Unwarranted administration of acetylcholinesterase inhibitors can impair genioglossus and diaphragm muscle function
- PMID: 17893459
- PMCID: PMC3473079
- DOI: 10.1097/01.anes.0000281928.88997.95
Unwarranted administration of acetylcholinesterase inhibitors can impair genioglossus and diaphragm muscle function
Abstract
Background: It is standard practice to administer a cholinesterase inhibitor (e.g., neostigmine) at the end of a surgical case to reverse suspected effects of neuromuscular blocking agents regardless of whether such residual effects are present. The authors hypothesized that cholinesterase inhibition when given the in absence of neuromuscular blockade (NB) would decrease upper airway dilatory muscle activity and consequently upper airway volume.
Methods: The authors measured genioglossus and diaphragm electromyograms during spontaneous ventilation in anesthetized, tracheostomized rats before and after administration of neostigmine (0.03, 0.06, or 0.12 mg/kg), after recovery of the train-of-four ratio (quadriceps femoris muscle) to unity after NB (n = 18). For comparison, the authors made the same measurements in rats that had no previous NB (n = 27). In intact anesthetized rats, the authors measured upper airway volume and end-expiratory lung volume by magnetic resonance imaging before and after 0.12 mg/kg neostigmine (n = 9).
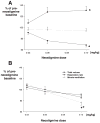
Results: Neostigmine treatment in rats that had fully recovered from NB based on the train-of-four ratio caused dose-dependent decreases in genioglossus electromyogram (to 70.3 +/- 7.6, 49.2 +/- 3.2, and 39.7 +/- 2.3% of control, respectively), decreases in diaphragm electromyogram (to 103.1 +/- 6.5, 83.1 +/- 4.7, and 68.7 +/- 7.3% of control), and decreases in minute ventilation to a nadir value of 79.6 +/- 6% of preneostigmine baseline. Genioglossus electromyogram effects were the same when neostigmine was given with no previous NB. Neostigmine caused a decrease in upper airway volume to 83 +/- 3% of control, whereas end-expiratory lung volume remained constant.
Conclusions: The cholinesterase inhibitor neostigmine markedly impairs upper airway dilator volume, genioglossus muscle function, diaphragmatic function, and breathing when given after recovery from vecuronium-induced neuromuscular block.
Figures




Similar articles
-
Neostigmine/glycopyrrolate administered after recovery from neuromuscular block increases upper airway collapsibility by decreasing genioglossus muscle activity in response to negative pharyngeal pressure.Anesthesiology. 2010 Dec;113(6):1280-8. doi: 10.1097/ALN.0b013e3181f70f3d. Anesthesiology. 2010. PMID: 20980910
-
Neostigmine but not sugammadex impairs upper airway dilator muscle activity and breathing.Br J Anaesth. 2008 Sep;101(3):344-9. doi: 10.1093/bja/aen176. Epub 2008 Jun 16. Br J Anaesth. 2008. PMID: 18559352 Free PMC article.
-
Pentobarbital dose-dependently increases respiratory genioglossus muscle activity while impairing diaphragmatic function in anesthetized rats.Anesthesiology. 2009 Jun;110(6):1327-34. doi: 10.1097/ALN.0b013e3181a16337. Anesthesiology. 2009. PMID: 19417601 Free PMC article.
-
The effects of acetylcholinesterase inhibitors on morbidity after general anesthesia and surgery.Neuropharmacology. 2020 Aug 15;173:108134. doi: 10.1016/j.neuropharm.2020.108134. Epub 2020 May 19. Neuropharmacology. 2020. PMID: 32416089 Review.
-
Atrio-ventricular Block Following Neostigmine-Glycopyrrolate Reversal in Non-heart Transplant Patients: Case Report.Anesth Prog. 2018 Fall;65(3):187-191. doi: 10.2344/anpr-65-03-10. Anesth Prog. 2018. PMID: 30235426 Free PMC article. Review.
Cited by
-
Comparison of the effects of neostigmine and sugammadex on postoperative residual curarization and postoperative pulmonary complications by means of diaphragm and lung ultrasonography: a study protocol for prospective double-blind randomized controlled trial.Trials. 2022 May 7;23(1):376. doi: 10.1186/s13063-022-06328-3. Trials. 2022. PMID: 35526047 Free PMC article.
-
Comparison of Sugammadex versus Neostigmine Costs and Respiratory Complications in Patients with Obstructive Sleep Apnoea.Turk J Anaesthesiol Reanim. 2015 Dec;43(6):387-95. doi: 10.5152/TJAR.2015.35682. Epub 2015 Dec 1. Turk J Anaesthesiol Reanim. 2015. PMID: 27366535 Free PMC article.
-
Optimizing Reversal of Neuromuscular Block in Older Adults: Sugammadex or Neostigmine.Drugs Aging. 2022 Oct;39(10):749-761. doi: 10.1007/s40266-022-00969-4. Epub 2022 Aug 8. Drugs Aging. 2022. PMID: 35934764
-
Perioperative Pulmonary Atelectasis: Part I. Biology and Mechanisms.Anesthesiology. 2022 Jan 1;136(1):181-205. doi: 10.1097/ALN.0000000000003943. Anesthesiology. 2022. PMID: 34499087 Free PMC article. Review.
-
Recovery of muscle function after deep neuromuscular block by means of diaphragm ultrasonography and adductor of pollicis acceleromyography with comparison of neostigmine vs. sugammadex as reversal drugs: study protocol for a randomized controlled trial.Trials. 2018 Feb 21;19(1):135. doi: 10.1186/s13063-018-2525-7. Trials. 2018. PMID: 29467022 Free PMC article.
References
-
- Sundman E, Witt H, Olsson R, Ekberg O, Kuylenstierna R, Eriksson LI. The incidence and mechanisms of pharyngeal and upper esophageal dysfunction in partially paralyzed humans: Pharyngeal videoradiography and simultaneous manometry after atracurium. Anesthesiology. 2000;92:977–84. - PubMed
-
- Eikermann M, Groeben H, Bunten B, Peters J. Fade of pulmonary function during residual neuromuscular blockade. Chest. 2005;127:1703–9. - PubMed
-
- Eikermann M, Groeben H, Husing J, Peters J. Accelerometry of adductor pollicis muscle predicts recovery of respiratory function from neuromuscular blockade. Anesthesiology. 2003;98:1333–7. - PubMed
-
- Eikermann M, Vogt FM, Herbstreit F, Vahid-Dastgerdi M, Zenge MO, Ochterbeck C, de Greiff A, Peters J. The predisposition to inspiratory upper airway collapse during partial neuromuscular blockade. Am J Respir Crit Care Med. 2007;175:9–15. - PubMed
-
- Viby-Mogensen J, Jorgensen BC, Ording H. Residual curarization in the recovery room. Anesthesiology. 1979;50:539–41. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

