-
Cesarean section on request at 39 weeks: impact on shoulder dystocia, fetal trauma, neonatal encephalopathy, and intrauterine fetal demise.Semin Perinatol. 2006 Oct;30(5):276-87. doi: 10.1053/j.semperi.2006.07.009. Semin Perinatol. 2006. PMID: 17011400 Review.
-
Management trend and safety of vaginal delivery for term breech fetuses in a tertiary care hospital of Karachi, Pakistan.J Perinat Med. 2001;29(3):250-9. doi: 10.1515/JPM.2001.036. J Perinat Med. 2001. PMID: 11447931 Review.
Cited by
-
Association between Maternal Mortality and Cesarean Section: Turkey Experience.PLoS One. 2016 Nov 23;11(11):e0166622. doi: 10.1371/journal.pone.0166622. eCollection 2016. PLoS One. 2016. PMID: 27880841 Free PMC article.
-
Obstetricians' Attitude towards Childbirth.Int J Environ Res Public Health. 2021 Oct 11;18(20):10650. doi: 10.3390/ijerph182010650. Int J Environ Res Public Health. 2021. PMID: 34682397 Free PMC article.
-
"You're not my obstetrician" (and it may not matter).CMAJ. 2007 Aug 14;177(4):372-3. doi: 10.1503/cmaj.070904. CMAJ. 2007. PMID: 17698827 Free PMC article. No abstract available.
-
Obstetrician call schedule and obstetric outcomes among women eligible for a trial of labor after cesarean.Am J Obstet Gynecol. 2017 Jan;216(1):75.e1-75.e6. doi: 10.1016/j.ajog.2016.08.032. Epub 2016 Aug 30. Am J Obstet Gynecol. 2017. PMID: 27589899 Free PMC article.
-
Processes of obstetrical care and outcomes among Ontario physicians versus non-physicians: a population-based study.BMJ Open. 2024 Dec 15;14(12):e091312. doi: 10.1136/bmjopen-2024-091312. BMJ Open. 2024. PMID: 39675822 Free PMC article.
References
-
- Borenstein SH, Choi M, Gerstle JT, et al. Errors and adverse outcomes on a surgical service: What is the role of residents? J Surg Res 2004;122:162-6. - PubMed
-
- Goldberg J, Gopal M, Singhal R, et al. Nighttime call in house vs. out of house: a comparison of obstetric procedure rates. J Reprod Med 2004;49:143-7. - PubMed
-
- Jakubowicz DM, Price EM, Glassman HJ, et al. Effects of a twenty-four hour call period on resident performance during simulated endoscopic sinus surgery in an accreditation council for graduate medical education-compliant training program. Laryngoscope 2005;115:143-6. - PubMed
-
- Mann FA, Danz PL. The night stalker effect: quality improvements with a dedicated night-call rotation. Invest Radiol 1993;28:92-6. - PubMed
-
- Scotti RJ. Compliance with the 24-hour, in-house attending coverage requirement. A survey. J Reprod Med 1995;40:101-6. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous