Evaluation of a neck-bridge device to assist endovascular treatment of wide-neck aneurysms of the anterior circulation
- PMID: 17928379
- PMCID: PMC8119120
- DOI: 10.3174/ajnr.A0767
Evaluation of a neck-bridge device to assist endovascular treatment of wide-neck aneurysms of the anterior circulation
Abstract
Background and purpose: Intracranial aneurysms with a wide-neck or an unfavorable dome-to-neck ratio may be difficult to treat properly and safely. Our aim was to evaluate the TriSpan neck-bridge device to assist coiling of wide-neck bifurcation aneurysms in the anterior circulation.
Materials and methods: In 14 patients, we performed 16 TriSpan-assisted coil embolizations with wide-neck bifurcation aneurysms of the anterior circulation. Eleven procedures were indicated for acutely ruptured aneurysms. Five were performed electively for the following: recurrent aneurysm after coil only (n = 1) or after TriSpan-assisted embolization (n = 2), aneurysm remnant after clipping (n = 1), and aneurysm incidentally found (n = 1). Procedural and clinical complications were recorded. Follow-up angiography was performed, and clinical outcomes were assessed by using the modified Rankin Scale score.
Results: TriSpan-assisted embolization was successful in 15/16 (93.8%) procedures, with complete occlusion in 2/16 (12.5%), near-complete occlusion in 10/16 (62.5%), and incomplete occlusion in 3/16 (18.75%). There were 6 (37.5%) intraprocedural complications: thrombus formation (n = 3), protrusion of a TriSpan loop in the parent artery (n = 1), TriSpan displacement in the aneurysm (n = 1), and tangling of a coil loop in the device (n = 1). Three patients died in the hospital (21.4%). Follow-up angiography or MR angiography was available in 8 (57.1%) patients and showed complete (n = 2), near-complete (n = 2), and incomplete occlusion (n = 4). Long-term clinical outcome was no (n = 4) or minor symptoms (n = 1) and moderate (n = 2), moderately severe (n = 2), or severe handicap (n = 2).
Conclusion: The use of the TriSpan device is feasible in the anterior circulation and can assist treatment of difficult wide-neck bifurcation aneurysms.
Figures
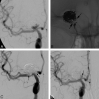

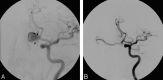
Similar articles
-
Neck-bridge device for endovascular treatment of wide-neck bifurcation aneurysms: initial experience.Radiology. 2001 Nov;221(2):318-26. doi: 10.1148/radiol.2212010474. Radiology. 2001. PMID: 11687670
-
Neuroform stent-assisted coil embolization of wide-neck intracranial aneurysms: strategies in stent deployment and midterm follow-up.Neurosurgery. 2007 Sep;61(3):460-8; discussion 468-9. doi: 10.1227/01.NEU.0000290890.62201.A9. Neurosurgery. 2007. PMID: 17881956
-
One-Year Angiographic Follow-Up after WEB-SL Endovascular Treatment of Wide-Neck Bifurcation Intracranial Aneurysms.AJNR Am J Neuroradiol. 2015 Dec;36(12):2320-4. doi: 10.3174/ajnr.A4457. Epub 2015 Aug 20. AJNR Am J Neuroradiol. 2015. PMID: 26294645 Free PMC article.
-
Pivotal Trial of the Neuroform Atlas Stent for Treatment of Anterior Circulation Aneurysms: One-Year Outcomes.Stroke. 2020 Jul;51(7):2087-2094. doi: 10.1161/STROKEAHA.119.028418. Epub 2020 Jun 17. Stroke. 2020. PMID: 32568654 Free PMC article. Clinical Trial.
-
Selection of cerebral aneurysms for treatment using Guglielmi detachable coils: the preliminary University of Illinois at Chicago experience.Neurosurgery. 1998 Dec;43(6):1281-95; discussion 1296-7. doi: 10.1097/00006123-199812000-00011. Neurosurgery. 1998. PMID: 9848841 Review.
Cited by
-
"Waffle cone"technique for intra/extra-aneurysmal stent placement for the treatment of complex and wide-necked bifurcation aneurysm.Interv Neuroradiol. 2008 Nov 11;14 Suppl 2(Suppl 2):49-52. doi: 10.1177/15910199080140S210. Epub 2009 Jan 2. Interv Neuroradiol. 2008. PMID: 20557801 Free PMC article.
-
Clinical safety and efficacy of stent-assisted coil embolization with ACCERO stent in cerebral aneurysm: Short-term follow-up and precaution for use.J Cerebrovasc Endovasc Neurosurg. 2025 Jun;27(2):118-128. doi: 10.7461/jcen.2025.E2025.02.002. Epub 2025 Feb 24. J Cerebrovasc Endovasc Neurosurg. 2025. PMID: 39988324 Free PMC article.
-
Neqstent coil-assisted flow diverter (NQS) for the treatment of bifurcation aneurysms: the coil-assisted flow diversion safety and performance study (CAFI).J Neurointerv Surg. 2024 Jun 17;16(7):721-725. doi: 10.1136/jnis-2022-020056. J Neurointerv Surg. 2024. PMID: 37419693 Free PMC article. Clinical Trial.
-
pCONus Device for the Endovascular Treatment of Wide-Neck Middle Cerebral Artery Aneurysms.AJNR Am J Neuroradiol. 2015 Sep;36(9):1735-40. doi: 10.3174/ajnr.A4392. Epub 2015 Jul 23. AJNR Am J Neuroradiol. 2015. PMID: 26206810 Free PMC article.
-
Waffle-cone technique with Solitaire™ AB remodeling device: endovascular treatment of highly selected complex cerebral aneurysms.Neuroradiology. 2011 Dec;53(12):961-72. doi: 10.1007/s00234-010-0766-6. Epub 2010 Sep 7. Neuroradiology. 2011. PMID: 20821314
References
-
- Molyneux A, Kerr R, Stratton I, et al. International Subarachnoid Aneurysm Trial (ISAT) of neurosurgical clipping versus endovascular coiling in 2143 patients with ruptured intracranial aneurysms: a randomised trial. Lancet 2002;360:1267–74 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
