Rapid subcutaneous immunoglobulin administration every second week results in high and stable serum immunoglobulin G levels in patients with primary antibody deficiencies
- PMID: 18341618
- PMCID: PMC2384102
- DOI: 10.1111/j.1365-2249.2008.03620.x
Rapid subcutaneous immunoglobulin administration every second week results in high and stable serum immunoglobulin G levels in patients with primary antibody deficiencies
Abstract
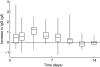
Subcutaneous immunoglobulin G (SCIG) infusions as life-long replacement therapy in patients with primary antibody deficiences (PAD) is being applied increasingly. However, only a few published pharmacokinetic studies are available for this route of administration. Therefore, the pharmacokinetics of a 16% immunoglobulin G (IgG) preparation intended for subcutaneous use were investigated in patients with common variable immunodeficiency and X-linked agammaglobulinaemia. SCIG infusions (200 mg/kg body weight) were administered to 12 adult patients every 14 days for 24 weeks (total of 144 infusions). Pharmacokinetic parameters were determined based on serum IgG trough levels and antibody levels against tetanus. The median half-life of the total serum IgG and for the tetanus antibodies was 40.6 and 23.3 days respectively. Median in vivo recovery of serum IgG and tetanus immunoglobulins were 36% and 46% respectively. Median, preinfusion serum IgG trough levels per patient were high without major variations between infusions and ranged from 7.24 to 7.86 g/l. Safety, in terms of adverse events including systemic adverse reactions and local tissue reactions at infusions sites, was monitored throughout the study. Six mild, local tissue reactions were observed during the study in one patient. No systemic adverse reactions related to the study drug were observed and no serious other adverse event occurred during the study. It is concluded that the bi-weekly SCIG therapy was well tolerated in the study and that it results in high and stable serum IgG levels, offering an alternative therapy regimen to patients suffering from PAD.
Figures

Similar articles
-
Efficacy and safety of Hizentra(®) in patients with primary immunodeficiency after a dose-equivalent switch from intravenous or subcutaneous replacement therapy.Clin Immunol. 2011 Oct;141(1):90-102. doi: 10.1016/j.clim.2011.06.002. Epub 2011 Jun 12. Clin Immunol. 2011. PMID: 21705277 Clinical Trial.
-
Subcutaneous immunoglobulin replacement in patients with primary antibody deficiencies: safety and costs.Lancet. 1995 Feb 11;345(8946):365-9. doi: 10.1016/s0140-6736(95)90346-1. Lancet. 1995. PMID: 7845120 Clinical Trial.
-
Rapid subcutaneous IgG replacement therapy is effective and safe in children and adults with primary immunodeficiencies--a prospective, multi-national study.J Clin Immunol. 2006 Mar;26(2):177-85. doi: 10.1007/s10875-006-9002-x. Epub 2006 Apr 26. J Clin Immunol. 2006. PMID: 16758340 Clinical Trial.
-
Intravenous and subcutaneous immunoglobulin G replacement therapy.Allergy Asthma Proc. 2016 Nov;37(6):426-431. doi: 10.2500/aap.2016.37.3987. Allergy Asthma Proc. 2016. PMID: 27931296 Review.
-
Immunoglobulin treatment for primary antibody deficiencies: advantages of the subcutaneous route.BioDrugs. 2007;21(2):105-16. doi: 10.2165/00063030-200721020-00005. BioDrugs. 2007. PMID: 17402794 Review.
Cited by
-
II Brazilian Consensus on the use of human immunoglobulin in patients with primary immunodeficiencies.Einstein (Sao Paulo). 2017;15(1):1-16. doi: 10.1590/S1679-45082017AE3844. Einstein (Sao Paulo). 2017. PMID: 28444082 Free PMC article.
-
Clinical immunology review series: An approach to the management of pulmonary disease in primary antibody deficiency.Clin Exp Immunol. 2009 Feb;155(2):147-55. doi: 10.1111/j.1365-2249.2008.03851.x. Clin Exp Immunol. 2009. PMID: 19128358 Free PMC article. Review.
-
Treatment with Hizentra in patients with primary and secondary immunodeficiencies: a real-life, non-interventional trial.BMC Immunol. 2016 Sep 29;17(1):34. doi: 10.1186/s12865-016-0169-5. BMC Immunol. 2016. PMID: 27687879 Free PMC article.
-
Subcutaneous Immunoglobulin 16.5% (Cutaquig®) in Primary Immunodeficiency Disease: Safety, Tolerability, Efficacy, and Patient Experience with Enhanced Infusion Regimens.J Clin Immunol. 2023 Aug;43(6):1414-1425. doi: 10.1007/s10875-023-01509-4. Epub 2023 May 9. J Clin Immunol. 2023. PMID: 37160610 Free PMC article.
-
Subcutaneous immunoglobulin: opportunities and outlook.Clin Exp Immunol. 2009 Dec;158 Suppl 1(Suppl 1):51-9. doi: 10.1111/j.1365-2249.2009.04027.x. Clin Exp Immunol. 2009. PMID: 19883424 Free PMC article. Review.
References
-
- Eibl MM, Wedgwood RJ. Intravenous immunoglobulin: a review. Immunodef Rev. 1989;1(Suppl.):1–42. - PubMed
-
- Gardulf A. Immunoglobulin treatment for primary antibody deficiencies: advantages of the subcutaneous route. Biodrugs. 2007;21:105–16. - PubMed
-
- Gardulf A, Hammarström L, Smith CIE. Home treatment for hypogammaglobulinaemia with subcutaneous gammaglobulin by rapid infusion. Lancet. 1991;338:162–6. - PubMed
-
- Gardulf A, Andersen V, Björkander J, et al. Subcutaneous immunoglobulin replacement in patients with primary antibody deficiencies: safety and costs. Lancet. 1995;345:365–9. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

