Alterations in vasomotor control of coronary resistance vessels in remodelled myocardium of swine with a recent myocardial infarction
- PMID: 18320249
- PMCID: PMC2329737
- DOI: 10.1007/s11517-008-0315-1
Alterations in vasomotor control of coronary resistance vessels in remodelled myocardium of swine with a recent myocardial infarction
Abstract
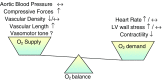
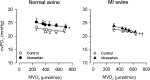
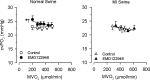
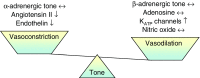
The mechanism underlying the progressive deterioration of left ventricular (LV) dysfunction after myocardial infarction (MI) towards overt heart failure remains incompletely understood, but may involve impairments in coronary blood flow regulation within remodelled myocardium leading to intermittent myocardial ischemia. Blood flow to the remodelled myocardium is hampered as the coronary vasculature does not grow commensurate with the increase in LV mass and because extravascular compression of the coronary vasculature is increased. In addition to these factors, an increase in coronary vasomotor tone, secondary to neurohumoral activation and endothelial dysfunction, could also contribute to the impaired myocardial oxygen supply. Consequently, we explored, in a series of studies, the alterations in regulation of coronary resistance vessel tone in remodelled myocardium of swine with a 2 to 3-week-old MI. These studies indicate that myocardial oxygen balance is perturbed in remodelled myocardium, thereby forcing the myocardium to increase its oxygen extraction. These perturbations do not appear to be the result of blunted beta-adrenergic or endothelial NO-mediated coronary vasodilator influences, and are opposed by an increased vasodilator influence through opening of K(ATP) channels. Unexpectedly, we observed that despite increased circulating levels of noradrenaline, angiotensin II and endothelin-1, alpha-adrenergic tone remained negligible, while the coronary vasoconstrictor influences of endogenous endothelin and angiotensin II were virtually abolished. We conclude that, early after MI, perturbations in myocardial oxygen balance are observed in remodelled myocardium. However, adaptive alterations in coronary resistance vessel control, consisting of increased vasodilator influences in conjunction with blunted vasoconstrictor influences, act to minimize the impairments of myocardial oxygen balance.
Figures







References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

