Biomarkers of hepatic fibrosis, fibrogenesis and genetic pre-disposition pending between fiction and reality
- PMID: 17979881
- PMCID: PMC4401271
- DOI: 10.1111/j.1582-4934.2007.00092.x
Biomarkers of hepatic fibrosis, fibrogenesis and genetic pre-disposition pending between fiction and reality
Abstract
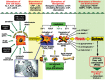
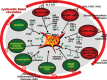
Fibrosis is a frequent, life-threatening complication of most chronic liver diseases. Despite major achievements in the understanding of its pathogenesis, the translation of this knowledge into clinical practice is still limited. In particular, non-invasive and reliable (serum-) biomarkers indicating the activity of fibrogenesis are scarce. Class I biomarkers are defined as serum components having a direct relation to the mechanism of fibrogenesis, either as secreted matrix-related components of activated hepatic stellate cells and fibroblasts or as mediators of extracellular matrix (ECM) synthesis or turnover. They reflect primarily the activity of the fibrogenic process. Many of them, however, proved to be disappointing with regard to sensitivity and specificity. Up to now hyaluronan turned out to be the relative best type I serum marker. Class II biomarkers comprise in general rather simple standard laboratory tests, which are grouped into panels. They fulfil most criteria for detection and staging of fibrosis and to a lesser extent grading of fibrogenic activity. More than 20 scores are currently available, among which Fibrotest is the most popular one. However, the diagnostic use of many of these scores is still limited and standardization of the assays is only partially realized. Combining of panel markers in sequential algorithms might increase their diagnostic validity. The translation of genetic pre-disposition biomarkers into clinical practice has not yet started, but some polymorphisms indicate a link to progression and outcome of fibrogenesis. Parallel to serum markers non-invasive physical techniques, for example, transient elastography, are developed, which can be combined with serum tests and profiling of serum proteins and glycans.
Figures


Similar articles
-
Biomarkers of liver fibrosis: clinical translation of molecular pathogenesis or based on liver-dependent malfunction tests.Clin Chim Acta. 2007 Jun;381(2):107-13. doi: 10.1016/j.cca.2007.02.038. Epub 2007 Feb 27. Clin Chim Acta. 2007. PMID: 17399697 Review.
-
Non-invasive biomarkers for monitoring the fibrogenic process in liver: a short survey.World J Gastroenterol. 2009 May 28;15(20):2433-40. doi: 10.3748/wjg.15.2433. World J Gastroenterol. 2009. PMID: 19468990 Free PMC article.
-
Biochemical markers, extracellular components in liver fibrosis and cirrhosis.Nig Q J Hosp Med. 2007 Jan-Mar;17(1):42-52. doi: 10.4314/nqjhm.v17i1.12541. Nig Q J Hosp Med. 2007. PMID: 17688172 Review.
-
Non-invasive markers for hepatic fibrosis.BMC Gastroenterol. 2011 Aug 17;11:91. doi: 10.1186/1471-230X-11-91. BMC Gastroenterol. 2011. PMID: 21849046 Free PMC article. Review.
-
Proteomics and liver fibrosis: identifying markers of fibrogenesis.Expert Rev Proteomics. 2009 Aug;6(4):421-31. doi: 10.1586/epr.09.59. Expert Rev Proteomics. 2009. PMID: 19681677 Review.
Cited by
-
Hyaluronic Acid in Vascular and Immune Homeostasis during Normal Pregnancy and Preeclampsia.Acta Naturae. 2016 Jul-Sep;8(3):59-71. Acta Naturae. 2016. PMID: 27795844 Free PMC article.
-
Caffeine intake decreases oxidative stress and inflammatory biomarkers in experimental liver diseases induced by thioacetamide: Biochemical and histological study.Int J Immunopathol Pharmacol. 2017 Mar;30(1):13-24. doi: 10.1177/0394632017694898. Epub 2017 Feb 1. Int J Immunopathol Pharmacol. 2017. PMID: 28281876 Free PMC article.
-
Extracellular matrix remodeling: the common denominator in connective tissue diseases. Possibilities for evaluation and current understanding of the matrix as more than a passive architecture, but a key player in tissue failure.Assay Drug Dev Technol. 2013 Mar;11(2):70-92. doi: 10.1089/adt.2012.474. Epub 2012 Oct 9. Assay Drug Dev Technol. 2013. PMID: 23046407 Free PMC article. Review.
-
Non-invasive evaluation of liver stiffness after splenectomy in rabbits with CCl4-induced liver fibrosis.World J Gastroenterol. 2016 Dec 14;22(46):10166-10179. doi: 10.3748/wjg.v22.i46.10166. World J Gastroenterol. 2016. PMID: 28028365 Free PMC article.
-
The human hyaluronan synthase 2 (HAS2) gene and its natural antisense RNA exhibit coordinated expression in the renal proximal tubular epithelial cell.J Biol Chem. 2011 Jun 3;286(22):19523-32. doi: 10.1074/jbc.M111.233916. Epub 2011 Feb 25. J Biol Chem. 2011. PMID: 21357421 Free PMC article.
References
-
- Pinzani M, Rombouts K. Liver fibrosis: from the bench to clinical targets. Digest Liver Dis. 2004;36:231–42. - PubMed
-
- Friedman SL, Rockey DC, Bissell DM. Hepatic fibrosis 2006: Report of the third AASLD Single Topic Conference. Hepatology. 2007;45:242–9. - PubMed
-
- Bedossa P, Dargere D, Paradis V. Sampling variability of liver fibrosis in chronic hepatitis C. Hepatology. 2003;38:1449–57. - PubMed
-
- Afdhal NH, Nunes D. Evaluation of Liver Fibrosis: A Concise Review. Am J Gastroenterol. 2004;99:1160–74. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

