Relevance of anaesthesia for dofetilide-induced torsades de pointes in alpha1-adrenoceptor-stimulated rabbits
- PMID: 17965737
- PMCID: PMC2199389
- DOI: 10.1038/sj.bjp.0707536
Relevance of anaesthesia for dofetilide-induced torsades de pointes in alpha1-adrenoceptor-stimulated rabbits
Abstract
Background and purpose: No information is available concerning the effects of anaesthetics in the most frequently used in vivo pro-arrhythmia model. Accordingly, in this study we examined the effect of pentobarbital, propofol or alpha-chloralose anaesthesia on the pro-arrhythmic activity of the class III anti-arrhythmic dofetilide in alpha(1)-adrenoceptor-stimulated rabbits.
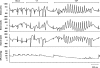
Experimental approach: Rabbits anaesthetized intravenously with pentobarbital, propofol or alpha-chloralose were infused simultaneously with the alpha(1)-adrenoceptor agonist phenylephrine (15 microg kg(-1) min(-1), i.v.) and dofetilide (0.04 mg kg(-1) min(-1), i.v.). The electrocardiographic QT interval, the T (peak)-T (end) interval and certain QT variability parameters were measured. The heart rate variability and the baroreflex sensitivity were utilized to assess the vagal nerve activity. The spectral power of the systolic arterial pressure was calculated in the frequency range 0.15-0.5 Hz to assess the sympathetic activity.
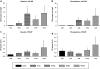
Key results: Pentobarbital considerably reduced, whereas propofol did not significantly affect the incidence of dofetilide-induced torsades de pointes (TdP) as compared with the results with alpha-chloralose (40% (P=0.011) and 70% (P=0.211) vs 100%, respectively). In additional experiments, neither doubling of the rate of the dofetilide infusion nor tripling of the rate of phenylephrine infusion elevated the incidence of TdP to the level seen with alpha-chloralose. None of the repolarization-related parameters predicted TdP. The indices of the parasympathetic and sympathetic activity were significantly depressed in the alpha-chloralose and propofol anaesthesia groups.
Conclusions and implications: In rabbits, anaesthetics may affect drug-induced TdP genesis differently, which must be considered when results of different studies are compared.
Figures

Similar articles
-
Biomarkers and endogenous determinants of dofetilide-induced torsades de pointes in α(1) -adrenoceptor-stimulated, anaesthetized rabbits.Br J Pharmacol. 2010 Dec;161(7):1477-95. doi: 10.1111/j.1476-5381.2010.00965.x. Br J Pharmacol. 2010. PMID: 20659107 Free PMC article.
-
Importance of extracardiac alpha1-adrenoceptor stimulation in assisting dofetilide to induce torsade de pointes in rabbit hearts.Eur J Pharmacol. 2006 May 10;537(1-3):118-25. doi: 10.1016/j.ejphar.2006.03.014. Epub 2006 Mar 20. Eur J Pharmacol. 2006. PMID: 16618484
-
The role of the Na+/Ca2+ exchanger, I(Na) and I(CaL) in the genesis of dofetilide-induced torsades de pointes in isolated, AV-blocked rabbit hearts.Br J Pharmacol. 2009 Mar;156(6):920-32. doi: 10.1111/j.1476-5381.2008.00096.x. Epub 2009 Feb 16. Br J Pharmacol. 2009. PMID: 19222480 Free PMC article.
-
Dofetilide induced torsade de pointes: mechanism, risk factors and management strategies.Indian Heart J. 2014 Nov-Dec;66(6):640-8. doi: 10.1016/j.ihj.2013.12.021. Epub 2014 Jan 7. Indian Heart J. 2014. PMID: 25634399 Free PMC article. Review.
-
Role of transmural dispersion of repolarization in the genesis of drug-induced torsades de pointes.Heart Rhythm. 2005 Nov;2(2 Suppl):S9-15. doi: 10.1016/j.hrthm.2004.09.011. Heart Rhythm. 2005. PMID: 16253930 Free PMC article. Review.
Cited by
-
Importance of vagally mediated bradycardia for the induction of torsade de pointes in an in vivo model.Br J Pharmacol. 2008 Jul;154(5):958-70. doi: 10.1038/bjp.2008.154. Epub 2008 Apr 21. Br J Pharmacol. 2008. PMID: 18587444 Free PMC article.
-
Adrenaline reveals the torsadogenic effect of combined blockade of potassium channels in anaesthetized guinea pigs.Br J Pharmacol. 2008 Aug;154(7):1414-26. doi: 10.1038/bjp.2008.169. Epub 2008 May 19. Br J Pharmacol. 2008. PMID: 18493252 Free PMC article.
-
Absolute beat-to-beat variability and instability parameters of ECG intervals: biomarkers for predicting ischaemia-induced ventricular fibrillation.Br J Pharmacol. 2014 Apr;171(7):1772-82. doi: 10.1111/bph.12579. Br J Pharmacol. 2014. PMID: 24417376 Free PMC article.
-
Drug-induced proarrhythmia: risk factors and electrophysiological mechanisms.Nat Rev Cardiol. 2016 Jan;13(1):36-47. doi: 10.1038/nrcardio.2015.110. Epub 2015 Jul 21. Nat Rev Cardiol. 2016. PMID: 26194552 Review.
-
Assessment of proarrhythmic activity of chloroquine in in vivo and ex vivo rabbit models.J Pharmacol Pharmacother. 2013 Apr;4(2):116-24. doi: 10.4103/0976-500X.110892. J Pharmacol Pharmacother. 2013. PMID: 23759957 Free PMC article.
References
-
- Aeschbacher G, Webb AI. Propofol in rabbits. 1. Determination of an induction dose. Lab Anim Sci. 1993a;43:324–327. - PubMed
-
- Aeschbacher G, Webb AI. Propofol in rabbits. 2. Long-term anesthesia. Lab Anim Sci. 1993b;43:328–335. - PubMed
-
- Antzelevitch C, Shimizu W, Yan GX, Sicouri S, Weissenburger J, Nesterenko VV, et al. The M cell: its contribution to the ECG and to normal and abnormal electrical function of the heart. J Cardiovasc Electrophysiol. 1999;10:1124–1152. - PubMed
-
- Bachmann A, Mueller S, Kopp K, Brueggemann A, Suessbrich H, Gerlach U, et al. Inhibition of cardiac potassium currents by pentobarbital. Naunyn Schmiedebergs Arch Pharmacol. 2002;365:29–37. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Miscellaneous

