Outcomes of revascularization strategies for two-vessel coronary artery disease involving the proximal left anterior descending artery in an era of improved pharmacotherapy and stenting
- PMID: 18273485
- PMCID: PMC2644566
- DOI: 10.1016/s0828-282x(08)70567-1
Outcomes of revascularization strategies for two-vessel coronary artery disease involving the proximal left anterior descending artery in an era of improved pharmacotherapy and stenting
Abstract
Background: The best therapeutic strategy for patients with double-vessel coronary artery disease and proximal left anterior descending artery involvement (2VD + pLAD) is not clear.
Objectives: To compare the survival experience of a cohort of cardiac catheterization patients with 2VD + pLAD based on chosen therapeutic strategy (medical management versus percutaneous coronary intervention [PCI] versus coronary artery bypass graft surgery [CABG]).
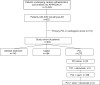
Methods: The authors identified and studied a total of 603 patients with 2VD + pLAD from all patients who underwent diagnostic coronary angiography in Alberta between January 1997 and May 1999. The primary end point was five-year survival from index catheterization for each of the treatment groups and from time of revascularization when the two revascularization strategies were compared.
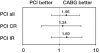
Results: Risk-adjusted hazard ratios (HR) comparing cumulative five-year survival rates of patients treated medically, or with PCI or CABG indicated a survival benefit for patients treated with CABG (HR 0.24, 95% CI 0.11 to 0.54; P<0.001) and PCI (HR 0.43, 95% CI 0.24 to 0.77; P=0.003) compared with medical management. Meanwhile, a risk-adjusted comparison of revascularization strategies suggested a possible trend toward higher mortality for PCI-treated patients versus CABG-treated patients (HR 1.56, 95% CI 0.65 to 3.72; P=0.125).
Conclusions: The results of this registry-based observational study suggest a survival benefit from revascularization compared with medical management in patients with 2VD + pLAD. Furthermore, the authors found a trend toward better survival in CABG-treated patients compared with PCI-treated patients.
HISTORIQUE: On n’est pas certain de la meilleure stratégie thérapeutique pour les patients atteints d’une coronaropathie bitronculaire avec atteinte de l’artère descendante antérieure gauche proximale (C2T+DAGP).
OBJECTIFS: Comparer l’expérience de survie d’une cohorte de patients ayant subi un cathétérisme cardiaque avec C2T+DAGP d’après la stratégie thérapeutique choisie (prise en charge médicale, intervention coronaire percutanée [ICP] ou pontage aortocoronarien [PAC]).
MÉTHODOLOGIE: Les auteurs ont dépisté et étudié un total de 603 patients atteints d’une C2T+DAGP parmi l’ensemble des patients qui avaient subi une coronarographie diagnostique en Alberta entre janvier 1997 et mai 1999. Le paramètre ultime primaire était la survie cinq ans après le cathétérisme de référence dans chacun des groupes de traitement et à compter de la revascularisation lorsqu’on comparait les deux stratégies de revascularisation.
RÉSULTATS: Les risques relatifs rajustés (RRR) comparant les taux de survie au bout de cinq ans des patients traités par des médicaments, par ICP ou par PAC indiquent un avantage de survie chez les patients traités par PAC (RRR 0,24, 95 % IC 0,11 à 0,54; P<0,001) et par ICP (RRR 0,43, 95% IC 0,24 à 0,77; P=0,003) par rapport à la prise en charge médicale. De plus, une comparaison rajustée au risque des stratégies de revascularisation laisse supposer une tendance possible vers un taux de mortalité plus élevé chez les patients traités par ICP par rapport à ceux traités par PAC (RRR 1,56, 95 % IC 0,65 à 3,72; P=0,125).
CONCLUSIONS: Les résultats de cette étude d’observation de dossiers laissent supposer une meilleure survie après la revascularisation qu’à la prise en charge médicale chez les patients atteints d’une C2T+DAGP. De plus, les auteurs ont remarqué une tendance de meilleure survie chez les patients ayant subi une PAC par rapport à ceux traités par ICP.
Figures




References
-
- Hartigan PM, Giacomini JC, Folland ED, Parisi AF. Two- to three-year follow-up of patients with single-vessel coronary artery disease randomized to PTCA or medical therapy (results of a VA cooperative study). Veterans Affairs Cooperative Studies Program ACME Investigators. Angioplasty Compared to Medicine. Am J Caridol. 1998;82:1445–50. - PubMed
-
- RITA-2 trial participants. Coronary angioplasty versus medical therapy for angina: The second Randomised Intervention Treatment of Angina (RITA-2) trial. Lancet. 1997;350:461–8. - PubMed
-
- Pitt B, Waters D, Brown WV, et al. Aggressive lipid-lowering therapy compared with angioplasty in stable coronary artery disease. Atorvastatin versus Revascularization Treatment Investigators. N Engl J Med. 1999;341:70–6. - PubMed
-
- Gibbons RJ, Abrams J, Chatterjee K, et al. American College of Cardiology; American Heart Association Task Force on Practice Guidelines. Committee on the Management of Patients With Chronic Stable Angina. ACC/AHA 2002 guideline update for the management of patients with chronic stable angina – summary article: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on the Management of Patients With Chronic Stable Angina) Circulation. 2003;107:149–58. - PubMed
-
- Coronary angioplasty versus coronary artery bypass surgery: The Randomized Intervention Treatment of Angina (RITA) trial. Lancet. 1993;341:573–80. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

