Occlusion length is a crucial determinant of efficiency and complication rate in thrombectomy for acute ischemic stroke
- PMID: 17974616
- PMCID: PMC8119001
- DOI: 10.3174/ajnr.A0790
Occlusion length is a crucial determinant of efficiency and complication rate in thrombectomy for acute ischemic stroke
Abstract
Background and purpose: Although mechanical thrombectomy (MT) has an encouragingly high recanalization rate in treating stroke, it is associated with severe complications of which the underlying factors have yet to be identified. Because MT is a mechanical approach, the mechanical properties of the thrombus might be crucial for its success. The present study assesses the effect of thrombus length on the in vivo effectiveness and complication rate of MT.
Materials and methods: Angiography and embolization of 21 cranial vessels with radiopaque whole-blood thrombi 10, 20, and 40 mm in length (7 occlusions each) were performed in 7 swine. MT was carried out using a distal snarelike device (BCR Roadsaver) with proximal balloon occlusion. A total of 61 retrievals were attempted.
Results: In the group of 10-mm occlusions, 77.8% of the attempts achieved complete recanalisation. For longer occlusions, the success rates decreased significantly to 20% of attempts for 20-mm occlusions (odds ratio [OR], 14; 95% confidence interval [CI], 2.2-89.2) and 11.1% for 40-mm occlusions (OR, 28; 95% CI, 3.9-202.2; P < .005). The low success rates were largely due to complications associated with thrombus compaction during retrieval. Similarly, the rate of thromboembolic events increased from 0% in 10-mm occlusions to 14.8% in 40-mm occlusions.
Conclusions: MT using a distal device proved to be a fast, effective, and safe procedure for recanalizing short (10-mm) occlusions in the animal model. However, occlusion length emerged as a crucial determinant for MT with a significant decrease in recanalization success per attempt and increased complication rates. These findings suggest limitations of MT in the clinical application.
Figures


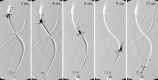



References
-
- del Zoppo GJ, Higashida RT, Furlan AJ, et al. PROACT: a phase II randomized trial of recombinant pro-urokinase by direct arterial delivery in acute middle cerebral artery stroke. PROACT Investigators. Prolyse in Acute Cerebral Thromboembolism. Stroke 1998;29:4–11 - PubMed
-
- Arnold M, Schroth G, Nedeltchev K, et al. Intra-arterial thrombolysis in 100 patients with acute stroke due to middle cerebral artery occlusion. Stroke 2002;33:1828–33 - PubMed
-
- The National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group. Tissue plasminogen activator for acute ischemic stroke. N Engl J Med 1995;333:1581–87 - PubMed
-
- Furlan A, Higashida R, Wechsler L, et al. Intra-arterial prourokinase for acute ischemic stroke. The PROACT II study: a randomized controlled trial. Prolyse in Acute Cerebral Thromboembolism. JAMA 1999;282:2003–11 - PubMed
-
- Layton KF, White JB, Cloft HJ, et al. Expanding the treatment window with mechanical thrombectomy in acute ischemic stroke. Neuroradiology 2006;48:402–04 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
