Both preoperative perinuclear antineutrophil cytoplasmic antibody and anti-CBir1 expression in ulcerative colitis patients influence pouchitis development after ileal pouch-anal anastomosis
- PMID: 18378498
- PMCID: PMC2742560
- DOI: 10.1016/j.cgh.2008.01.002
Both preoperative perinuclear antineutrophil cytoplasmic antibody and anti-CBir1 expression in ulcerative colitis patients influence pouchitis development after ileal pouch-anal anastomosis
Abstract
Background & aims: Acute pouchitis (AP) and chronic pouchitis (CP) are common after ileal pouch-anal anastomosis (IPAA) for ulcerative colitis. The aim of this study was to assess associations of preoperative perinuclear antineutrophil cytoplasmic antibody (pANCA) and anti-CBir1 flagellin on AP or CP development.
Methods: Patients were assessed prospectively for clinically and endoscopically proven AP (antibiotic responsive) or CP (antibiotic-dependent or refractory to antibiotic therapy). Sera from 238 patients were analyzed for ANCA and anti-CBir1 using an enzyme-linked immunosorbent assay. pANCA(+) patients were substratified into high-level (>100 EU/mL) and low-level (<100 EU/mL) groups.
Results: After a median follow-up period of 47 months, 72 patients (30%) developed pouchitis. Pouchitis developed in 36% of pANCA(+) patients versus 16% of pANCA(-) patients (P = .005), 46% of anti-CBir1(+) patients versus 26% of anti-CBir1(-) patients (P = .02), and 54% of 35 pANCA(+)/anti-CBir1(+) patients versus 31% of 136 pANCA(+)/anti-CBir1(-) patients (P = .02). AP developed in 37 pANCA(+) patients (22%) versus 6 pANCA(-) patients (9%) (P = .02), and 12 anti-CBir1(+) patients (26%) versus 31 anti-CBir1(-) patients (16%) (P = .1). Although AP was not influenced by pANCA level, AP was seen in 38% of low-level pANCA(+)/anti-CBir1(+) patients versus 18% low-level pANCA(+)/anti-CBir1(-) patients (P = .03). CP was seen in 29% of high-level pANCA(+) patients versus 11% of low-level pANCA(+) patients (P = .03).
Conclusions: Both pANCA and anti-CBir1 expression are associated with pouchitis after IPAA. Anti-CBir1 increases the incidence of AP only in patients who have low-level pANCA expression, and increases the incidence of CP only in patients who have high-level pANCA expression. Diverse patterns of reactivity to microbial antigens may manifest as different forms of pouchitis after IPAA.
Figures


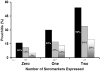
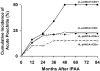
 ) development (p trend=0.007) but not chronic pouchitis (
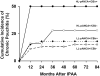
) development (p trend=0.007) but not chronic pouchitis ( ) development (p trend=0.05) with increasing seromarker positivity. Zero, one or two represents number of seromarkers expressed. Patient numbers are italicized along the x axis.
) development (p trend=0.05) with increasing seromarker positivity. Zero, one or two represents number of seromarkers expressed. Patient numbers are italicized along the x axis.
References
-
- Meagher AP, Farouk R, Dozois RR, Kelly KA, Pemberton JH. J ileal pouch-anal anastomosis for chronic ulcerative colitis: complications and long-term outcome in 1310 patients. Br J Surg. 1998;85:800–3. - PubMed
-
- Shepherd NA, Hulten L, Tytgat GNJ, et al. Workshop: Pouchitis. Int J Colorectal Dis. 1989;4:205–29. - PubMed
-
- Kuisma J, Mentula S, Luukkonen P, et al. Factors associated with ileal mucosal morphology and inflammation in patients with ileal pouch-anal anastomosis for ulcerative colitis. Dis Colon Rectum. 2003;46:1476–1483. - PubMed
-
- Madden MV, McIntyre AS, Nicholls RJ. Double-blind crossover trial of metronidazole versus placebo in chronic unremitting pouchitis. Dig Dis Sci. 1994;39:1193–96. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

