Congenital cholestatic syndromes: what happens when children grow up?
- PMID: 18026579
- PMCID: PMC2658590
- DOI: 10.1155/2007/581247
Congenital cholestatic syndromes: what happens when children grow up?
Abstract
Although advances in the management of children with congenital cholestasis have enabled many to survive into adulthood with their native livers, even the most common of these conditions remains rare in adult hepatology practice. Among four congenital cholestatic syndromes (biliary atresia, Alagille syndrome, Caroli disease and congenital hepatic fibrosis, and progressive familial intrahepatic cholestasis), the published data on outcomes of the syndromes into adulthood suggest that a spectrum of severity of liver disease can be expected, from cirrhosis (almost universal in adults with biliary atresia who have not required liver transplantation) to mild and subclinical (eg, in the previously undiagnosed affected parent of an infant with Alagille syndrome). Complications associated with portal hypertension and nutritional deficiencies are common, and other associated features of the cholestatic syndrome may require appropriate attention, such as congenital heart disease in Alagille syndrome. Indications for liver transplantation include synthetic failure, progressive encephalopathy, intractable pruritus, recurrent biliary sepsis and recurrent complications of portal hypertension. Improved understanding of biliary physiology will hopefully translate into improved therapy for children and adults with cholestasis.
Bien que les progrès dans la prise en charge des enfants atteints d’une cholestase congénitale aient permis à bon nombre d’entre eux de survivre jusqu’à l’âge adulte avec leur foie d’origine, ces pathologies, même les plus courantes, demeurent rares en hépathologie pour adultes. Parmi les quatre syndromes cholostatiques congénitaux (atrésie des voies biliaires, syndrome d’alagille, maladie de Caroli et fibrose hépatique congéniale, cholestase intrahépatique héréditaire évolutive), les données publiées sur l’issue des syndromes à l’âge adulte laissent prévoir tout un spectre de gravité de maladie hépatique, en passant par la cirrhose (presque universelle chez les adultes atteints d’atrésie des voies biliaires qui n’ont pas subi de greffe hépatique) jusqu’à une maladie légère et subclinique (p. ex., chez le parent auparavant non diagnostiqué d’un nourrisson atteint du syndrome d’alagille). Les complications associées à l’hypertension portale et aux déficiences nutritionnelles sont courantes, et d’autres caractéristiques reliées au syndrome cholostatique peuvent exiger des mesures pertinentes, telles que la cardiopathie congénitale en cas de syndrome d’alagille. Les indications de greffe hépatique incluent une faille synthétique, une encéphalopathie évolutive, un prurit réfractaire, une septicémie biliaire récurrente et les complications récurrentes de l’hypertension portale. Les auteurs espèrent qu’une meilleure compréhension de la physiologie biliaire se traduira par une amélioration de la thérapie des enfants et des adultes atteints de cholestase biliaire.
Figures
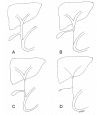

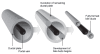

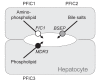
References
-
- Moyer V, Freese DK, Whitington PF, et al. Guideline for the evaluation of cholestatic jaundice in infants: Recommendations of the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition. J Pediatr Gastroenterol Nutr. 2004;39:115–28. (Erratum in 2004;39:306). - PubMed
-
- Mack CL, Sokol RJ. Unraveling the pathogenesis and etiology of biliary atresia. Pediatr Res. 2005;57:87R–94R. - PubMed
-
- Zhang DY, Sabla G, Shivakumar P, et al. Coordinate expression of regulatory genes differentiates embryonic and perinatal forms of biliary atresia. Hepatology. 2004;39:954–62. - PubMed
-
- Davenport M. A challenge on the use of the words embryonic and perinatal in the context of biliary atresia. Hepatology. 2005;41:403–4. - PubMed
-
- Muise AM, Turner D, Wine E, Kim P, Marcon M, Ling SC. Biliary atresia with choledochal cyst: Implications for classification. Clin Gastroenterol Hepatol. 2006;4:1411–4. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
