Very prematurely born infants wheezing at follow-up: lung function and risk factors
- PMID: 17715441
- PMCID: PMC2084021
- DOI: 10.1136/adc.2006.112623
Very prematurely born infants wheezing at follow-up: lung function and risk factors
Abstract
Objectives: To determine whether abnormalities of lung volume and/or airway function were associated with wheeze at follow-up in infants born very prematurely and to identify risk factors for wheeze.
Design: Lung function data obtained at 1 year of age were collated from two cohorts of infants recruited into the UKOS and an RSV study, respectively.
Setting: Infant pulmonary function laboratory.
Patients: 111 infants (mean gestational age 26.3 (SD 1.6) weeks).
Interventions: Lung function measurements at 1 year of age corrected for gestational age at birth. Diary cards and respiratory questionnaires were completed to document wheeze.
Main outcome measures: Functional residual capacity (FRC(pleth) and FRC(He)), airways resistance (R(aw)), FRC(He):FRC(pleth) and tidal breathing parameters (T(PTEF):T(E)).
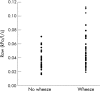
Results: The 60 infants who wheezed at follow-up had significantly lower mean FRC(He), FRC(He):FRC(pleth) and T(PTEF):T(E), but higher mean R(aw) than the 51 without wheeze. Regression analysis demonstrated that gestational age, length at assessment, family history of atopy and a low FRC(He):FRC(pleth) were significantly associated with wheeze.
Conclusions: Wheeze at follow-up in very prematurely born infants is associated with gas trapping, suggesting abnormalities of the small airways.
Conflict of interest statement
Competing interests: None.
References
-
- Bancalari E, Claure N, Sosenko I R. Bronchopulmonary dysplasia: changes in pathogenesis, epidemiology and definition. Semin Neonatol 2003863–71. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical