Long-term effects on medical costs of improving depression outcomes in patients with depression and diabetes
- PMID: 18332158
- PMCID: PMC3810023
- DOI: 10.2337/dc08-0032
Long-term effects on medical costs of improving depression outcomes in patients with depression and diabetes
Abstract
Objective: The purpose of this study was to examine the 5-year effects on total health care costs of the Pathways depression intervention program for patients with diabetes and comorbid depression compared with usual primary care.
Research design and methods: The Pathways Study was conducted in nine primary care practices of a large HMO and enrolled 329 patients with diabetes and comorbid major depression. The current study analyzed the differences in long-term medical costs between intervention and usual care patients. Participants were randomly assigned to a nurse depression intervention (n = 164) or to usual primary care (n = 165). The intervention included education about depression, behavioral activation, and a choice of either starting with support of antidepressant medication treatment by the primary care doctor or problem-solving therapy in primary care. Interventions were provided for up to 12 months, and the main outcome measures are health costs over a 5-year period.
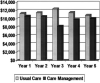
Results: Patients in the intervention arm of the study had improved depression outcomes and trends for reduced 5-year mean total medical costs of -$3,907 (95% CI -$15,454 less to $7,640 more) compared with usual care patients. A sensitivity analysis found that these cost differences were largely explained by the patients with depression and the most severe medical comorbidity.
Conclusions: The Pathways depression collaborative care program improved depression outcomes compared with usual care with no evidence of greater long-term costs and with trends for reduced costs among the more severely medically ill patients with diabetes.
Figures
References
-
- Anderson RJ, Freedland KE, Clouse RE, Lustman PJ. The prevalence of comorbid depression in adults with diabetes: a meta-analysis. Diabetes Care. 2001;24:1069–1078. - PubMed
-
- Ludman EJ, Katon W, Russo J, Von Korff M, Simon G, Ciechanowski P, Lin E, Bush T, Walker E, Young B. Depression and diabetes symptom burden. Gen Hosp Psychiatry. 2004;26:430–436. - PubMed
-
- Von Korff M, Katon W, Lin EH, Simon G, Ludman E, Oliver M, Ciechanowski P, Rutter C, Bush T. Potentially modifiable factors associated with disability among people with diabetes. Psychosom Med. 2005;67:233–240. - PubMed
-
- Lin EH, Katon W, Von Korff M, Rutter C, Simon GE, Oliver M, Ciechanowski P, Ludman EJ, Bush T, Young B. Relationship of depression and diabetes self-care, medication adherence, and preventive care. Diabetes Care. 2004;27:2154–2160. - PubMed
-
- Black SA, Markides KS, Ray LA. Depression predicts increased incidence of adverse health outcomes in older Mexican Americans with type 2 diabetes. Diabetes Care. 2003;26:2822–2828. - PubMed