Passive versus active parental permission: implications for the ability of school-based depression screening to reach youth at risk
- PMID: 18307611
- PMCID: PMC2713664
- DOI: 10.1111/j.1746-1561.2007.00278.x
Passive versus active parental permission: implications for the ability of school-based depression screening to reach youth at risk
Abstract
Background: Depression is prevalent among children and adolescents and often goes untreated with adverse effects on academic success and healthy development. Depression screening can facilitate early identification and timely referral to prevention and treatment programs. Conducting school-based emotional health screening, however, raises the controversial issue of how to obtain informed parental permission.
Methods: During implementation of a depression screening program in an urban school district in the Pacific Northwest, the district's parental permission protocol changed from passive (information provided to parents via a school mailer with parents having the option to actively decline their child's participation) to active (information provided to parents via a school mailer requiring the written permission of the parents for their child's participation). This change provided an opportunity to examine differences in participation under these 2 conditions.
Results: A total of 1533 students were enrolled in this program across both years. Compared to conditions of passive permission, participation was dramatically reduced when children were required to have written parental permission, dropping from 85% to 66% of eligible children. Furthermore, under conditions of active parental permission, participation decreased differentially among student subgroups with increased risk for depression.
Conclusions: Successful implementation of school-based emotional health screening programs requires careful consideration of how to inform and obtain permission from parents.
Figures
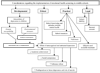

References
-
- Lewinsohn PM, Hops H, Roberts RE, Seeley JR, Andrews JA. Adolescent psychopathology: I. Prevalence and incidence of depression and other DSM-III-R disorders in high school students. J Abnorm Psychol. 1993;102(1):133–144. - PubMed
-
- Birmaher B, Ryan ND, Williamson DE, Brent DA, Kaufman J, Dahl RE, et al. Childhood and adolescent depression: a review of the past 10 years. Part I. J Am Acad Child Adolesc Psychiatry. 1996;35(11):1427–1439. - PubMed
-
- Vander Stoep A, Weiss NS, Kuo ES, Cheney D, Cohen P. What proportion of failure to complete secondary school in the US population is attributable to adolescent psychiatric disorder? J Behav Health Serv Res. 2003;30(1):119–124. - PubMed
-
- Wu P, Hoven CW, Bird HR, Moore RE, Cohen P, Alegria M, et al. Depressive and disruptive disorders and mental health service utilization in children and adolescents. J Am Acad Child Adolesc Psychiatry. 1999;38(9):1081–1090. discussion 1090–2. - PubMed
-
- Angold A, Costello EJ, Farmer EM, Burns BJ, Erkanli A. Impaired but undiagnosed. J Am Acad Child Adolesc Psychiatry. 1999;38(2):129–137. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

