MRI in ocular drug delivery
- PMID: 18186077
- PMCID: PMC2728085
- DOI: 10.1002/nbm.1230
MRI in ocular drug delivery
Abstract
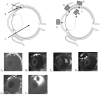
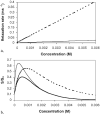
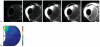
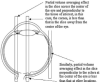
Conventional pharmacokinetic methods for studying ocular drug delivery are invasive and cannot be conveniently applied to humans. The advancement of MRI technology has provided new opportunities in ocular drug-delivery research. MRI provides a means to non-invasively and continuously monitor ocular drug-delivery systems with a contrast agent or compound labeled with a contrast agent. It is a useful technique in pharmacokinetic studies, evaluation of drug-delivery methods, and drug-delivery device testing. Although the current status of the technology presents some major challenges to pharmaceutical research using MRI, it has a lot of potential. In the past decade, MRI has been used to examine ocular drug delivery via the subconjunctival route, intravitreal injection, intrascleral injection to the suprachoroidal space, episcleral and intravitreal implants, periocular injections, and ocular iontophoresis. In this review, the advantages and limitations of MRI in the study of ocular drug delivery are discussed. Different MR contrast agents and MRI techniques for ocular drug-delivery research are compared. Ocular drug-delivery studies using MRI are reviewed.
Figures

Similar articles
-
Episcleral, intrascleral, and suprachoroidal routes of ocular drug delivery - recent research advances and patents.Recent Pat Drug Deliv Formul. 2014;8(2):81-91. doi: 10.2174/187221130802140707093509. Recent Pat Drug Deliv Formul. 2014. PMID: 25001638 Review.
-
Assessment of subconjunctival and intrascleral drug delivery to the posterior segment using dynamic contrast-enhanced magnetic resonance imaging.Invest Ophthalmol Vis Sci. 2007 Feb;48(2):808-14. doi: 10.1167/iovs.06-0670. Invest Ophthalmol Vis Sci. 2007. PMID: 17251481
-
Controlled drug release from an ocular implant: an evaluation using dynamic three-dimensional magnetic resonance imaging.Invest Ophthalmol Vis Sci. 2004 Aug;45(8):2722-31. doi: 10.1167/iovs.04-0091. Invest Ophthalmol Vis Sci. 2004. PMID: 15277497
-
MRI study of subconjunctival and intravitreal injections.J Pharm Sci. 2012 Jul;101(7):2353-63. doi: 10.1002/jps.23127. Epub 2012 Mar 30. J Pharm Sci. 2012. PMID: 22473517 Free PMC article.
-
Safety evaluation of ocular drug delivery formulations: techniques and practical considerations.Toxicol Pathol. 2008 Jan;36(1):49-62. doi: 10.1177/0192623307310955. Toxicol Pathol. 2008. PMID: 18337221 Review.
Cited by
-
Ultrahigh field MR imaging of a subconjunctival anti-glaucoma drug delivery system in a rabbit model.Sci Rep. 2017 Nov 17;7(1):15780. doi: 10.1038/s41598-017-15954-w. Sci Rep. 2017. PMID: 29150670 Free PMC article.
-
Monitoring New Long-Lasting Intravitreal Formulation for Glaucoma with Vitreous Images Using Optical Coherence Tomography.Pharmaceutics. 2021 Feb 5;13(2):217. doi: 10.3390/pharmaceutics13020217. Pharmaceutics. 2021. PMID: 33562488 Free PMC article.
-
Ocular pharmacokinetic study using T₁ mapping and Gd-chelate- labeled polymers.Pharm Res. 2011 Dec;28(12):3180-8. doi: 10.1007/s11095-011-0507-5. Epub 2011 Jun 21. Pharm Res. 2011. PMID: 21691891 Free PMC article.
-
Review: magnetic resonance imaging techniques in ophthalmology.Mol Vis. 2012;18:2538-60. Epub 2012 Oct 12. Mol Vis. 2012. PMID: 23112569 Free PMC article. Review.
-
Medical Imaging Technology and Imaging Agents.Adv Exp Med Biol. 2023;1199:15-38. doi: 10.1007/978-981-32-9902-3_2. Adv Exp Med Biol. 2023. PMID: 37460725
References
-
- Bauer NJ, Motamedi M, Wicksted JP, March WF, Webers CA, Hendrikse F. Non-invasive assessment of ocular pharmacokinetics using Confocal Raman Spectroscopy. J. Ocul. Pharmacol. Ther. 1999;15:123–134. - PubMed
-
- Szymanski-Exner A, Stowe NT, Salem K, Lazebnik R, Haaga JR, Wilson DL, Gao J. Noninvasive monitoring of local drug release using X-ray computed tomography: optimization and in vitro/in vivo validation. J. Pharm. Sci. 2003;92:289–296. - PubMed
-
- Mader K, Bacic G, Domb A, Elmalak O, Langer R, Swartz HM. Noninvasive in vivo monitoring of drug release and polymer erosion from biodegradable polymers by EPR spectroscopy and NMR imaging. J. Pharm. Sci. 1997;86:126–134. - PubMed
-
- Rudin M, Weissleder R. Molecular imaging in drug discovery and development. Nat. Rev. Drug Discov. 2003;2:123–131. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

