Mortality and physician supply: does region hold the key to the paradox?
- PMID: 17995563
- PMCID: PMC2151400
- DOI: 10.1111/j.1475-6773.2007.00728.x
Mortality and physician supply: does region hold the key to the paradox?
Abstract
Objective: . To determine if the supply of physicians has a consistent relationship with mortality across regions.
Data sources: County-level data describing the supply of physicians, mortality, and socioeconomic conditions of the population as provided in the Area Resource File (BHPr, HRSA) and the Compressed Mortality File (NCHS, CDC).
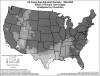
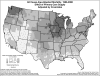
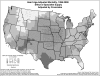
Study design: Ordinary least squares and geographically weighted regression models with age-adjusted all-cause and disease-specific mortality as the dependent variables were specified using pooled data from 1996 to 2000 to test for the relationship with primary care and specialist physician-population ratios. The residuals from the OLS models were mapped and examined for potential clustering. A series of geographically weighted regression models were run for all 3,070 counties and the z-scores and significance of the models mapped.
Principal findings: The association between primary care physician supply and mortality was not observed in contrast to other studies; mapping the residuals of those models suggested regional clustering. When weighted geographically, the relationship between primary care and specialist physician supply and mortality presents a mixed pattern. The results show strong regional patterns that may explain the lack of a consistent national association. Primary care physicians are associated with decreased mortality on the east coast and upper midwest, but that correlation disappears or is reversed in the west (with the exception of Washington State) and south central states.
Conclusions: We find evidence that there are regionally focused association between physician supply and mortality, holding constant population characteristics that reflect the influence of social and economic characteristics. However, these relationships are not consistent across the United States; there are regions where there are stronger and weaker associations between type of practitioner and mortality and other regions where no association is apparent. This suggests that the direction for further analysis lies in the understanding of the regional differences and whether there are policy alternatives to address these different patterns.
Figures
Comment in
-
Commentary: primary care and health outcomes: a health services research challenge.Health Serv Res. 2007 Dec;42(6 Pt 1):2252-6; discussion 2294-323. doi: 10.1111/j.1475-6773.2007.00739.x. Health Serv Res. 2007. PMID: 17995564 Free PMC article. No abstract available.
References
-
- Bureau of Health Professions. Area Resource Files. Rockville, MD: Health Resources and Services Administration; 2002.
-
- Cooper RA, Henderson T, Dietrich CL. “Roles of Nonphysician Clinicians as Autonomous Providers of Patient Care.”. Journal of the American Medical Association. 1998;280(9):795–802. - PubMed
-
- Cossman RE, Cossman JS, Jackson R, Cosby A. “Mapping High or Low Mortality Places across Time in the United States: A Research Note on a Health Visualization and Analysis Project.”. Health Place. 2003;9(4):361–9. - PubMed
-
- Fisher ES, Wennberg JE. “Health Care Quality, Geographic Variations, and the Challenge of Supply-Sensitive Care.”. Perspectives in Biology and Medicine. 2003;46(1):69–79. - PubMed
-
- Forrest CB, Starfield B. “The Effect of First-Contact Care with Primary Care Clinicians on Ambulatory Health Care Expenditures.”. Journal of Family Practice. 1996;43:40–8. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

