The relationship between nighttime dipping in blood pressure and cerebral hemodynamics in nonstroke patients
- PMID: 18046099
- PMCID: PMC8110050
- DOI: 10.1111/j.1524-6175.2007.07342.x
The relationship between nighttime dipping in blood pressure and cerebral hemodynamics in nonstroke patients
Abstract
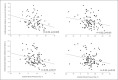
Inadequate dipping in nighttime blood pressure (BP) is associated with cerebrovascular disease. The authors aimed to determine whether inadequate nocturnal dipping was associated with abnormalities in cerebrovascular hemodynamics in individuals without stroke. Participants in this study underwent 24-hour ambulatory BP monitoring followed by morning transcranial Doppler measurements of blood flow velocities (BFVs) in the middle cerebral artery during supine rest, head-up tilt, hypocapnia, and hypercapnia. Nighttime BP decline by <10% was considered nondipping. Of the 102 nonstroke participants (mean age, 53.6 years), 35 (34%) were dippers. Although nondippers had similar BFV and cerebrovascular resistance (CVR) while supine, they had a lower BFV (P=.04) and greater CVR (P=.02) during head-up tilt compared with dippers. Moreover, greater nighttime dipping in both systolic BP (P=.006) and diastolic BP (P=.03) were associated with higher daytime BFV and lower CVR (P=.01 for systolic BP; P=.02 for diastolic BP). Inadequate nocturnal BP dipping is associated with lower daytime cerebral blood flow, especially during head-up tilt.
Figures

References
-
- Giles TD. Circadian rhythm of blood pressure and the relation to cardiovascular events. J Hypertens Suppl. 2006;24(2):S11–S16. - PubMed
-
- Tsioufis C, Antoniadis D, Stefanadis C, et al. Relationships between new risk factors and circadian blood pressure variation in untreated subjects with essential hypertension. Am J Hypertens. 2002;15(7, pt 1):600–604. - PubMed
-
- Lee AC, Rahman S, Hodges JR, et al. Associative and recognition memory for novel objects in dementia: implications for diagnosis. Eur J Neurosci. 2003;18(6):1660–1670. - PubMed
-
- Fujiwara N, Osanai T, Baba Y, et al. Nocturnal blood pressure decrease is associated with increased regional cerebral blood flow in patients with a history of ischemic stroke. J Hypertens. 2005;23(5):1055–1060. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

